| When is a C-section performed? |
| Risks of a caesarean section |
| The benefits of having a planned caesarean |
| Preparing for a C-section |
| What to expect during a c-section |
| There are generally three different types of anaesthesia that are available |
| C-section surgery |
| Recovering from a C-section |
A caesarean, also commonly known as a C-section or surgical birth (1) is a surgical procedure during which a baby is baby is born via two surgical incisions (cuts) that are made in the abdomen and uterus by the doctor delivering the baby.
For some women a c-section is an elective procedure that they discuss with their doctor and opt for prior to the baby’s delivery. In other instances, a C-section is unplanned and performed as an emergency procedure when a baby cannot be delivered naturally for some reason.
As such, regardless of the type of birthing plan you’re hoping to have and have planned for so meticulously, it’s important that you don’t dismiss the idea of a possible C-section, especially in the event of such an emergency.
While a caesarean is a major type of surgery, it doesn’t necessarily have to be a completely negative experience, even if it wasn’t your first choice. Being well informed and prepared for this type of operation, whether you elect to have it or not, may assist in making the surgery less frightening and will aid in the recovery process. This article will give you insight into what to expect before, during and after this type of surgery.
When is a C-section performed?
Birth is a natural biological function and natural birth has a number of benefits for both mother and child, as such, medical intervention is generally intended only for when it is absolutely necessary. However, most gynaecologists and medical professionals will respect a woman’s right to choose what it best for her body and only insist on a c-section in situations where it is medically necessary.
Elective C-section
In some countries, women are given the option to elect to have a c-section for non-medical reasons, the primary of which are convenience and the reduction of anxiety (although the reduction of maternal anxiety is often considered a medical reason).
With a c-section, the baby’s birth date and approximate time of birth can be planned prior to delivery. This can help to take the ‘unknown’ and anxiety out of a baby’s arrival and prevent the soon-to-be parents and doctors having to visit the hospital in the middle of the night.
Women who have heard the awful natural birth tales that inevitably seem to circulate amongst family, friends and colleagues, often become fearful and opt for a c-section to avoid the long, painful, traumatic birthing process they’ve heard about.
Then there are those who are worried about how natural birth will affect their body and sex life and as such, opt for a c-section to ensure that everything ‘down there’ stays just the way it was before. While one may note some differences in the way things feel in the early months after natural birth, long-term studies show that there is no relation between delivery types and sexual function in women. (2)
Medical reasons for a C-section
Your doctor may suggest a caesarean section as opposed to giving birth naturally if you have a pre-existing health condition that necessitates, or if you’ve experienced some issues and complications during pregnancy or in previous pregnancies.
At times, it may become apparent to your doctor during the natural birthing process that a caesarean is medically necessary in order to minimize potential risks for both you as the mother and your unborn baby.
Some of the medical reasons to perform a c-section are:
- If the baby is in a breach position (i.e. feet first instead of head first) and cannot be turned which may result in making a natural delivery unlikely.
- The pelvis is too small which would make a vaginal birth highly impossible
- Maternal congenital abnormalities (i.e. abnormalities formed before birth) such as a deformed pelvis
- Eclampsia (convulsions) as well as HELLP syndrome (haemolysis (i.e. the rupture or destruction of blood vessels), elevated liver enzyme levels, and low platelet levels) as a result of pre-eclampsia which is a condition characterised by high blood pressure during pregnancy. If not managed and treated correctly, these complications can be life-threatening.
- Placenta previa – occurs when the placenta covers -a woman’s cervix either partially or completely.
- Foetal hypoxia – the oxygen supply to the unborn child is compromised.
- Prolapse of the umbilical cord - This is when the umbilical cord drops into the vagina through the open cervix in front of the baby. This may result in the cord being caught against the body of the baby during the time of delivery.
- Amniotic infection syndrome: Medically termed Chorioamnionitis, while rare, this condition can cause an infection of the placenta and possibly the foetus, and result in the need for an immediate delivery.
