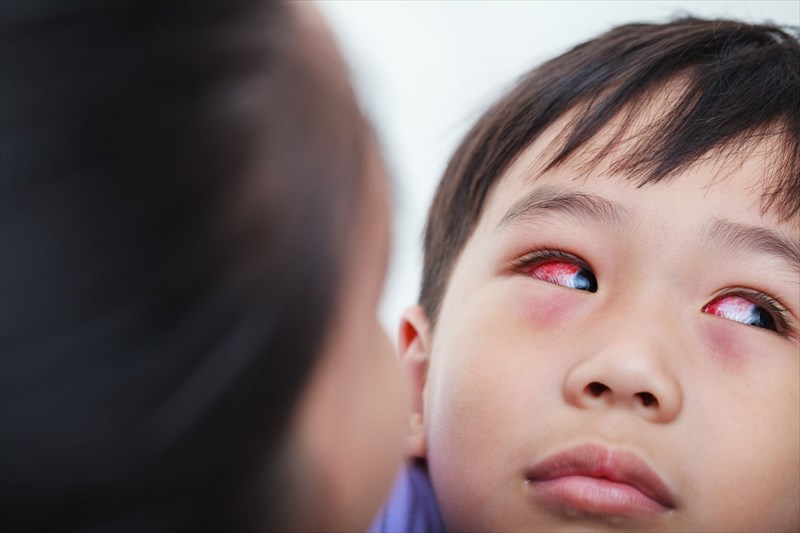
If signs and symptoms are bothersome and conjunctivitis is suspected, a consultation with the doctor (primary healthcare physician / general practitioner) is advisable, especially if there is a possibility that the underlying cause may be viral or bacterial.
If one wears contact lenses, it is best to stop wearing them and note any symptom changes (whether a consultation has been booked or not). Sometimes conjunctivitis symptoms may resolve within 12 to 24-hours once the aggravating source is removed (in this instance, the contact lenses). If not, the cause may be an infection and should be thoroughly assessed by a medical doctor.
Ahead of a medical consultation, it is a good idea to ensure that sound hygiene practices are maintained (particularly handwashing with warm water and soap), and that no towels and other hygiene care products or linens are shared with others (thus increasing potential risk of spreading an infectious form of pink eye / conjunctivitis).
What to expect during a consultation
Once at the doctor’s office, he or she will conduct a full medical review and discuss the nature of symptoms being experienced. During this process, a doctor will ask a series of questions and note down relevant details which can help to contribute to a diagnosis, including any notable environmental factors which can contribute to eye irritation.
The types of questions which a doctor may ask include:
- How long ago did symptoms begin?
- Have these symptoms been experienced on a continuous basis since they began? Or have they appeared to come and go?
- Is just one eye currently affected? Or both?
- Would you describe symptoms as mild or severe (i.e. are you experiencing aggravating discomfort or pain)?
- Are you experiencing symptoms other than those affecting your eye/s? If so, what? Are they mild or severe? Did they start around the same time as eye-related symptoms?
- Do you have any known allergies? If so, what?
- Do you wear contact lenses? If so, how often? When last were they worn? How often do you clean your contact lenses? How often do you replace your contact lens storage case?
- Have you tried anything that has seemingly improved symptoms (e.g. discontinuing the wearing of contact lenses)?
- Have you noted anything specific that has appeared to worsen conjunctivitis symptoms?
- Have you been around anyone else who has pink eye or similar symptoms?
- Have you been around anyone recently who has shown cold and flu symptoms, or other respiratory conditions?
- Have you recently been exposed to any chemical products which have been in contact with your eyes?
Following a symptom discussion and medical review (including a brief family history), a doctor will request that you undergo a physical examination. More often than not, a diagnosis can be made at this stage. Differentiating indicators may already point to a possible viral, bacterial or allergic underlying cause. Other than symptoms affecting the eye/s, any others experienced around the same time will also strongly hint at a possible cause.
Tell-tale signs a doctor will look for during a physical examination in order to diagnose an underlying cause are as follows:
- Viral: Pink eye symptoms are accompanied by other indications of a viral infection, like that of a cold or respiratory tract infection. Discharge from the affected eye/s is of a watery consistency (not thick, mucous-like or pus). Testing for diagnostic purposes is not normally necessary for viral conjunctivitis (pink eye) unless the condition is severe, chronic or recurrent and the specific virus causing pink eye needs to be identified. 14
- Bacterial: Eye-related symptoms often occur alongside sinus or ear infections. Discharge that indicates a bacterial infection will be thick (not watery or clear) mucous or pus.
- Allergic: A doctor will take into account possible seasonal influences (i.e. does the consultation coincide with a time of year that has a high pollen count – spring or summer?). Itching may be described as intense or severe and a doctor will be looking for both redness in the white of the eye, as well as small bumps on the inner eyelids. Symptoms associated with allergic conjunctivitis will often also be accompanied by other signs of allergen related illnesses, like asthma, hay fever or eczema.
