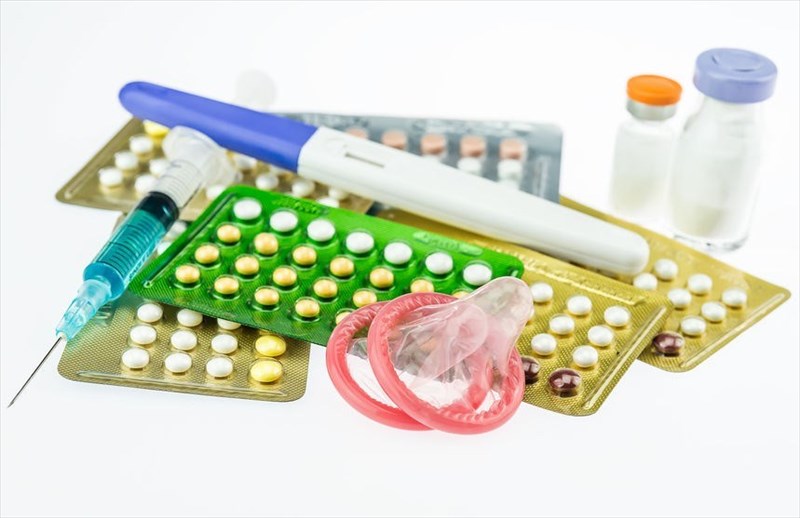
The type of birth control method you choose to use is a very personal one for both men and women. Some are more effective than others. The main reason behind a decision to use a contraceptive method is usually to prevent an unwanted pregnancy. The below types are sorted by how effective they are at preventing a pregnancy.
Extremely effective (99-100%):
- Abstinence: As the saying goes, “prevention is better than cure.” Pregnancy is 100% avoidable by practicing abstinence (not having sex at all) although this may not be realistic for the greater majority of people.
- Intrauterine device (IUD): A small t-shaped piece of plastic that is placed inside a women’s uterus by a medical professional. This prevents a man’s sperm from fertilising an egg. There are two types of IUD, hormonal IUDs and Copper IUDs. Hormonal IUDs are available in several different types, and release a small amount of hormones into the uterine cavity. This can thicken cervical mucus and prevent sperm penetration, or alter the uterine lining to make it inhospitable for a fertilised egg to implant. In some cases, the hormones released suppress ovulation (the release of eggs from the uterus). A copper IUD on the other hand, releases copper ions which damage sperm and disrupt their motility, thereby preventing them from travelling through the woman’s cervical mucus and fertilising the egg/s released during ovulation.
- Intrauterine Ball (IUB): IUB™ copper pearls are a relatively new birth control device which take on a three-dimensional spherical shape once inserted and is designed for single-use only. This new take on the IUD offers women a hormone-free, reversible pregnancy protection option (preventing pregnancy locally within the uterus), which is effective for up to 5 years.
The new device is inserted and removed in much the same manner as a normal IUD (intra-uterine device). IUBs are approximately half the size of the more traditionally used IUDs and are available in three different sizes of their own. Sizes available are 12mm, 15mm and 18mm (IUDs are available in sizes ranging from 32mm to 36mm). After measuring the size of a woman’s uterus, a doctor will recommend the most appropriate size.
The generally smaller sizes of these devices means that they can be inserted without the need for local anaesthesia and depending on the condition of a woman’s cervix, the procedure is generally a painless one. The contraceptive effect comes mostly from its copper components rather than from hormonal constituents. Copper pearls are strung onto a flexible wire frame which is coated with white polymer. At each end of the frame are two strings (made of uncoloured nylon monofilament thread), which extend into the vagina and are necessary for the removal of the device. Something that is unique about the device is that is consists of a shape memory alloy, Nitinol, which serves as a carrier of the copper material. This has been successfully used in medical implants and stents and is now proving to be effective in IUB devices too.
