How is appendicitis diagnosed?
If you suspect appendicitis, you must see a medical professional. There are no home-remedies that will be able to effectively treat this condition.
It can be tricky to diagnose as symptoms are fairly similar to a host of other conditions, such as a urinary tract infection, bladder problems, gastritis, intestinal infections, problems with the gallbladder, Crohn’s disease and ovary problems.
The presence of pain is a good indication to see your family physician and have a thorough check, no matter what the condition turns out to be. If you suspect appendicitis, ensure that you see your doctor as quickly as possible.
Questions your doctor may ask during your consultation include:
- How long ago did you start experiencing abdominal pain?
- Where specifically are you experiencing discomfort or pain?
- Would you describe the pain as mild or severe (unbearable)?
- Have you noticed that the pain has moved around your tummy area?
- Have you noticed any movements that seem to worsen the pain?
- Have you done anything to try and alleviate the pain? (i.e. taken a pain reliever)
- Do you feel feverish?
- Are you experiencing nausea and or/ vomiting?
- Aside from pain, is there anything else causing you to feel unwell?
What tests are involved in diagnosing appendicitis?
Following the discussion and a physical exam (applying gentle pressure to the area of discomfort), your doctor may recommend a series of tests in order to make a diagnosis.
Signs you doctor will look out for during the physical exam will be to check for what happens when pressure is suddenly released. Pain associated with appendicitis typically feels better under pressure and worse and somewhat tender when pressure is no longer applied. This indicates to your doctor that the peritoneum (serous membrane of the abdominal lining cavity) is infected or inflamed. He or she will also be on the lookout for other physical reactions to applied pressure. Your abdominal area may be rigid or swollen and when pressure is applied, you may stiffen your muscles. This is somewhat like a protective instinct where your body’s reaction to pressure is an attempt to ‘guard’ the affected area against further harm or pain.
Another part of your physical exam may involve a rectal exam. Your doctor may insert a gloved, and lubricated finger to examine your lower rectum. Your doctor may use their other hand to apply a little pressure on your lower abdomen or pelvic area at the same time. Males will experience a digital rectal exam which checks the prostate gland. For women, this process may also involve checks for any potential gynaecological or reproductive problems, which may be the underlying cause of the uncomfortable symptoms being experienced. While this procedure may seem embarrassing for the patient, it is routine for many doctors, administered quickly and with very minimal discomfort.
Tests to confirm a diagnosis may include the following:
- Blood samples: Samples of your blood will be drawn to check if your white blood cell count (CBC) is high. This typically happens as the body’s reaction to an infection. Your doctor may want to determine if there is a bacterial infection in the body. White blood cell counts are a good indicator of this as they increase to naturally help fight off the presence of an infection in the body.
- Urine test: Your doctor may recommend this test to try and rule out any other potential causes of pain, such as a kidney stone or a urinary tract infection.
- Imaging tests: An abdominal ultrasound, X-ray (of your abdomen area) or a CT scan may be recommended. These tests will provide your doctor with detailed images about what is happening on the inside of your body. These will be used to detect appendicitis and confirm a diagnosis or used as a way to see what other causes could be the underlying source of your symptoms, such as an abscess. If necessary, an X-ray of your chest can also be used to rule out the possibility of right lower lobe pneumonia.
- Pregnancy test: In odd instances, a doctor may recommend a pregnancy test to potentially rule out an ectopic pregnancy (if this is strongly suspected).
Appendicitis treatment and recovery
In most instances, a doctor will opt for surgery to treat appendicitis, especially if there are signs of rupture (perforation). Surgery typically happens quickly and you may be asked to book yourself into hospital right away. If your pain is minimal and diagnostic tests don’t show up any indications of further infection or complications, you may merely be prescribed antibiotics and asked to maintain a liquid diet for a short time while your symptoms are being monitored.