- Uterine rupture – tearing of the uterus that can occur in late pregnancy or during labour. This can occur along healed scar lines in those who have delivered previous pregnancies via c-section.
- Failure to progress in labour - If delivery is delayed or labour ceases, a c-section may be required to protect against adverse foetal outcomes.
- Previous caesarean - It is widely assumed that having a previous c-section makes it impossible to have a vaginal delivery in any pregnancies that follow due to the risk of uterine rupture. This, however, is not always the case, and some doctors will be willing to discuss the possibility of having a vaginal birth after a caesarean (VBAC) based on whether or not you meet certain criteria (discussed later in the article). (3)
Risks of a caesarean section:
For you:
A caesarean is a major surgery and with it comes possible risks that you should be aware of which include: (4)
- Unfavourable reactions to prescribed medications including the aesthetic
- An excessive amount of bleeding which may result in you needing a blood transfusion.
- Recovery time is longer than that of a vaginal delivery
- Post-partum Infection in the wound which may result in swelling, increased pain, redness and discharge from the incision.
- An infection in the lining of your uterus which can cause excessive vaginal bleeding, fever and pain.
- Blood clot/s also known as DVT (Deep vein thrombosis) in your legs which causes swelling and can be extremely dangerous if it moves towards your lungs causing a pulmonary embolism (when arteries in the lungs become blocked).
- Injuries to organs such as your bowels and bladder
- Possible complications with future pregnancies
For your baby (5)
- Nicking the infant’s skin which may occur accidentally when your womb is opened up.
- Your baby may experience difficulty breathing which is common in infants being born prior to 39 weeks. The baby will be monitored in hospital and taken care of until this is resolved.
The risks of a caesarean versus a vaginal birth (6)
The following risks are reduced by c-sections
- Abdominal and perineal pain (pain in the peritoneum – the fleshy area between the anus and vagina) in birth
- Abdominal and perineal pain three days following birth
- Injuries to the vagina
- Adverse reactions to anaesthesia such as bleeding and shock
The following risks were reduced after a vaginal delivery
- The length of stay in hospital
- Having a hysterectomy performed due to bleeding postpartum
- Heart attack (also known as cardiac arrest)
The benefits of having a planned caesarean
The major benefits of having a planned c-section largely relate to eliminating the unknown and the fear and anxiety that go with this. Still, a balanced view needs to be considered, because a caesarean is a major surgery and not the ‘easy’ alternative to natural birth. It is also not risk free.
Some benefits include:
- You as a parent will know the exact date as to when your baby will enter the world. This makes planning a lot easier in terms of finalizing any work requirements and arranging help at home for when you bring your baby home.
- It minimizes some of the potential health risks to both you and your child in certain circumstances.
- The risk of post-term pregnancy (when the natural due date is exceeded) can be avoided.
- Your obstetrician will be booked in advance and readily available for that day, this can go a long way to reduce anxiety.
- There are hardly any unknowns such as how long you could possibly be in labour for, for many women this reduces anxiety.
- Reducing the risk of injury to the pelvic muscles and tissues, and anal sphincter (muscle found at the bottom of the rectum that encircles the anus and aids in the discharge and retention of stools) (7)
Preparing for a C-section
Being prepared for a c-section if you or your doctor is scheduling one, or for the chance that you may need one, even if you’re planning a natural birth, can help to take the fear and anxiety out of the whole procedure. Here are a few tips on packing for your hospital stay either way.
Packing for your hospital stay
For peace of mind, it’s generally a good idea to have your own hospital bag as well as your baby’s packed and ready to go during your third trimester.
Here’s a list of suggested items:
Expectant mothers:
- Your ID / drivers licence for your hospital admission
- Any medical records / history that the hospital needs to be made aware of
- Your purse with some cash (in the event that you feel like a late night snack from the café)
- A couple of pairs of loose fitting dark coloured pyjamas (to hide any stains), preferably with a buttoned top if you are breastfeeding.
