Treatment for conjunctivitis most often begins with things a person can do for themselves in order to alleviate the symptoms causing discomfort. For instance, contact lens wearers must discontinue use until all conjunctivitis symptoms have cleared up (or a treating medical professional gives the all-clear to resume wear). A doctor may advise that contact lenses and their casing be disposed of, and a new set made (normally if lenses are the disposable variety). If hard lenses are normally worn, a doctor may provide recommended care instructions for disinfecting them before they can be used again.
In the meantime, wearing of eyeglasses where necessary is advisable. A doctor may recommend high-index lenses with an anti-reflective coating (making glasses lighter and thinner), which will help to reduce distracting reflections. Alternatively, photochromic lenses can help to reduce problems with light sensitivity and also protect eyes from high-energy blue light. These options may also be considered in place of having new contact lenses made.
A doctor may recommend that any eye make-up a person has used before developing conjunctivitis be thrown away due to risk of contamination. If used again, risk for re-infection is likely.
To determine the most effective means of treatment, an underlying cause of symptoms is necessary. What works for an allergic bout of conjunctivitis may not be at all effective for those affected by a bacterial cause, and vice versa.
Medical treament for conjunctivitis
Medical treatment is typically recommended to:
- Increase comfort by alleviating symptoms associated with pink eye
- Reduce inflammation and the course of infection
- Prevent transmission of infection (if a contagious form is identified)
Treatment of conjunctivitis based on its cause
Treatment according to the underlying cause or primary type of conjunctivitis involves:
Viral conjunctivitis
The majority of viral infections are generally mild and thus typically resolve without treatment or long-term health complications within 2 to 4 weeks. The body will, most often, naturally work out the virus causing infection during this period, thus easing pink eye symptoms. If a doctor has made a diagnosis, antiviral medication may be prescribed (often for topical use) to help things along and ease more severe symptoms (i.e. those caused by more serious viral infections like the herpes simplex virus).
Bacterial conjunctivitis
An underlying bacterial cause will be treated with prescribed antibiotics (eye drops or ointment to be used topically). Antibiotics help to alleviate symptoms, reduce the risk of further complications (by shortening the duration of infection), as well as the possibility of transmitting the infection to others.
Antibiotic medications will be selected with the severity of the infection in mind, as well as the overall state of a person’s immune system (and whether there is a risk of antibiotic resistance to a specific medication in relation to the type of bacterium causing the infection) and the type of bacteria determined as the cause.
With antibiotic treatment, a mild case of bacterial conjunctivitis will show improvement within 2 to 5 days (without further complications) but can sometimes take as long as 2 weeks to clear completely. 16 A patient must use antibiotics prescribed exactly as recommended by the treating doctor, for as long as is directed.
Chlamydial conjunctivitis will involve treatment with chlortetracycline ointment and tetracycline tablets which in combination, will resolve the full spectrum of infection symptoms. Antibiotic eye drops may also be recommended.
Allergic conjunctivitis
Once an allergen is identified (either before a consultation or when determined through testing), a doctor will recommend a separation of the adverse substance from the person concerned (where possible). Once an allergen is no longer in a person’s environment, symptoms are likely to show a marked improvement.
To ease discomfort, a doctor may recommend topical antihistamine eyedrops or vasoconstrictors (prescription eye drops), sometimes in combination. Those containing antihistamines will help to alleviate irritation and itchiness in the affected eye/s.
Vasoconstrictors typically work to compress blood vessels in the eye, and thus relieve redness. Allergy medications (prescribed according to the different types of allergies experienced) may also be recommended to alleviate allergic reaction symptoms, like redness and itching. Antihistamines, mast cell stabilisers (a class of non-steroid controller medication which blocks the calcium channel and prevents the secretion of histamine), decongestants, steroids and anti-inflammatories are common medications normally recommended for most kinds of allergies and can also be helpful in alleviating the symptoms of allergic conjunctivitis.
To treat giant papillary conjunctivitis, a doctor will normally remove the object (often contact lenses) causing an abnormal immune response and flush the eye with a saline solution. Severe symptoms may then be treated with a short course of prescribed eye drops containing corticosteroids (to effectively reduce swelling and the body’s immune response).
Chemical conjunctivitis
Exposure or contact with foreign substances, like chemicals, vapour, fumes or dust will not normally require much medical intervention. Normally at the first sign of contact, flushing the eye with fresh running water for several minutes is advised. Thereafter homecare treatment may be recommended to alleviate symptoms while the eye/s heal. Acid or alkaline substances which make contact with the eyes, such as bleach, must be attended to by a medical doctor immediately so as to avoid injuries like sight impairment or scarring. In such instances, the affected eye/s will be flushed with a saline solution. Thereafter topical steroid ointments may be recommended to alleviate symptoms further.