Surgery may depend on the nature of your particular diagnosis and circumstances. If your doctor feels it necessary to remove the appendix, an appendectomy procedure will be recommended straight away.
What happens during an appendectomy (appendix removal)?
Appendectomy: The procedure can be done in one of two ways – via a laparoscopy or open surgery. A laparoscopy involves a small camera and tiny surgical tools. The appendix will be reached via very few, small incisions. As a result, the procedure is less invasive for a patient, making recovery a little shorter. If it is noted via imaging tests that your appendix has ruptured or you have an abscess which has burst as well, open surgery is likely to be recommended. You may likely be given antibiotics before the procedure to try and fight further infection in the body. An abscess may be drained using a tube which is inserted through your skin, removing any fluid and pus. Open surgery will then take place to remove the appendix. The abdomen will be irrigated and drained of any infectious fluid and pus before you are stitched up and prepared for recovery.
- Post-surgery: You will need to be immobile for at least 12 hours following surgery and will remain in hospital. You may be able to start moving around a little after at least 12 hours. Your surgeon may keep you in hospital for 1 to 2 days post-op. Children may be kept in hospital a little longer to receive more antibiotics post-op via an intravenous line (IV) as they are at higher risk of possible infection following surgery. Normal daily activities can usually be resumed within 2 to 3 weeks (sometimes up to 6 weeks) post-op. Recovery time is considerably shortened if you have a laparoscopic procedure. You may experience less post-op pain and the scarring won’t be as bad. During recovery, you may experience some discomforts. If you experience a little dizziness, a fever, vomiting (uncontrolled), pain or inflammation at the site of incision, the presence of blood in urine or vomit, an increasing pain in your abdomen area, or pus in your healing incision wounds, call your doctor or surgeon as soon as possible.
Tips to help your child understand what happens during an appendectomy
The idea of being admitted to hospital for surgery can be as distressing for a child (even a little terrifying) as it can be for a parent. It can be rather difficult to explain to a child what he or she is about to go through.
In the case of a ruptured appendix, hospitalisation will be recommended immediately, leaving you with little time to explain the situation to your child.
Here are a few tips to help your child understand what is happening and alleviate as much worry as possible:
- Be mindful of your choice of words: “The doctor is going to cut you open …” is likely to cause unnecessary fear in your child. Choose your words carefully when you explain to your little one that they have a problem inside that the doctor is going to help fix for them. You don’t want to lie to your child either. There will come a point when the two of you will be separated. You will not be allowed in the operating theatre and your child will become aware at some point that you are not by their side to soothe any worries. Be honest, without painting a graphic picture, and causing unnecessary distress. Explain to your child that the medical staff and the doctor be with them the whole time, even if you aren’t, and will not leave him or her alone. Explain that you will be at his or her side the moment they wake up, setting a calming expectation your child can look forward to – a familiar, loving face, which makes them feel safe.
- Explain what the medical staff will do: Your child will need to be sedated and placed under general anaesthetic before the procedure. You will need to explain to the child that he or she won’t feel any pain while the doctor is helping to fix the problem. The doctor will give him or her something to help them sleep for the entire time needed to fix the problem. It is also important to let the child know that the doctor and their medical staff will also wake them up once they’ve fixed the problem. This is important if your child is familiar with “putting an animal to sleep”. They may associate their experience with an animal that won’t be waking up again and going home. This will be distressing for a child.
- Be nurturing: Once the ‘medical explanations’ are out of the way, it’s a good idea to revert to normal ‘mommy’ or ‘daddy’ mode and assure your child that what they’re about to go through is not a punishment for something they’ve done wrong. Reassure your child again that you will be waiting for them as soon as the doctor is finished fixing the problem and that once it is all done, they will begin to feel a lot better again soon. They might not feel better straight away, when they wake up, but they will start to feel better soon. Prior to surgery, if you can, provide some entertaining distractions for your child – a book, a toy or a little play with a family member. This will help to keep the child relatively calm and less aware of the foreign surroundings they find themselves in. These things can also be available for them as comforts when surgery is done and the recovery process in hospital begins. This helps calm a child and creates an expectation that something familiar and safe is waiting for them to come back.
