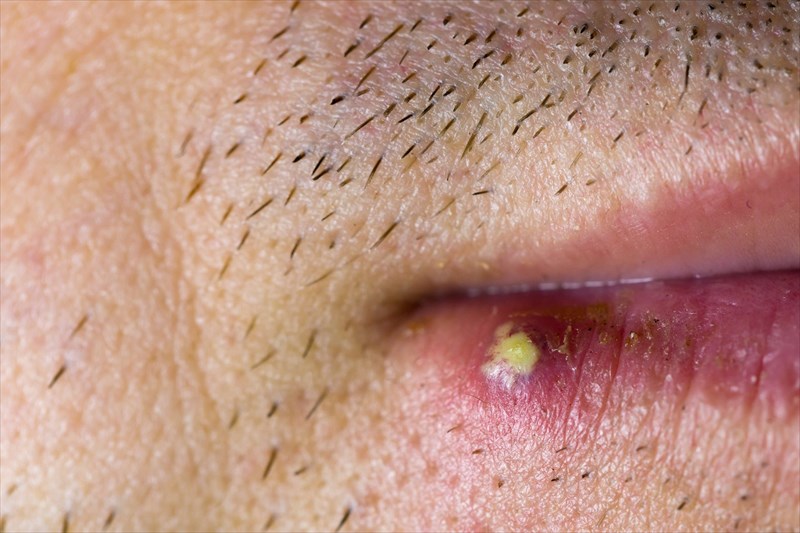
Who is most at risk of getting herpes?
The honest truth is, we are all at risk, young and old. Any one of us can be exposed to the HSV virus. It is estimated that up to 90% of adults, worldwide, have been exposed to and carry the HSV virus, even if symptoms have not been experienced.
Risk increases for those who have compromised immune systems or certain existing conditions. The reason for this is that risk of further medical conditions increases with an active infection.
Risk factors include:
- Chemotherapy (for the treatment of cancer)
- HIV/AIDS
- Eczema
- Severe burns
- Anti-rejection medications (for those who have undergone organ transplants)
What are the common complications or side-effects of the herpes simplex virus?
Those with weakened immune systems are generally at most risk for the various types of complications, affecting the following areas of the body:
- The eyes: Eye infections (known as kerato-conjunctivitis) can occur as a result of herpes simplex virus infection. If these types of infections are experienced frequently, they can cause visual problems, such as blindness and scarring if the infection affects the cornea. Sores and blisters on the eyelids can also cause considerable swelling and discomfort.
- The fingertips: Herpes whitlow (or herpetic whitlow) is an infection of the fingertips which often occurs in children who suck their thumbs. An infection can easily then be spread from the mouth to the thumbs. Cold sores can spread to any area of the hands, resulting in an outbreak of blisters and sores on the fingers, especially if there is a cut or graze on the skin at the time.
- The skin (widespread): If you are prone to skin condition such as eczema, the development of blisters and cold sores can easily be spread to other portions of the body. In severe instances this can become a medical emergency.
- Organs: The most notable concerns are when an infection spreads to the spinal cord or brain, resulting in conditions such as encephalitis, and causes swelling in these areas of the bodies. Swelling increases the risk of brain damage and can be extremely life-threatening.
- Dehydration: If pain in the mouth and throat is so severe, you may be reluctant to drink fluids during an outbreak. Care should be taken not to dehydrate. Rather see your doctor for diagnosis and treatment recommendations to help alleviate symptoms.
Can herpes be prevented?
If it can’t be cured, is it possible to prevent herpes outbreaks? When it comes to prevention, outbreaks may not be entirely avoidable, but there are measures you can take to reduce recurrences and spreading of the virus.
These include:
- Practicing good hygiene habits, especially when an infection is active. Wash your hands frequently with soap and water.
- Avoid sharing objects that increase transmission risks such as lip balms or lipsticks, towels, clothing, razors, toothbrushes, cutlery and crockery.
- Avoid skin contact where possible, such as kissing or any form of sexual contact, especially when an infection is active and blisters or sores are present.
- Avoid touching other areas of the body when an infection is active, especially the genitals and eyes.
- Take care to avoid possible outbreak triggers such as other infections, like the common cold or flu, and stress.
- Use lip balms and sunscreen frequently to reduce the risk of outbreak flares.
- Supplementing with L-lysine. In laboratory settings this amino acid interferes with arginine, another amino acid that promotes the growth of HSV. Efficacy in humans still needs further trials to provide conclusive evidence.
An infection essentially remains in the body for life, even if no symptoms ever manifest. Outbreaks vary from person to person. Some experience many outbreaks, and others hardly ever during their lifetime. Medical professionals tend to agree that recurrent infections are typically less intense than an initial experience (primary) or once a growing child develop antibodies. A generally healthy person does not develop further health complications with this virus.
How can you tell the difference between herpes and psoriasis?
What is psoriasis?
Also a condition that manifests symptoms in the skin, psoriasis is an inherited autoimmune disease that can range from mild to severe. The condition typically causes cell production in the skin to significantly speed up and accumulate on the surface. This causes skin thickening and as a result, considerable irritation and discomfort.
The most common areas this condition affects include the face, elbows, knees, back, scalp, palms of the hands and soles of the feet. Psoriasis can also affect the genital area.
The main symptoms of this condition include:
- Dry and cracked skin (surface)
- Patches of red skin (sometimes accompanied by silver scales)
- Inflammation – itching or burning sensations on the affected areas of skin
- Swollen or stiff joints
- Pitted (thick) nails
Unlike herpes, psoriasis is not a contagious skin condition and cannot be transmitted from one person to another through contact.
How to tell the difference
- Psoriasis: Affected skin areas appear smooth and flat, sometimes with scales. Irritation is also experienced in areas of the body such as the elbows and knees.
- Herpes: Affected areas manifest symptoms of blisters and sores, sometimes ulcers, accompanied by other symptoms such as fever and fatigue.
Any skin irritation that develops, especially when it doesn’t resolve on its own in a short period of time should be thoroughly checked by a medical professional for proper diagnosis and treatment. If you are unsure, see your doctor (general practitioner / GP or dermatologist).
What is birth-acquired herpes?
Birth-acquired herpes (or congenital herpes) is an infection that affects an unborn baby during pregnancy. The infection can also occur during the birthing process, especially if a mother is infected with the HSV-2 virus (genital herpes).
When an infant is born with an infection, they typically display what is known as systemic herpes (a system-wide infection of the skin). This is regarded as severe and can cause a variety of very serious health concerns for a new-born. Complications which can easily arise as a result include problems with breathing, damage to the brain (such as inflammation) and seizures. The entire body can become infected with herpes.
Organs such as the lungs, liver and kidneys are also at risk of serious complications. This is known as disseminated herpes.
Birth-acquired herpes is effectively passed from mother to child, more often during a vaginal birth. A virus can be dormant in a mother and become active at any time. If active at the time of birth and a baby comes into contact with genital herpes blisters during delivery, a baby will become infected. The chances of passing on an infection during delivery when the virus is dormant is slim, but not impossible either.
A mother can also pass on HSV-1 through direct contact between a baby and an active outbreak of blisters or sores. A new mother with an active outbreak should take care not to kiss or place the baby at risk of direct contact while sores and blisters occur.
Herpes in babies with birth-acquired herpes may show up as clusters of fluid-filled blisters, mainly on the torso and around the eyes. A baby may also have symptoms of extreme fatigue and feeding problems.
Doctors may perform various tests to check the nature of infection and whether various areas of the body, such as the brain and organs are at high-risk of further health complications. Tests can include blood and urine samples and even an MRI scan.
Treatment will involve managing symptoms with IV (intravenous) administered antiviral medications and general hygiene and inflammation care. If other complications are present, associated symptoms and concerns will be appropriately treated as well.


