- Gum Disease (Gingivitis)
- What is the difference between gingivitis and periodontitis?
- What are the symptoms of gingivitis?
- What causes gingivitis?
- What are the risk factors and complications of gingivitis?
- How is gingivitis diagnosed and treated?
- Can gingivitis be prevented?
- How to practice good oral hygiene
- Some more information on gum disease
How is gingivitis diagnosed and treated?
How is gingivitis diagnosed?
Your dentist will typically diagnose gingivitis by:
- Reviewing your medical and dental history – This also includes investigating any current or past conditions or infections that may be contributing to your current symptoms.
- Examining your gums, teeth, tongue and mouth – This will be done to detect any signs of inflammation and plaque.
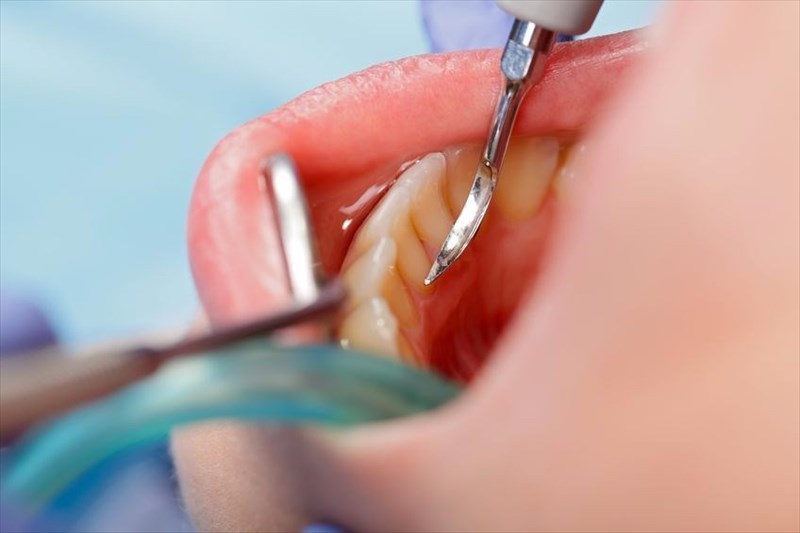
- Measuring your pocket depth – This is the groove between the teeth and gums. To examine this your dentist will insert a probe into your gum line (between your teeth and your gums) at a few different sites in your mouth. If you have a healthy mouth then the pocket depth will range from one to three millimetres (0.03 to 0.11 inches). If your pockets are deeper than four millimetres (0.16 inches), then this may indicate the presence of gum disease.
- Conducting dental X-rays – These will be conducted to examine your dental structure and detect if there is any bone loss in the areas your dentist has detected any deeper pockets.
- Performing any other tests that may be needed – If your dentist is unable to find a clear cause of gingivitis, then he or she may suggest that you have a medical evaluation done to detect any underlying health problems. If the gingivitis has advanced, then you may be referred to a periodontist (a doctor who specialises in gum disease), for a more thorough evaluation and treatment.
How is gingivitis treated?
In order for gingivitis to be treated effectively and for the outlook to be a positive one, it is best that you are treated promptly so as to prevent the condition’s progression and in turn the development of a more severe form of gum disease, tooth decay and potential tooth loss.
It is also best to stop the use of tobacco products and adopt a healthy regimen of good dental care to ensure that you have a higher chance of a full recovery.
The professional care for gingivitis includes the following:
- Dental cleaning – This will need to be done by your dentist or specialist who will remove all the plaque and tartar, as well as other bacterial products. This procedure is referred to as root planing or scaling. Scaling will remove the bacteria and tartar from the surfaces of your teeth, as well as any traces found under your gums. Root planing is a meticulous cleaning of the surfaces of your roots and will remove any bacterial products that are produced as a result of the inflammation. Root planing will also smooth the surfaces of the root, which will discourage any further build-up of bacteria or tartar as a smooth surface does not allow for the bacteria to latch onto the surface as easily. This will allow for the proper healing of the condition. Dental cleaning can be performed with dental instruments, an ultrasonic device or a laser.
- Restoring any dental fittings (if needed) – If there are any misaligned teeth, crowns that have been poorly fitted, as well as bridges or any other teeth restorations that may be irritating your gums or making it difficult for the plaque to be removed during dental care, then these need to be corrected and your dentist might suggest that he or she fix these issues to help rid your mouth of gum disease and prevent further infection.
- Ongoing care – A gum infection or inflammation will typically clear up once you have had a thorough cleaning by your dentist, coupled with practising dental and oral hygiene by brushing and flossing your teeth regularly. Your dentist may be able to assist you in putting together an effective routine and program to help you stick to keeping good care of your teeth. This plan will also include regular visits and check-ups with your dentist. When you are consistent with your oral hygiene, then you will be able to see your gum tissue return to a healthy state, being light pink in colour, in a number of weeks and in some cases, days.
What types of medication are used to treat gingivitis?
Your dentist will typically prescribe antibiotics to aid in eliminating the bacterial infection. Antibiotic therapy is often combined in a number of ways in assist in the treatment of gum disease. Types of gum disease and infections that make use of antibiotics for the treatment are:
- Gingivitis
- Periodontitis
- Trench mouth (ANUG - Acute Necrotizing Ulcerative Gingivitis) - This form of gum disease results in infected, bleeding and painful ulcerations and gums.
An antibiotic mouthwash known as Peridex (Chlorhexidine) is often prescribed. This assists in reducing the number of bacteria present in your mouth that contribute to the development of infection. In some cases, your dentist may give you small gels or pellets (PerioChip), that contain doxycycline or chlorhexidine. These are placed deep inside in the gum pockets once your dentist has conducted root planing or scaling, in order to eliminate the bacteria and also reduce the depth and size of the gum pockets caused by the infection.
The above-mentioned ways of administering antibiotics are extremely effective as the medications are slowly released over a period of seven days or more. You may also need additional pain medications such as NSAIDs (Nonsteroidal anti-inflammatory drugs) or xylocaine. These are commonly used in cases where the infection has progressed to ANUG (Trench Mouth) or chronic gingivitis.
What types of specialists treat gingivitis?
A periodontist is a dentist who has undergone additional training once they have completed dental school and specialised in diagnosing and treating disease of the bones, gums and teeth. If you have a more severe and advanced gingivitis infection, then you may be referred to a periodontist by your general dentist. Your dentist may first try to get rid of the tartar and plaque, after which you will see a specialist.
A periodontist may suggest a number of surgical or nonsurgical treatment options that are able to eliminate the infection and stabilise the condition of your gums. Periodontists are extremely skilled when it comes to conducting treatments of a number of oral conditions of the bone and gums. Some of these procedures include:
- Bone grafts – Surgery to fix issues associated with the bones in your mouth
- Functional and aesthetic gingivectomy – Surgical removal of the gum tissue
- Gingivoplasty – Surgical reshaping of the gums surrounding the teeth
- Crown lengthening
- Implants
Bear in mind, the milder cases of gingivitis can be cured through practising oral hygiene at home at undergoing a professional dental cleaning. The aforementioned surgeries are typically conducted when gingivitis has progressed to periodontitis or trench mouth.
