- Skin Growths (Benign / Non-cancerous)
- How are skin growths commonly diagnosed and treated?
- Common types of benign (non-cancerous) skin growths
- What other types of benign skin growths can occur?
- Are freckles (Ephelides) considered a type of skin growth?
- When should I worry about a marking on my skin?
Common types of benign (non-cancerous) skin growths
Skin changes with age are common for most people. It is not uncommon for a variety of different marks, such as moles and freckles, to develop as a result of sun exposure too.
Some of the most common types of non-cancerous (controlled or benign) skin growths which can develop include:
Dermatofibromas
- Characteristics: Dermal nodules (small and firm flesh-coloured, dusky red, brown or black coloured bumps) develop as a result of accumulated fibroblasts (soft tissue cells beneath the skin’s surface). The overlaying epidermis (layer of skin) is slightly thickened and ranges between 0.5 and 1.5 centimetres in diameter. Occasionally, these growths can develop a little larger. Sometimes, these growths can ‘retract’ forming a dimple in the area. Dermatofibromas can sometimes be itchy or painful to the touch, but are predominantly asymptomatic (displaying no noticeable symptoms). These growths are common among women, but are not unusually experienced in children or teenagers.
- Cause: These growths may form as multiples or as solitary lesions, often developing spontaneously following a minor trauma to the skin (for instance an insect bite).
- Diagnosis and treatment: A doctor may apply lateral pressure to the growth. Sometimes this action can cause it to dimple. These growths are usually harmless, but can be assessed through biopsy analysis if a doctor feels it necessary to differentiate it from other conditions. Dermatofibromas can be surgically removed for cosmetic reasons or if they become bothersome due to itchiness or pain, and especially if they begin changing colour, grow larger or bleed.
 Dermoid Cyst
Dermoid Cyst
- Characteristics: These saclike growths are often present at birth on the surface of the skin (usually the face, lower back, in the ovaries or even inside the skull) and are made up of hairs, sweat glands, sebaceous glands and fluid. A growth that develops internally can even contain bone fragments, cartilage or teeth. The growths typically develop slowly and can become tender to the touch when broken open (or ruptured). The growths are normally firm to the touch and painless (unless they break open). These growths have also been known to develop, although rarely, in the brain, nasal sinuses, the eyes or spinal cord.
- Cause: During foetal development the skin and multiple skin structures become trapped. The cell walls of these structures are almost identical, containing hair follicles, sweat glands and even nerves. The slow growth of these cysts means that they are often only noticed in early childhood and even adulthood.
- Diagnosis and treatment: These growths can be unsightly and for this reason alone, may be safely removed. They can also become inflamed and painful, and removed for this reason too. Inflammation and rupture of these growths can be accompanied by fever. If a cyst increases in size or changes colour, a doctor must assess the growth, which will most likely be treated with surgical removal as well. Growths which occur on the surface of the skin (often termed ‘superficial’) can mostly be removed surgically without complications. Rarer forms of dermoid cysts may require removal using special techniques. Deeper-level growths (i.e. those that are internal) may require testing to determine other possible abnormalities associated with various conditions, such as CT scans or scope procedures (and other imaging procedures). A growth should never be removed at home. A medical doctor should perform removal, ensuring that the procedure is safely done without risk of infection or bleeding. A growth can also develop again if not completely removed. Removal is done with an injected local anaesthetic and a small incision (cut into the skin) directly over the growth.
Keloids (pronounced: kee-loids)
- Characteristics: Fibrous tissue (or scar tissue) that forms following injury to the skin forms a protective scar which can grow excessively to form a smooth, hard growth. These growths can become itchy, tender and even painful or cause a burning sensation, but are mostly not a risk to your overall health. Keloids can be larger in size than the actual wound and often occur on the chest, shoulder area, cheeks and earlobes. A keloid, however, can develop anywhere on the body.