- Maternity pads – you will bleed after your C-section (these pads are way thicker than normal sanitary pads and will be necessary for at least a few days post-op and then you may find you can switch to your normal brand). You will not be able to use tampons as in addition to the discomfort experienced, there is an increased risk of developing an infection.
- Extra pairs of underwear (tip – make sure the elastic waistband isn’t too tight as it may end up hurting your wound area)
- Toiletries such as your toothbrush, toothpaste, hairbrush and ties, deodorant, shampoo and conditioner, lip balm and hand cream. Towels for your shower
- Comfortable footwear with a grip so that you don’t slip
- A few pairs of nursing bras.
- Nursing pads to soak up any leakage
- A wrap or nursing cover, in the event you need to feed your child in front of people.
- Nipple cream – if you are breastfeeding, you may find that your nipples will crack and become rather painful. Applying breast / nipple cream may alleviate the discomfort.
- A breast pump – your milk supply may come in the same day, but if there are any issues with feeding, you may need to express. The hospital may have these on hand, but it’s advisable to bring one with you just in case.
- A comfortable outfit for the day you’re discharged and ready to take your baby home
For your baby
- A couple of pairs of onesies that have built in socks at the bottom
- Newborn vests
- Baby beanies or caps
- New born diapers / nappies
- Bum cream to prevent diaper / nappy rash
- Talcum powder (if you intend on using it) to apply to your baby one he/she is completely dry.
- You will have to swaddle your new baby and so bring along a few receiving blankets that will keep your little one snug and warm.
- Enough bibs and wash cloths
- A dummy to soothe your little one when needed
- An outfit for the day he/she gets to go home
- Also ensure that you have an infant car seat which must already be fitted in the vehicle you will both be transported home in and ready to use
What to expect during a c-section
Admission and prior arrangements
If your c-section is scheduled, you will be required to fill in all hospital admission and doctors release forms. This may be arranged in advance or done on the day of admission. Try to get as much done in advance as possible so that your day of admission is as calm as possible.
Ensure that you are aware of all costs and/or deposits required (as is applicable to your country of residence) so that you can make arrangements to pay for these in advance to avoid surprises.
In addition, depending on the doctor and/or hospital that you attend you may be given medications (often anti-acid and anti-sickness tablets) to be taken the night before and on the morning of your surgery.
At home
Your doctor may request that you wash with antiseptic soap the night before and morning of the procedure. Any removal of pubic hair should be done more than 24 hours before the procedure to reduce the risk of infection.
This type of grooming may be a tricky task in the later stages of pregnancy but if you prefer to do this yourself, a magnifying mirror may help you get the job done prior to your hospital admission. Alternatively, you can enlist your partner’s help or book a wax in advance.
Before surgery
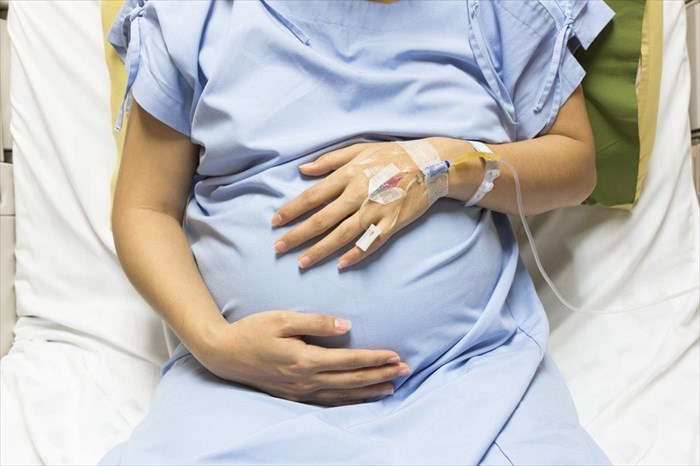
Once you have been admitted, you will be shown to your room and given a hospital gown to change into.
While you’re waiting, a nurse will set you up with a drip (IV) in order for you to receive intravenous fluids. This will enable your doctor and nurses to administer the relevant anaesthesia and medication that you require.
You will be asked whether you have shaved / clipped your pubic hair or if you will require assistance from a nurse. Having a shaved/clipped pubic area will ensure that your gynaecologist / doctor can easily make the relevant incision in the pubic area without any obstructions.
Your anaesthesiologist will generally pop in to ask you a few questions about your health, weight and history of anaesthesia as well as discuss the procedure and how the epidural (a form of anaesthesia that stops pain) will be administered.
Inside the waiting area and operating room
You will be wheeled through into theatre or in some hospitals, into a side waiting room while your partner is given a set up scrubs and a facial mask to change into while they wait. This is a standard requirement and to minimize the risk of infection.
You may find that these rooms are exceptionally cold.(8) This is to avoid any problems with temperatures that may affect the anaesthetic equipment causing it to overheat, as well as to keep nursing staff and doctors who are in long sterile gowns and working in front of hot lights comfortable.
C-section anaesthesia
The next step is for the anaesthesiologist to administer the anaesthesia that will be used to prevent pain during the surgery.
There are generally three different types of anaesthesia that are available: (9)
Epidural / spinal epidural
This form of local anaesthesia is commonly used for caesarean and vaginal deliveries. Epidurals prevent pain during these procedures by blocking nerve impulses.
What to expect when getting an epidural
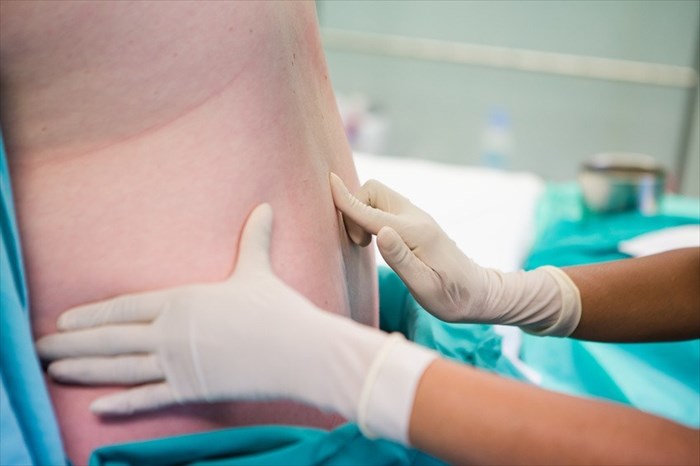
If you’re having an epidural, an anti-septic solution to reduce the risk of infection will then be applied to your back, this is often quite cold so brace yourself! You will then be asked to sit on the edge of the bed or lie on your left side and arch your back to open up the spaces between the bones of the spine and remain completely still.
A local anaesthetic to numb the area will then be injected into the skin of the back, this may sting a little. Next a needle will then be inserted into the spinal area of the lower back, this should not be painful but may give a feeling or pressure or aching. A small tube (catheter) will then be inserted and left in the back. Anaesthesia and medication are administered through this throughout the procedure.
If you aren’t already, you will be asked to lie down. You may begin to feel some warmth, tingling or pins and needles in your bottom and legs. Your legs will feel heavy and difficult to move. Do not panic, this is normal.
Side effects are rare, which is why this is a commonly used form of anaesthetic.
Spinal block
A spinal block, also referred to as a ‘spinal’ is different from an epidural in that the injected narcotic and/or anaesthetic is injected into the spinal fluid once, using a needle, whereas the epidural involves the insertion of a catheter for continuous infusion.
Spinal blocks generally provide pain relief for 2 hours. They are administered in much the same manner as an epidural, with the exception that the catheter (tube is not inserted).
General anaesthesia
General anaesthesia used to be the only option available for caesarean deliveries prior to the development of spinal blocks and epidurals. These days, this form of anaesthesia is often reserved for situations that arise during a standard c-section that require emergency intervention and the patient in question to be fully sedated in a deep sleep where no pain will be felt, and the procedure not remembered afterwards.
Catheterisation
Once the appropriate anaesthesia has been administered, a urinary catheter will be inserted. This is to assist in emptying your bladder and ensure that you do not urinate during surgery.
Operating room preparations
If you were in a side room for the administration of the anaesthesia, you will be wheeled into the operating room. If the anaesthesia was administered in theatre, you will remain lying down while a sterile drape / curtain is pinned up across the middle of your abdomen in order to prevent you from being able to view the physical surgery. However, some hospitals (or doctors), when asked, may allow you to have the drape lowered in order for you to view the last steps of delivery and your baby being brought into the world while taking his / her first breath.
Once everything is in order, your partner will be brought in to be with you and may, with permission, be permitted to take photographs.
C-section surgery
The surgeon will begin by making an incision in your lower abdomen. Due to the anaesthesia, you will not be able to feel this. The surgery will proceed as follows:
- An abdominal incision will be made
Your skin is so thin, and the scalpel is so sharp that your layer of fat beneath your skin will almost instantly be exposed. From there a smaller section of this layer of fat will be cut until the fascia (tough connective tissue comprised mostly of collagen that separates, encloses and stabilizes your muscles and various other internal organs) is found below it. A small incision will be made in the fascia in order to expose your rectus abdominal muscles, otherwise commonly referred to as your ‘abs’. These particular muscles move above from your abdomen and then down to your pubic bone area. These muscles are joined at the midline and can be easily seen when your doctor cuts into the fascia on either side. Your doctor will then gently push these muscles apart where they meet in order to separate them. This in turn will then expose the peritoneum (the abdominal cavity lining). The peritoneum is so thin and fragile that your doctor will carefully cut it open, it has a film like appearance and your bowels can be seen beneath it.
A retractor is then used to pull the lowest part of the peritoneum down towards your feet preparing your body for the next step.
- Next a uterine incision will be made
Your womb (uterus) has another film-like layer lying over it and a small incision is made in order to spread it on either side (horizontally). Your uterus will now be exposed, and an incision will be made on the lower part of your womb (or elsewhere, depending on the baby’s position). Your baby’s head will then be visible to your doctor.
During the procedure, you may feel pressure, pulling, pushing and a sensation that can be likened to someone rummaging around in your abdomen. This may seem strange but is not painful. Your anaesthesiologist will keep a close eye on your stats throughout the entire surgery and chat to you from time to time. Feel free to tell him/her if anything feels unusual, if you feel dizzy, nauseous or experience anything else out of the ordinary. Feeling dizzy or nauseous is often due to a drop in blood pressure due to the epidural and there are medications that can be given to counteract this.
- Delivery
Once the final incision has been made, it’s time for your baby to be positioned. You will probably feel a lot of painless tugging, pulling and prodding which is your doctor and nursing staff busy aligning the baby in such a way in order to get hold of the baby’s head to cradle and pull the baby out. Due to the fact that you are basically immobilized and unable to push, your doctor will push the top area of your uterus and lift up your baby’s head from the pelvis, and the shoulders and the rest of the body will follow.
The doctor will clear fluid from your baby’s nose and mouth, clamp and cut the umbilical cord. Most of the time, you will get a brief moment to see your little one before he/she is taken to be cleaned, weighed and assessed. In the assessment an APGAR test will be conducted. APGAR (10) stands for:
- Appearance (checking the skin colour)
- Pulse (checking the heart rate)
- Grimace (checking reflexes)
- Activity (checking muscle tone)
- Respiration (checking the breathing rate and effort)
Final steps
The placenta will be removed from your uterus and the incisions made will be closed up using sutures (stitches). If all is fine with your baby, he/she may be given to you to enjoy some skin-to-skin time as this is done.
Depending on your particular circumstances, the entire process from start to finish is roughly 30 minutes.
You will then be placed into a recovery room in order to have your vitals monitored You may be given a suppository for pain at the end of the surgery or pain medication will be administered thereafter (this may be done via the epidural port which is often left in place for a few hours).
