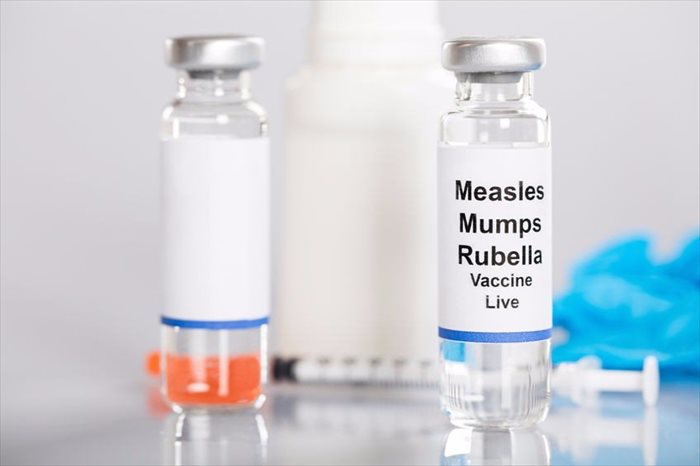
Mumps is prevented through the MMR vaccine. People are considered immune if they have previously been infected as they cannot become infected for a second time or if they have had the vaccine and are therefore immunised against mumps.
The MMR vaccine, also known as the Measles, Mumps and Rubella vaccine, is recommended for children before they start school. The following is a list of criteria for the administration of the vaccine:
- Being between the ages of 12 and 15 months old – this is when the first dose of the vaccine is given.
- Being between the ages of four and six years old, or between the ages of 11 and 12 – this is when the second dose of the vaccine is given.
- You are an adult and have not had the vaccine or your antibody titer test shows that your levels of immunity to measles, mumps or Rubella is low. An antibody titer test detects the presence and quantity of antibodies in the blood.
People who do not need or should not get the MMR vaccine
The vaccine does not need to be administered:
- If you have had two doses of the vaccine after the age of 12 months old or if they have had one dose of the MMR vaccine and a second dose administered of the measles vaccine.
- If you have had one dose of the MMR vaccine and is not at high risk of exposure to measles or mumps.
- If you have had blood tests that illustrate their immunity to mumps, measles as well as rubella.
- If you're a man who was born before the year 1957 (those born before this year are thought likely to have already been exposed to measles or mumps in childhood, however, this is not a hard and fast rule).
- If you're a woman that was born before the year 1957 and don't plan to conceive any more children – this recommendation is due to the fact that an inactive form of the measles virus was used in a vaccine that was administered between 1963 and 1967 and may no longer be effective.
- If you are pregnant or plan on falling pregnant in the next couple of weeks.
- If you have a life-threatening reaction to the antibiotics neomycin or gelatine.
- If you have an immune system that is severely compromised or are taking oral steroids. However, in some cases, immunisation against the virus can outweigh the risks and your doctor will be able to advise you on the best course of action.
Those who should get the MMR vaccine
If you do not fall into the criteria above, you can get vaccinated if you:
- Are not pregnant or do not plan on falling pregnant
- Attend trade school, college or postsecondary school institutions, as one has a higher risk of infection in highly populated environments.
- Work in a medical facility, school, child-care centre or hospital
- Plan on travelling overseas or going on a cruise
Those who should wait to get the MMR vaccine
You should consider delaying the vaccine if:
- You are severely or moderately ill - It is advised that one wait until fully recovered.
- You are planning to fall pregnant - It is generally advised by manufacturers of the MMR vaccine that pregnancy be postponed for 3 months after receiving it, while the Advisory Committee on Immunisation Practices (ACIP) recommends waiting for 4 weeks after vaccination before trying to fall pregnant). The MMR vaccine has been linked to birth-defects and can impact the health of the foetus.
- You are pregnant - It is important to wait until giving birth and possibly until breastfeeding is finished so as not to compromise the pregnancy or the health of the newborn infant.
Those who should check with their doctors before getting an MMR Vaccine
You should check with your doctor before being vaccinated with the MMR vaccine for mumps if you:
- Currently have cancer
- Have a blood condition or disorder
- Have a disease that impacts the immune system, such as HIV and AIDS.
- Are being treated with drugs that impact the immune system such as steroids.
- Have received another vaccine for a different condition in the last four weeks.
Side effects of the MMR vaccine
One cannot contract mumps from the MMR vaccine and the majority of people who are given the vaccine, do not experience any side effects. Some people may experience a mild rash or a fever and some adults may also suffer from achy joints after the administration of the vaccine.
Concerns have been raised in the past regarding the link between the MMR vaccine and autism. Some people believed that the vaccine could lead to the development of autism in children. However, extensive research has been conducted to prove this theory wrong and this research concluded that there is no scientifically proven evidence to back the theory of the link between autism and the MMR vaccine.
Can you get mumps if you have been vaccinated?
You can get mumps even if you have received the MMR vaccine in some rare instances. This is because the vaccine preventsmost but not all cases of mumps. Those who have received it are approximately nine times less likely to contract this virus. Those who have been vaccinted with the standard two doses of the MMR vaccine may, after prolonged exposure to someone with the virus, also contract it, but the illness is usually far less severe than those who don't get vaccinated1.
References
1. Centers for disease control and prevention. November 2017. Mumps - Outbreak-Related Questions and Answers for Patients. Available: https://www.cdc.gov/mumps/outbreaks/outbreak-patient-qa.html [Accessed 19 November 2017]