- Cause: These growths are thought to occur as a result of a collagen production defect. The most common causes include injuries to the skin such as burns, acne scars, chickenpox scars, scratches, vaccination sites, ear piercings and surgical incision sites.
- Diagnosis and treatment: Treatment can be administered with cortisone injections (to flatten the growth and reduce inflammation), pressure dressings or silicone gel pads, radiation therapy (to shrink the growth), freezing of tissue, laser removal treatments (to reduce scar tissue) and silicone gel applications or moisturising oils. Most keloids don’t typically require medical intervention, however unsightly they may be. If a keloid grows in size or develops other symptoms, you should seek assistance from your doctor, so that he or she can check for any potential problems, such as signs of skin cancer. If necessary, a biopsy can be performed to either determine or rule out any other possible medical conditions. For cosmetic reasons alone, a doctor can also treat the growth by trying to remove it. Treating keloids can be tricky as scar tissue can grow back again, and larger than before. Initial treatment may involve less invasive forms, applied frequently. Many keloids do typically shrink over time without any necessary treatment. Keloids which are quite large may be surgically removed, although as mentioned, this is not without risk of further scarring if the keloid returns.
Keratoacanthomas
- Characteristics: These growths are round or dome-shaped, often with a crater (almost resembling a small skin-coloured or red volcano) consisting of pasty material (keratin and dead skin cells). These grows typically occur on the face, neck, forearms or the back of the hands. They can also occur on the legs. These growths can clear on their own, but often leave scars and may recur. Initially the appearance of these growths can resemble a pimple or boil. They do tend to enlarge fairly quickly (within a matter of months) and reach a size of about 1.75 mm (millimetres) wide.
- Cause: These growths are linked to sun exposure, but often begin in a hair follicle on the skin. Areas of the body that are regularly exposed to the sun are most vulnerable for these growths to develop. Other possible causes that are linked with keratoacanthomas include HPV (Human papillomavirus) infections, genetics, a compromised or weakened immune system and some cancer-causing chemicals.
- Diagnosis and treatment: If this growth develops it is important to seek medical assessment from your doctor. Although, usually benign, these growths can develop into a squamous cell carcinoma (a type of skin cancer) which will require treatment. In order to assess the nature of the growth, a skin biopsy will likely be required. The tissue sample will need careful analysis under a microscope as they closely resemble those of squamous cell carcinomas. The shape and distinctive crater are important characteristics of the growth in determining it as a keratoacanthoma. Corticosteroid injections or fluorouracil injections (or creams), as well as surgical removal are the more common means of treatment for these growths. Surgical removal may involve scraping, freezing with liquid nitrogen, excision (cutting out) of the growth, or removing a layer of tissue at a time. Wounds will be sealed or stitched to allow for healing following removal. Chemotherapy medications, radiation or orally taken retinoid drugs are also means of treatment your doctor may consider. It is advisable to have these growths checked and treated as they can recur or spread to other areas of the body.
 Moles (pigmented nevi)
Moles (pigmented nevi)
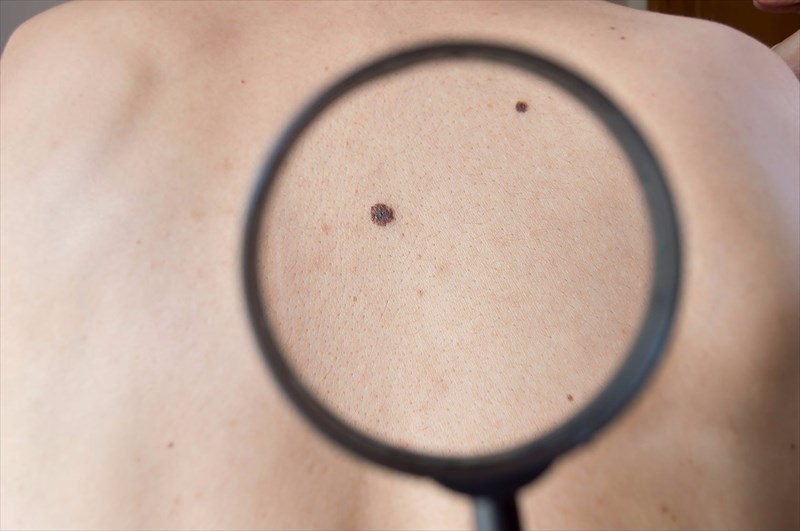
- Characteristics: Moles are typically brown or black in colour (sometimes flesh-coloured or yellowish), and are usually benign rounded skin growths (usually symmetrical with a uniform colour and regular borders) that often begin in childhood and can continue throughout a person’s lifetime. Pigmented nevi, or moles, are known to consistently change shape or colour over time, making some more prone to developing cancerous cells (melanoma) than others. Moles can be smooth or rough (some contain hair), as well as flat or raised in appearance. Changes to moles can also sometimes be as a physical response to hormonal adjustments in the body. These growths can appear anywhere on the body, alone or in clusters.
