How does egg freezing work?
The process is a multi-layered one. Egg freezing involves ovulation induction, egg harvesting and freezing.
Egg freezing involves the first stage of IVF treatment. Just as with embryo freezing, fertility drugs / medications are necessary to induce ovulation to help produce numerous eggs for easier harvesting.
If a woman determined as healthy during the initial work-up, the process may begin at the start of their menstrual cycle. A woman may need to self-administer hormone injections and birth control pills (oral contraceptives) daily for 8 to 10 days. This is necessary to temporarily ‘turn off natural hormone production’. Another round of hormone injections is then administered for a period of about 2 weeks after that to stimulate egg production. This normally happens at the beginning of a woman’s menstrual cycle. A woman may also be given medications (gonadotropin-releasing hormone agonist or a gonadotropin-releasing hormone antagonist) during the last few days of stimulation to prevent premature ovulation.
The entire process is closely monitored by checking blood levels and frequent vaginal ultrasounds (two to three scans to monitor the growth of follicles). The ultrasound uses sound waves to produce a visual of the inside of your ovaries. A specialist will be watching for fluid-filled ovarian cysts where eggs mature (follicles). A woman’s oestrogen hormone levels generally increase when follicles develop. Progesterone hormone levels are typically low until ovulation.
When eggs have matured, the follicles are ready for retrieval (after at least 8 to 14 days) and a woman will be placed under light anaesthesia for the harvesting / retrieval process. This is an outpatient procedure (a woman is admitted to hospital for the day, and does not need to stay overnight). A common retrieval approach is transvaginal ultrasound aspiration. An ultrasound probe is inserted into a woman’s vagina to help identify a follicle. A suction device is then connected to the needle and guided into a follicle through the vagina. The same suction device and needle are then used to retrieve the egg, removing it from the follicle. In approximately 15 to 20 minutes, multiple eggs are removed.
After the harvesting / retrieval process a woman may experience some cramping and light pressure (similar to period pain) for a day or two as the enlarged ovaries return to their normal state.
Extracted eggs are then cooled to sub-zero temperatures by means of a flash-freezing process (known as vitrification wherein high concentrations of cryoprotectants are used in combination with rapid cooling) at minus 196 degrees Celsius or minus 384.8 degrees Fahrenheit, as this generally produces the most favourable results. This stops all biological activity and starts the preservation process. The specialist team of embryologists may use cryoprotectants to help prevent ice crystals from forming while frozen.
After the harvesting and freezing procedure, a woman can recommence normal activities after a few days. She will most likely be able to return to work after about a day or so, but may need to take things easy for up to a week. A specialist will advise a woman to avoid having unprotected sex to avoid an unwanted pregnancy as not all of a woman’s eggs may have been retrieved during the harvest procedure and can thus ovulate on the own after retrieval.
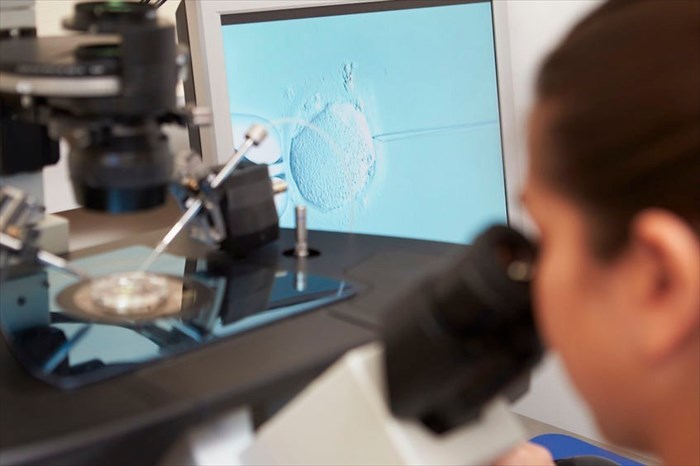
When a woman is ready, her specialist will thaw the eggs and inject each with a single sperm in preparation for fertilisation (intracytoplasmic sperm injection / ICSI). The fertilised eggs (embryos) are then given time to grow in the lab for a period of about 5 days. From there they are ready to be transferred and implanted in a woman’s uterus. The implantation process is similar to a pap smear and is relatively quick and painless.