In the case of medication-induced conjunctivitis, a doctor will have determined the offending agent (medication or preservative) during the diagnostic process. Treatment will involve discontinuation of the medication or product in order to ease symptoms, as well as the use of immunosuppressive agents (like corticosteroids). Ideally, as many medications as can be discontinued should be while symptoms subside. Should the offending medication be needed for treatment of another condition (like glaucoma), a preservative-free or less toxic option may be recommended in its place. Supportive measures, such as the use of preservative-free lubricants (drops or ointments) or anti-glaucoma medications, and cool compresses can help to alleviate inflammatory discomforts and dry eye symptoms. If itching is a problem (often due to dry eye symptoms), antihistamines or mild topical steroid ointments can be used.
In most instances, chemical / toxic conjunctivitis resolves on its own within a few days, with much improvement in several hours of flushing out irritants with clean running water. If no improvement occurs after 24 to 36 hours, it is advisable to consult the doctor once again for an evaluation.
How is conjunctivitis in babies treated?
A newborn baby with signs of neonatal conjunctivitis will need to be evaluated immediately (at the first indication of possible pink eye) and diagnosed and treated swiftly. Underlying causes of conjunctivitis in a newborn can rapidly develop serious complications that, if not treated timeously or adequately, can result in life-long problems and health complications.
In many instances, neonatal conjunctivitis may be prepared for if a pregnant woman has a diagnosed condition like genital herpes (HSV-2), chlamydia or gonorrhoea. A baby born to a woman with such conditions can easily contract an infection during the childbirth process. If this is a known factor, doctors and their medical teams can not only help to minimise the risk of transmission, but also prepare for possible health concerns should transmission occur.
Neonatal conjunctivitis can occur during childbirth (when the infant is exposed to various types of bacteria during the birth process, not just an STI) or within the first few weeks of life at home (due to exposure to bacteria outside the hospital environment). Not all instances of neonatal conjunctivitis are, thus, as a result of the transmission of an STI from mother to child.
Infection as a result of bacterial causes will need to be treated with antibiotics, these can be applied topically (using eye drops or ointments) or given orally (by mouth). Antibiotics can also be administered intravenously (through an IV line in the arms). An infant with neonatal conjunctivitis may be treated with a combination of antibiotics in any form (oral, IV or topical).
Chlamydial conjunctivitis (also called inclusion conjunctivitis) will normally be treated with oral antibiotics. Intravenous (IV) antibiotics are usually administered for the treatment of gonococcal conjunctivitis (i.e. conjunctivitis as a result of a gonorrhoeal infection). This helps the body to absorb medication quickly, so as to avoid the development of corneal ulcerations or glaucoma (a group of eye conditions that have the ability to cause blindness).
Doctors and their medical teams will also use a saline solution to rinse the affected eye/s of a newborn baby to remove any build-up of mucous or pus discharge. A warm compress applied to the eye will also help to alleviate swelling.
If through evaluation, it is determined that a baby has a blocked tear duct (also known as a nasolacrimal duct obstruction) that is causing the symptoms of conjunctivitis, the area between the eye and the nose may be given a warm, gentle massage to help ease discomfort. A baby with this condition will be closely monitored during his or her first year of life, and if the blocked tear duct does not resolve after 12 months, surgical repair may be considered.
A baby may also develop conjunctivitis through chemical contact. If chemical irritation is determined, a doctor will likely monitor a little one without much medical treatment. A newborn should show signs of improvement within 24 to 36 hours, with appropriate homecare. 17
Home treatment for pink eye
Homecare is also an important part of treatment, helping to alleviate symptoms of conjunctivitis. A doctor may make the following recommendations:
- Cleaning the affected eye/s with a clean, damp, lint-free cloth or cotton wool (using individual cloths / cotton wool for each affected eye).
- Applying (on closed eyes) warm and cold compresses to the affected eye/s (several times a day) for the relief of pain (cold compress) and swelling and irritation (warm compress). Tip: If both eyes are affected, it is best to use a different compress for each, ensuring that one does not touch the other and thereby reducing risk of spreading an infection.
- Using the recommended eyedrops (also referred to as artificial tears) for the relief of symptoms (as many times a day as directed by a treating doctor).
- Practicing good hygiene daily, taking care to wash hands (in particular) before and after applying treatment to the affected eye/s, as well as when handling food.
- Avoiding wearing make-up until symptoms resolve.
- For those prone to allergic conjunctivitis, taking measures to minimise exposure to allergens is recommended – ensure that the home is kept dust-free, windows are closed, and air-conditioning used when pollen counts are high, an indoor air purifier is used, and that harsh chemical products (dyes or perfumes etc) are not used. Some may find relief by proactively using certain medications (with the guidance and consent of a medical professional) to reduce the likelihood of allergic reactions during peak times of the year. Antihistamine medications can cause a little drowsiness, so appropriate precautions must be taken when using these medications (such as not driving when experiencing this side-effect).