An examination may also involve an evaluation of external eye tissue and the conjunctiva (using magnification and bright light tools), as well as visual acuity measurements (to check for any possible visual impairments). An evaluation of the inner structures of the eye may be recommended as well (this type of testing involves a slit lamp eye examination). This is to assess whether any other tissues of the eye may have been affected by conjunctivitis.
Tear or fluid samples (conjunctival scrapings) from the affected conjunctiva may only be necessary for laboratory analysis should the symptoms present be severe, or if a high-risk cause is suspected (such as a bacterial or specific sexually transmitted infection).
In this instance, a topical anaesthetic may be applied and a sample of teary fluid (or discharge) swabbed with the use of a platinum spatula or other metallic object and sent for a culture analysis to determine signs of a bacterium or other infectious substance which may be causing conjunctivitis.
If an underlying cause is tricky to diagnose using a medical review and physical examination alone, a doctor may send a sample for analysis, even if symptoms are not severe, in order to rule out or help diagnose the cause of infection.
Alternative diagnosis
Other conditions which may present similar sets of symptoms as those exprienced with conjunctivitis include acute:
- Glaucoma (a rare form of glaucoma which can lead to incurable loss of vision)
- Keratitis (inflammation of the cornea which can also result in permanent vision impairment / loss)
- Blepharitis (inflammation of the eyelids, which can also display dandruff-like scales / crusting on the eyelashes)
- Iritis (inflammation of the iris that can cause the iris to stick to the lens and prevent fluid drainage from the pupil, thus resulting in permanent damage to the eye)
While rare, conjunctivitis may also be one of many signs and symptoms of other illnesses not specifically relating to the eyes. These can include conditions like:
- Lupus (systemic lupus erythematosus)
- Inflammatory bowel disease (such as ulcerative colitis or Crohn’s disease)
- Rheumatoid arthritis
- Kawasaki disease
Together with relevant symptoms and appropriate testing, these conditions can either be ruled out or diagnosed, and conjunctivitis can then be treated symptomatically. A diagnosis must be accurately made, however, so that a doctor can recommend the most appropriate means of treatment.
Should a patient be diagnosed with chronic conjunctivitis or return to the doctor’s office if symptoms are not improving after the recommended period of time, cultures or smears of fluid substances may be taken and sent for further supplemental laboratory testing, in order to determine an underlying cause.
A severe set of symptoms may prompt a doctor to refer a patient to an ophthalmologist (a specialist in medical and surgical eye conditions or diseases) for further, more comprehensive evaluation.
Allergic Conjunctivitis
Allergic conjunctivitis may be tested using any of the following:
Allergy skin test
If an allergy is unknown, a skin prick test may be recommended in order to determine what may be causing symptoms of conjunctivitis. A skin prick test (also known as a puncture or scratch test) helps a doctor to be able to determine a specific allergen by examining the body’s reaction. As many as 40 different substances can be tested at once. Allergens such as mould, pollen, animal / pet dander, foods, or dust and dust mites are most often tested for in this way.
In adults, the test is usually performed on a person’s arm in a doctor’s office. A doctor may choose to perform the test on the upper back of children. A doctor will draw marks on the skin after cleaning the site to be used thoroughly. Drops of specific allergens will then be placed the drawn markings. A lancet will then be used to prick into the skin’s surface. This will not normally be a painful experience (as the tool does not penetrate the skin deeply) and doesn’t cause any bleeding either. A temporary and mild discomfort is normally all that is to be expected. A new lancet is used to prick each allergen being tested.
Histamine, glycerine or saline may also be scratched into the surface of the skin to assess whether skin is reacting in a manner that is to be expected. Histamine will cause a skin response that indicates an allergy. Glycerine or saline are more likely to cause a reaction if a person has sensitive skin, but not necessarily an actual allergy.
Within about 15 minutes, allergic reactions (if any) may be observed 15 – a person may develop red and itching skin bumps (or wheals) at the marking site where an allergy may be identified. Once determined, a person’s skin will be thoroughly cleaned. Once the allergy is identified, it can be treated, and steps can be taken to reduce exposure to the offending allergen.
Blood test
A sample of blood may be taken for laboratory testing. Technicians will analyse a sample for the presence of proteins or antibodies which will indicate an immune response to possible allergens (i.e. increased production will indicate that the body is actively trying to protect itself from a substance it deems harmful).
A complete blood count may also be assessed, including the presence of eosinophils, a type of white blood cell produced in bone marrow, which become more active when an allergen is detected in the system.
References:
14. National Center for Biotechnology Information. December 2017. Conjunctivitis, Viral: https://www.ncbi.nlm.nih.gov/books/NBK470271/ [Accessed 22.08.2018]
15. US National Library of Medicine - National Institutes of Health. February 2013. The skin prick test – European standards: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3565910/ [Accessed 22.08.2018]