Recovering from a C-section
Generally, you will be in hospital for 3 nights and 4 days following your surgery. You will be transferred to your postpartum hospital room and you will initially receive pain medication through your IV which will then be switched to medication which can be taken orally. Usually the anaesthetic will wear off within three hours after your operation and your nurses will encourage you to start walking and moving around within the first 6 hours of your surgery. This is to help prevent any possible blood clots and the build-up of gas in your abdomen. This may be challenging as your body has been through a lot. Be prepared and take things slowly.
Taking a walk to have a shower will also be encouraged by the nurses. Do not scrub your abdomen and incision area, simply let the soapy water run over it and pay dry once you are done. You may require assistance from hospital staff getting dressed as you may not be able to bend over at this time. You will experience heavier bleeding than you do during your monthly period. This requires a maternity pad (a longer, thicker pad specifically designed for heavier bleeding) and mesh underwear to keep it in place.
As the heavy bleeding gradually subsides over the following week you may switch to normal sanitary pads that are more comfortable and less bulky. Don’t be alarmed by the amount of blood you see, it’s completely normal to experience heavier bleeding than your period. It will also look different and is medically referred to as lochia (vaginal discharge containing mucus, blood as well as uterine tissue matter). This also occurs in vaginal birth deliveries as well.
As soon as you are feeling up to it, you may eat and drink something light. Your nurses may give you a stool softener to take to help you as you may not experience regular bowel movements straight after your operation. Drinking plenty of water and eating food that is high in fiber may also help to regulate your bowel.
The ability to laugh, cough, sneeze or even get up and off the toilet will be a mammoth task to begin with but you’ll modify your capabilities and adapt. If you feel the need to sneeze or even cough, it is recommended that you use a pillow to hold over your tummy / incision or invest in a pregnancy belt to give you that added support. Each woman will experience symptoms and degrees of pain or discomfort differently and as the days pass, these should improve. It is highly recommended that for the next couple of weeks following your surgery that you rest and take things slowly.
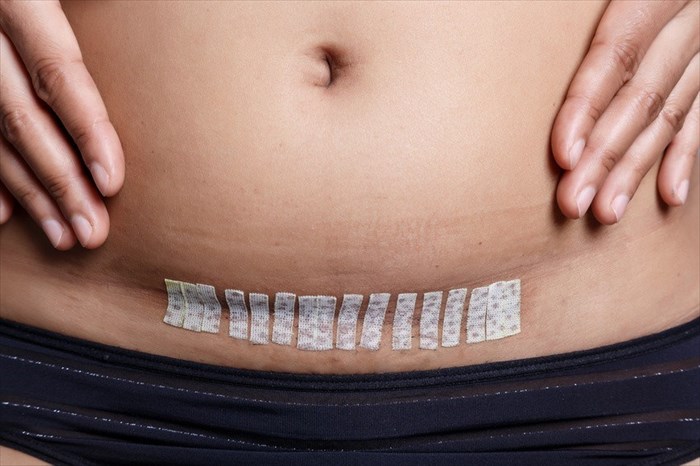
If you have had staples inserted to close the outer incision, these are usually removed within three and seven days of your delivery. However, if dissolvable sutures were used, they are absorbed and dissolved by the body and it’s not necessary to have them removed.
During your recovery process, you may continue to experience mild to moderate cramping, slight bleeding and even vaginal discharge. You may use a sanitary pad or a panty liner to ease the discomfort.
Also keep in mind that even after the staples or stitches are removed/dissolve, it is completely normal for your incision to be sensitive and painful or for some numbness to be experienced around that area.
Before you are discharged from hospital, your doctor will give you some post-operative advice which may include the following: (11)
- Refrain from any major physical activities and demanding exercises.
- Do not lift any heavy items
- Avoid placing anything inside your vagina such as tampons until 4-6 weeks after surgery
- Sex is to be avoided until you receive the all clear from your physician 4-6 weeks post-partum.
