- Gum Disease (Gingivitis)
- What is the difference between gingivitis and periodontitis?
- What are the symptoms of gingivitis?
- What causes gingivitis?
- What are the risk factors and complications of gingivitis?
- How is gingivitis diagnosed and treated?
- Can gingivitis be prevented?
- How to practice good oral hygiene
- Some more information on gum disease
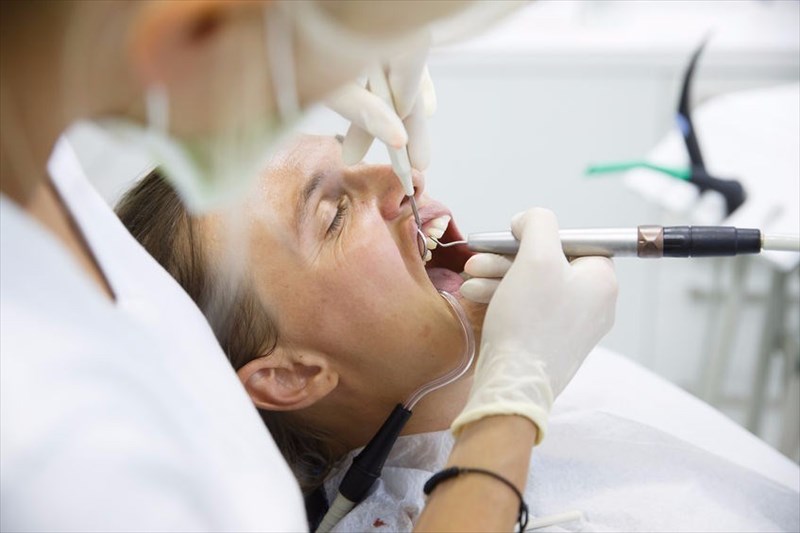
What is gum disease (gingivitis)?
Gum disease, also known as periodontal disease, is a dental infection that can lead to a number of other complications. The milder form of gum disease, which is scientifically referred to as gingivitis, refers to the teeth’s surrounding tissues (gums) becoming inflamed, which is typically due to poor practices of oral and dental hygiene. Simply put, gingivitis results in the inflammation of the gingiva specifically, this is the part of the gum that is found at the base of the teeth.
Gum disease is a common condition that may vary widely in its severity. The condition is characterised by swollen and red gums that will easily bleed when brushing your teeth or flossing. Gingivitis is commonly confused with periodontitis, however, the two terms refer to two different conditions, although someone who suffers from gingivitis may also suffer from periodontitis as gingivitis that is left untreated can progress to periodontitis.
Periodontitis, which is pronounced “per-e-o-don-TIE-tis”, is a severe gum infection that results in damage done to the soft tissue that leads to the destruction of the teeth’s supporting bone. This can cause loosening of your teeth, tooth decay and eventually tooth loss.
Both gingivitis and periodontitis are forms of gum disease. Gingivitis should be taken seriously and treated accordingly so as to prevent the condition from developing into periodontitis.
Through good dental and hygiene habits, you may be able to prevent the condition and even reverse it.
These include the following:
- Brushing your teeth at least twice daily (morning and night)
- Flossing regularly
- Going for regular check-ups with your dentist
For the sake of this information in the navigation menu above, we will focus on gingivitis specifically. To add more depth to your understanding of periodontal (gum) disease, we will also briefly describe periodontitis.
Other Articles of Interest

HIV/AIDS
Since the early 1980s, HIV/AIDS has been widely publicised as a destructive virus without a cure. We take a look at the best ways to treat the condition and live a quality life...
Diabetes (Diabetes Mellitus)
Diabetes (diabetes mellitus) is a long-term disease that requires daily management and care. The illness refer to a group of metabolic health conditions. Learn how the condition affects the body here.
Arthritis
Did you know? There are more than 100 different variations of arthritis and associated conditions. We take a look at the more common signs and types of arthritis here...

