
What is menopause?
Menopause is something a lot of women dread, however, it is a natural biological process and should not be seen as an adverse condition, but rather a period of transition. Menopause may mark the end of fertility, but this does not mean it will end your health and vitality, in fact, sticking to a healthy exercise regime during this time can actually keep you feeling fit and fabulous as well as help to improve the symptoms of menopause.
With fertility coming to an end, this means that menstruation will stop permanently and you will no longer be able to fall pregnant and have children. During menopause, the ovaries stop producing eggs and the body starts to produce less progesterone and oestrogen (the two main hormones needed to maintain a healthy pregnancy). Menopause is usually apparent when a woman is of a certain age (usually the forties or fifties) and has not had a menstrual period for 12 consecutive months.
If you have reached this stage, it is a turning point in your life and should not be seen as a disease or health issue, however, many women agree that menopause has a great impact on their overall feelings of well-being, both physically and mentally. This is often due to the adverse symptoms associated with menopause, some of which include, hot flushes, changes in mood, and various noticeable body changes (learn more about the full range of symptoms that may be experienced by clicking on the appropriate tab above).
These symptoms often trigger feelings of sadness, loss and depression in menopausal women. In others menopause may bring relief from worry over unexpected pregnancy or dealing with monthly periods. This time of life affects everyone differently and is symptoms are also experienced in vastly different intesity from one woman to the next.
There are a number of treatment options, both medical and lifestyle orientated, to help you through this period of change.
In the information found in the navigation menu above, we will discuss all that you need to know about menopause, from the symptoms through to treatment in order to make this journey an easier one for you and those around you.
Other Articles of Interest

Headaches
Headaches. We all get them. When is a headache something to worry about? What are the different types and how should a headache be treated? Here's all you need to know...

Stress
Stress can affect everyone differently. It is your body's biological response to a certain situation. It is important to know how to deal with stress in order to develop certain coping mechanisms...
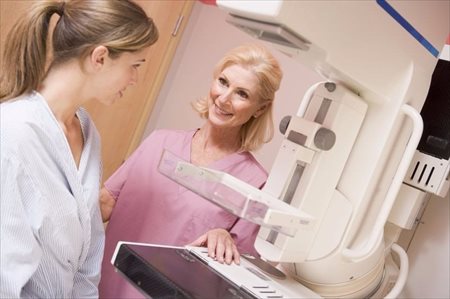
Mammogram (Mammography)
A mammogram is an X-ray used to screen the breast for breast cancer. It is a very important procedure to have done. Here's what you can expect to experience when having a screening done...