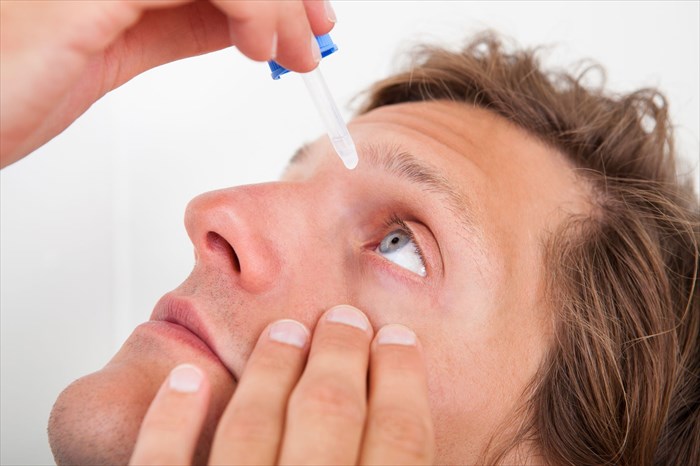
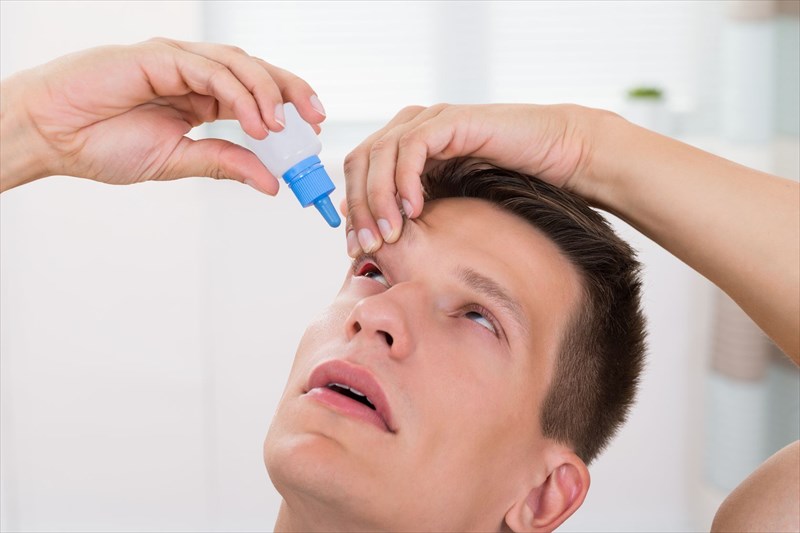
Tips for inserting eye drops
- Wash hands thoroughly with warm water and soap. Hands should be dried with a clean towel.
- Lay down and look up at the ceiling (with both eyes). Tilt the head backwards and gently pull the lower lid down with one hand. Some are more comfortable doing this when facing a mirror.
- Hold the bottle of eye drops with the other hand over the eye (facing downwards). If more comfortable, rest the hand holding the bottle on the forehead to help keep it steady.
- Squeeze out one drop on the inside of the lower lid, without allowing the tip to touch the eye.
- Blink the eye and dab away excess fluid with a clean tissue or cotton wool ball. Keeping the eyes closed for a minute or two can also help for better absorption of the medication.
- Wash hands thoroughly once again.
If both eyedrops and ointments have been recommended by a doctor, it is best to apply the drops first, and then the ointment (which can be done in a similar way). In this way, treatment will be more effective, allowing for the drops to be better absorbed. Sometimes, ointment application is easier for a young child or infant to tolerate than eye drops. A doctor can assist with the easiest means of application should a parent experience difficulty.
If using more than one type of recommended eye drops, application should ideally occur several minutes apart. Apply one medication, wait up to 5 minutes and then apply the next one.
A person’s vision may be temporarily blurry shortly after applying eye drops. It is best to wait until vision is completely clear before performing any tasks requiring clarity of vision, such as cooking and preparing food (i.e. using host surfaces such as stoves or knives), driving or operating machinery.
Persistent blurry vision and pain that develops after applying eyedrops must be thoroughly evaluated by a treating medical doctor as soon as possible. If other visual problems such as loss of sight or photophobia (light sensitivity), and the development of intense redness is in the eye develops after using eyedrops, a doctor should also be consulted as soon as possible. It could be that infection has spread beyond the conjunctiva and the affected individual will need an adjustment in their treatment plan in order to resolve the condition. A thorough check is necessary to determine this.
References:
16. Centers for Disease Control and Prevention. 2 October 2017. Conjunctivitis (Pink Eye) Treatment: https://www.cdc.gov/conjunctivitis/about/treatment.html [Accessed 22.08.2018]
17. National Eye Institute. November 2015. Facts about Pink Eye: https://nei.nih.gov/health/pinkeye/pink_facts [Accessed 22.08.2018]