- Rest as much as possible
- Keep hydrated
- Take your pain medications as prescribed
- Wear a pregnancy belt or use a pillow as a form of support for your abdominal area
- It is recommended that you do not to drive 4-6 weeks after surgery
Your incision will take approximately six weeks to heal. You will be left with a scar but over time and with proper care this will gradually fade. You may find that the area around your scar is numb and there is no sensation but feeling will come back as time passes.
Vaginal birth after caesarean (VBAC) (12)
Things may not have gone as planned with the birth of your child, whether it be your first, second or even third. You had planned a natural vaginal birth only to end up requiring a caesarean in order to protect you and your unborn child. This can be rather upsetting to most mothers. If you’ve had a C-section it doesn’t mean that you cannot have a vaginal birth in future pregnancies.
Do you qualify for a VBAC?
The following criteria are considered when determining whether a woman can give natural birth after a previous c-section delivery:
- Overall health: You may not have an major health issues such as diabetes, troubles with blood pressure, or heart conditions.
- Health during pregnancy: You need to be healthy and have had a straightforward pregnancy.
- Foetal position: You baby may not be in a breeched position and must be in the head down position.
- No physical abnormalities or risks: There shouldn’t be any new scarring on your uterus, only the lower transverse caesarean scar. If you have a vertical C-section scar, a VBAC will not be possible. There is a possibility that the scar may burst (rupture) which may be exceptionally dangerous for both the mother and the child.
- Induction should not be required: Labour may not be induced and must take place on its own, naturally. If you exceed your natural due date without going into labour, a caesarean will be required.
Although a VBAC is possible for some women, it’s important to discuss this with your doctor in detail to ensure that you are fully aware of the risks.
References
1. US National Library of Medicine National Institutes of Health. 01 December 2013. Caesarean deliveries by Pfannestiel versus Joel-Cohen incision: A randomisted controlled trial: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3935539/ [Accessed 03.04.2019]
2. US National Library of Medicine National Institutes of Health. 25 March 2017. Long term effect of vaginal delivery and cesarean section on female sexual function in primipara mothers: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5407233/ [Accessed 03.04.2019]
3. American Pregnancy Association. August 2015. VBAX: Vaginal Birth after cesarean: https://americanpregnancy.org/labor-and-birth/vbac/ [Accessed 03.04.2019]
4. US National Library of Medicine National Institutes of Health. 25 July 2015. Indications for and Risks of Elective cesarean Section: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4555060/ [Accessed 03.04.2019]
5. NHS. 01 July 2016. Risks - Caesarean section: https://www.nhs.uk/conditions/caesarean-section/risks/ [Accessed 03.04.2019]
6. US National Library of Medicine National Institutes of Health. 20 July 2015. Indications for and Risks of Elective cesarean Section: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4555060/ [Accessed 03.04.2019]
7. US National Library of Medicine National Institutes of Health. 23 December 1993. Anal-sphincter disription during vaginal delivery: https://www.ncbi.nlm.nih.gov/pubmed/8247054 [Accessed 03.04.2019]
8. US National Library of Medicine National Institutes of Health. 20 October 1963. The control of operating-suite temperatures: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1038380/ [Accessed 03.04.2019]
9. US National Library of Medicine National Institutes of Health. September - October 2010. Anaesthesia for lower-segment caesarean section: Changing perspectives: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2991650/ [Accessed 03.04.2019]
10. US National Library of Medicine National Institutes of Health. 2000. Apgar scores: Examining the long-term signidicance: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1595023/ [Accessed 03.04.2019]
11. US National Library of Medicine National Institutes of Health. 2004. Recovery following caesarean section: https://www.ncbi.nlm.nih.gov/books/NBK115312/ [Accessed 03.04.2019]
12. US National Library of Medicine National Institutes of Health. 5 February 2013. Vaginal birth after cesarean section: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3624716/ [Accessed 03.04.2019]