Once placed in a woman’s uterus (using a tube which is retrieved following insertion), the device coils back into its original smooth, round shape, becoming three-dimensional once more. This shape is better accommodated in the uterus. There are no sharp edges or corners. The new shape enables the device to remain in an ideal position within the uterus, with less risk of perforation, expulsion and malposition. Small amounts of copper are secreted, providing continuous birth control. The copper ions released function in much the same way as a copper IUD, by limiting sperm mobility and interfering with the fertilisation process (i.e. preventing sperm from being able to fertilise an egg / an egg from implanting in the uterus). Once inserted, the device position will be checked with an ultrasound scan examination. The device should begin taking effect immediately. Insertion of the device may require cervical dilation, especially if a woman has not experienced pregnancy before. Placement of the IUB is best done during the final few days of menstruation, when the cervix is typically wider and pregnancy risk is at its lowest. A follow-up may be required 4 to 12 weeks later, after which a doctor may recommend an annual check-up.
- Implants: A soft plastic rod is placed just under the skin of a woman’s arm by a medical professional. Synthetic progestin hormones are then released into the body via the rod gradually over a period of 3 years. This works by preventing ovulation in a woman.
- Sterilisation: A permanent method of birth control that involves cutting or blocking the tubes that carry eggs to a woman’s uterus (tubal ligation) or those which carry a man’s sperm (vasectomy).
Highly effective (approximately 91%)
- Injection: A progestin hormone is injected into the body and is slowly absorbed. The hormone prevents eggs from leaving the ovaries in a woman’s body, blocking ovulation. Generally, an injection lasts for a period of 12 weeks. If this method is chosen, it is important to receive subsequent shots on schedule if you wish to maintain this means of contraception.
- Patch: A small, sticky patch is worn on the surface of the skin. The patch sends steady levels of hormones into the bloodstream.
- Vaginal ring: A soft, plastic ring is placed inside the vagina. The ring releases a steady dose of sex hormones.
- Birth control pills (oral contraceptives): A set of pills taken daily at the same time. Pills contain levels of oestrogen and progesterone hormones which work by preventing the release of eggs from a woman’s ovaries.
Effective (approximately 80%)
Condoms: A thin, disposable wrap placed over the erect penis of a man just prior to sex. If used correctly, this prevents a man’s sperm from entering a woman’s vagina. Condoms are also highly effective for protecting from infections (sexually transmitted infections or STIs) such as HIV/AIDS.
- Cervical barriers: These can be diaphragms, caps or shields. Usually a small rubber cup that is filled with spermicidal jelly and place inside the vagina, over the cervix right before sexual intercourse. Sperm is then prevented from entering a woman’s uterus.
Moderately effective (approximately 70%)
- Spermicides: These are chemical developed to kill off sperm and usually come in jelly, cream or foam forms. Spermicides are commonly used together with a cervical barrier.
- Birth Control Sponge: A small foam pad that is soaked in a spermicide. The sponge is then placed inside the vagina and over the cervix.
- Fertility tracking: A woman can carefully track the changes in her body as a way to determine where in her cycle she is most fertile and when she is not. A sexually active woman is less likely to fall pregnant on days she is not at her most fertile (although this is not entirely impossible). Additional protection can include the use of a barrier method (the use of a condom) if following this type of birth control.
Emergency contraceptives
Contraceptive pills are available soon after a person has had unprotected sex (sexual intercourse without the use of a birth control method). These emergency contraceptive pills are often referred to as the ‘morning after pill’, and can be used as a backup if one has forgotten to use a birth control method or the type used has a higher chance of failing.
Emergency contraceptives can help to prevent an unwanted pregnancy for up to 5 days after unprotected sex, but will not be effective if a woman is already pregnant (i.e the fertilised embryo has been implanted in the wall of the uterus).
Contraceptive methods that are ineffective forms of birth control include douching, feminine hygiene products, homemade condoms or urinating after intercourse, although the latter can help to prevent urinary tract infections (UTI’s) in many cases, but more on that elsewhere.


 Condoms:
Condoms: