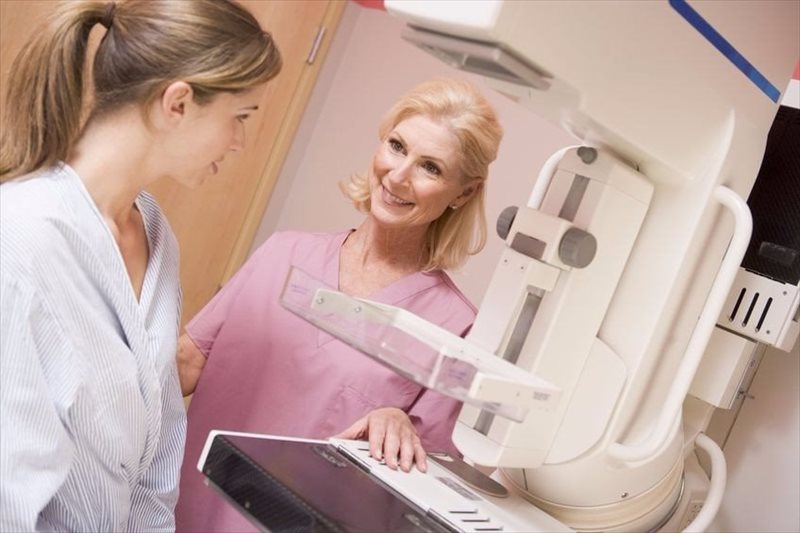
What is a mammogram?
A mammogram, also known as a mammography, is a screening method that screens the breast tissue for cancer (breast cancer) through the use of a specialised X-ray. These are a vital element in diagnosing breast cancer in the early stages, together with monthly self-examinations of the breast and regular clinical exams.
After skin cancer, breast cancer is the second most common cancer in women. Depending on age and family history, your risk for breast cancer may be higher.
Doctors recommend that women over 40 should undergo a mammogram every second year. If you have a personal history of breast cancer or it runs in your family, your doctor may suggest that you undergo more regular screenings. He or she may also suggest the use of further diagnostic tools.
Regular self-examination and medical screening is essential in the fight against breast cancer. This is due to the fact that if detected in the early stages, many forms of breast cancer can be treated and cured. It is important to note that mammograms do not cure cancer or reduce the risk of developing the condition, they are only a detection method.
Other Articles of Interest
Ultrasound scan
What is an ultrasound scan and how does it work? We look at the numerous ways this screening and monitoring tool is used in medicine today, as well as relevant benefits and considerations...
MRI (Magnetic Resonance Imaging)
What is an MRI? How does it work? What does it test? What can you expect to experience during the procedure? Here's everything you need to know...
CT (Computerised Tomography) Scan
What is a CT scan and what exactly does it involve? We break down this testing procedure so that you know what to expect when you go through your scan.