Post-op home care after an appendectomy
Recovery will depend on the nature of your diagnosis and the type of appendectomy procedure your surgeon opted for. If your appendix (and or/ abscess) burst, you can expect to be recovering over a period of a few weeks (at least).
When you are discharged from hospital, and allowed home, there are some things you can do to help your body heal:
- Take things slow and steady: If you’re normally an active person, you’ll have itchy feet. It is important that you refrain from any strenuous activity at first (in some cases for up to 6 weeks). If you had an open appendectomy, you may need to take things easy for at least 10 to 14 days. If you had a laparoscopic procedure, you may need to rest for up to a week without activity. Your surgeon will explain your activity limitations immediately post-op and advise when you may be likely to be able to resume normal activity, and return to work or school. Take their advice. Your body will need to rest and recuperate.
- When feeling stronger, get up and move: It’s important that you gradually get moving again once you have regained a little more strength and pain or discomfort post-op begins to subside. Start slowly and increase your activity level at a gradual pace. A good start is by taking short walks.
- Rest: Your body has been through a trauma, and a double dose of it at that – the stress of infection and a surgery to correct it. You will get tired easily during the healing process. Rest when you need to and sleep when you’re tired. It’s one of the best ways to help build strength again and help you to heal.
- Take care: Recovery will bring with it some discomfort, particularly in the days following your surgery. You will experience some degree of pain. Your doctor will prescribe medications to help alleviate this. Pain typically causes the body more stress and will slow down the healing process. You will need to be aware of your movements and possibly need to support your abdomen when you laugh, cough or move. Placing a pillow over your abdomen with a little pressure before you laugh or cough can help to alleviate discomfort in this tender area as you heal. If you still experience pain despite taking pain medication, contact your doctor for a check.
- Switch up your diet for healthy healing: Another discomfort you may experience is constipation. This is temporary and not all that uncommon a side-effect post-op. You will need to stay well hydrated in the days following your op and consume foods that are rich in fibre to help your digestive system along. This will help regulate your bowel movements and ease the discomfort. Foods you can eat include lentils, split peas, black beans and artichokes, as well as foods with whole-wheat flour (pastas), brown rice, kidney beans, apples, pears, raspberries, broccoli, barley, and oatmeal. You can try eating breakfast cereals with yoghurt and a sprinkling of oat bran or wheat germ as well.

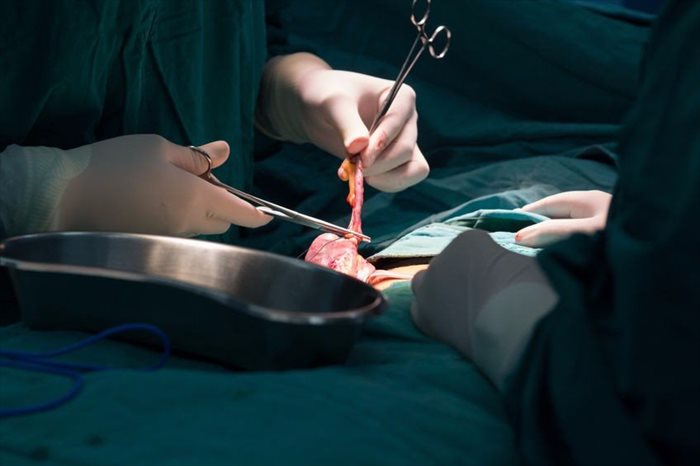
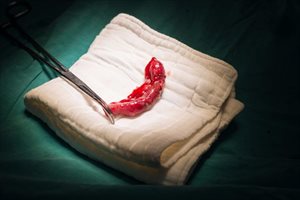 Appendectomy:
Appendectomy: