What are the causes, risk factors and complications of a peptic ulcer?
How does food get digested?
When we eat food, our stomach produces a chemical known as hydrochloric acid, as well as this, an enzyme termed pepsin is also secreted, this acid and enzyme combination aid in the digestion of food.
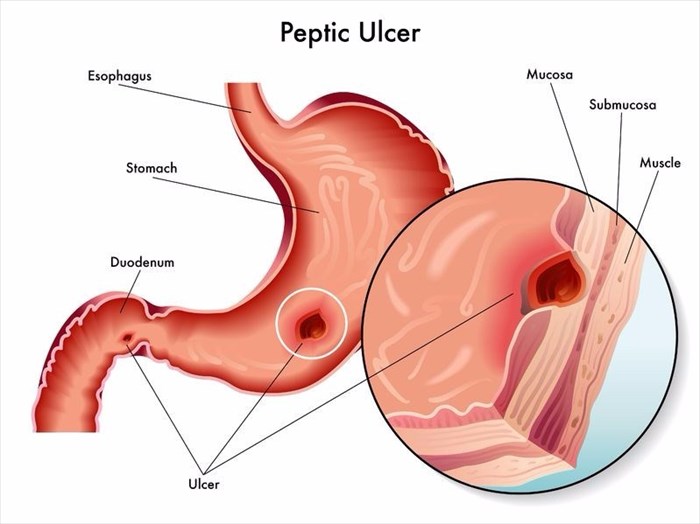
Food is then partially digested when it is in the stomach, and from here it moves to the upper part of the small intestine (duodenum) where the process of digestion continues.
A peptic ulcer may occur if the acid (hydrochloric acid) and enzyme (pepsin) create an imbalance in the lining of the digestive tract (either in the stomach or duodenum) and overcome the defence mechanisms in place in the digestive tract which usually aid in protecting the lining from these harsh substances. This may result in the mucous membrane (mucosal wall) eroding, and in doing so, an ulcer will form.
It was previously thought that the peptic ulcers were a result of specific eating habits that involved highly acidic foods and other lifestyle factors such as smoking cigarettes and stress. It is now evident that those who suffer from peptic ulcers may have an imbalance in the blend of pepsin and acid present in the digestive tract, combined with the failure of the digestive tract to protect its mucosal wall from these extremely harsh substances.
What causes a peptic ulcer?
- An imbalance of the digestive substances pepsin and acid,
- coupled with the digestive tract’s self-defence failure allowing for the mucosal wall to be penetrated by the harsh substances.
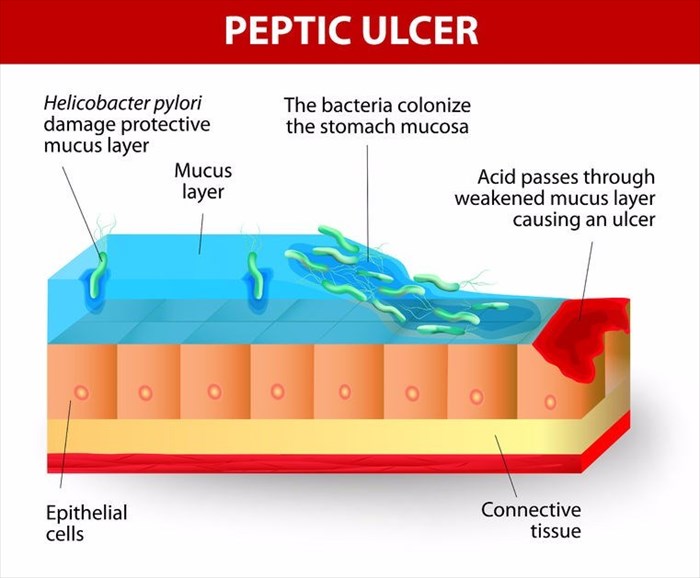
Research conducted during the 1980s contained evidence showing that ulcers are often a result of the bacterial infections of the bacterium H. pylori (Helicobacter pylori). However, not all cases of ulcers are caused by the bacterium and can also be from the prolonged use of certain pain medications such as aspirin or nonsteroidal anti-inflammatory drugs (NSAIDs).
The three main causes of peptic ulcers that can damage the digestive system’s defensive ability or result in the accumulation of digestive substances are:
- Helicobacter pylori bacteria
- Prolonged and regular use of specific painkillers and anti-inflammatories
- Other medications
These causes are further explained below:
There are also some kinds of medical treatments and therapies that contribute to the formation of ulcers. The following are factors that may result in the weakening of the mucosal barrier’s ability to protect the digestive lining. These factors increase one’s chances of developing an ulcer and can slow the process of healing of any existing ulcers:
- Medications - Aspirin (painkillers), as well as nonsteroidal anti-inflammatory drugs (NSAIDs) which include - Naproxen and ibuprofen (Motrin IB and Advil), while newer forms of these drugs include celecoxib, also known as Celebrex. These drugs can inflame or irritate the stomach and intestinal lining.
- Other medications – The combination of other medications with NSAIDs, which include steroids, selective serotonin reuptake inhibitors (SSRIs), risedronate (Actonel) and alendronate (Fosamax) can increase the risk of ulcers developing.
- Radiation therapy – Such as radiation used for the treatment of cancer may lead to ulcers or prevent healing of existing ones.
Further risk factors regarding anti-inflammatory medications and the development of ulcers include:
- Elderly people who have existing conditions such as arthritis and are taking anti-inflammatory drugs are particularly vulnerable.
- Those who have had a peptic ulcer before or have suffered from intestinal bleeding.
- Those who take anti-inflammatory drugs or aspirin have an increased risk of developing a peptic ulcer regardless of whether or not they have an H. pylori infection.
If you take these medications regularly then you should discuss what other options there are with your doctor. Particularly if you already suffer from heartburn or indigestion after taking them.
More about H. pylori bacteria
- The bacteria spread through the faeces of someone who is infected.
- The infected faeces can contaminate water or food through poor hygiene practices (usually when people don’t wash their hands after using the toilet and then handle or prepare food).
- After entering a person’s mouth, the infected faecal particles will move through the digestive tract with the contaminated water or food that was ingested.
- This is what is known as faecal-oral transmission, which is the most common form of the infection spreading.
- pylori bacteria are naturally found in the mucous layers protecting and covering the tissues of the stomach lining and the lining of the small intestine. In most cases, the bacteria do not cause any issues, unless they manage to penetrate the lining of the digestive tract and cause damage which manifests through open sores known as ulcers.
- Those who have been recently infected tend to develop their symptoms in the first few weeks after the initial infection.
- The bacterium can infect people of all ages, regardless of their socioeconomic class or race.
- It commonly infects adults, but it may be due to people being infected during childhood and carrying the bacteria with them into adulthood.
- Lower socioeconomic classes tend to have a higher infection due to their living conditions and poor practices of personal hygiene and sanitation.
- It is vital to know the difference between ulcers that are caused by the bacterium H. pylori and ulcers that are caused by medications as the treatment will be vastly different.
Other medical conditions and ulcers
Ulcers can also be linked to other medical disorders which include:
- Generalised anxiety disorder – Those who constantly worry in an excessive manner are thought to suffer from a condition known as generalised anxiety disorder, this has been linked to peptic ulcers. Prolonged anxiety and stress are known to have an effect on the production of stomach acid, resulting in an imbalance of the digestive components and penetration of the mucosal wall.
Risk factors
- Lifestyle factors – It was previously thought that spicy foods and mental stress could directly cause ulcers, however, there is a lack of hard evidence to prove this. These lifestyle factors can aggravate the symptoms of the ulcer. Thus, stress, smoking cigarettes and spicy foods are seen as risk factors rather than direct causes.
- Drinking alcohol – Anything that irritates the natural balance of digestive enzymes and stomach acid will increase one’s chances of developing a stomach ulcer. Alcohol, when consumed in excessive (sometimes even in moderate) amounts, can eventually erode and damage the mucosal wall of the stomach and increase stomach acid production. When alcohol is taken with painkillers (which is often the case as those with drinking problems may often take anti-inflammatories or aspirin to relieve their hangover symptoms), this can often result in a peptic ulcer.
Complications of a peptic ulcer
If peptic ulcers are left untreated, they may result in the below complications:
- Internal bleeding – Peptic ulcers may result in bleeding and either slow or fast blood loss. As previously mentioned, a severe loss of blood will require a blood transfusion or surgery. A slow loss of blood is evident through the vomiting of blood or a bloody or black stool.
- Obstruction – Inflammation, scarring and swelling can often be the outcome of an ulcer. These complications may block food from passing through the digestive tract leading to weight loss and vomiting.
- Infection – When peptic ulcers perforate the lining of the small intestine or stomach, this increases the risk of a severe infection developing in the abdominal cavity, this is known as peritonitis.
Who is affected by peptic ulcers?
Peptic ulcers have been shown to be a common occurrence in the general population with roughly one in ten people having a peptic ulcer at least once in their life. Stomach ulcers can affect people of all ages but are commonly seen in those who are over the age of 60. Men are more commonly affected than their female counterparts.