- Cause: When skin cells (melanocytes) grow in clusters (in one spot) instead of spreading throughout the skin, pigment that gives skin its natural colour can darken with sun exposure. Causes of moles are strongly linked to genes, in combination with the amount of sun exposure experienced, especially during childhood. It has been noted that skin that has been exposed to sun often tends to have more moles. These growths are also more commonly found in those who are prone to freckles (ephelides) – those with paler complexions.
Diagnosis and treatment: In many cases, moles can lighten and disappear on their own over time. When this happens, the body effectively causes a regression by “attacking the unusual formation”. As such, many moles, whether lightened or not, may never require treatment at all. Any noticeable changes to a mole must be checked by a medical doctor as soon as possible for a thorough physical assessment and possibly a biopsy as well. Not all enlarging moles are cause for alarm and may not become malignant (cancerous). Some enlarge and darken during pregnancy and do not pose a threat to a woman’s health at all. A biopsy of any mole being assessed can help to determine irregularity. Those to be concerned about will display changes in size and colour, as well as other symptomatic signs such as bleeding. These may be examined periodically, treated or removed altogether. If detected early many melanoma types can be diagnosed, and cured with appropriate treatment. Surgical removal for cosmetic reasons is also acceptable if desired. Moles should never be treated with lightening or fading creams, bleaches or other chemicals. A medical doctor must perform any desired or necessary removal. Scarring can occur and can be treated with creams, gels laser treatments or cortisone injections.
Atypical moles (dysplastic nevi)
- Characteristics: These moles are normally larger than pigmented nevi and are irregular in shape (not always rounded). The colour of these moles is often uneven with darker centres and lighter, patchy or jagged edges. Typical colours are tan or a dark brown shade, sometimes surrounding by a pinkish area of skin. Atypical moles can occur anywhere on the body, and are often flat (nearly or completely) in appearance. A person who has between 20 and 25 atypical or irregular moles on the body will need to have them checked by a medical doctor, as the risk for skin cancer (melanoma) increases. Some people have been known to have as many as 100 atypical moles on their body. Risk may be increased, but not all atypical moles will develop into skin cancer.
- Cause: These moles are typically passed through family genes (i.e. they are hereditary – from parent to child). The combination of genes and sun exposure to various parts of the skin can cause atypical moles. These growths are more common with people who have experienced severe sunburn or who have chronically sun-exposed areas of their body, such as the upper back and shoulders, head, neck and ears, as well as the lower legs and calves. Sun exposure on an atypical mole can accelerate changes to its appearance.
- Diagnosis and treatment: Diagnosis and treatment is similar to that of pigmented nevi. Removal of the mole can be done for both health and cosmetic reasons.
Pyogenic granulomas
- Characteristics: Small, round and often blood red, brown or bluish-black in colour, these growths form as raised marks on the surface of the skin. They can develop at any age, affecting both men and women (especially during pregnancy). Hormonal changes in the body can lead to the development of these growths. Pyogenic granulomas initially grow quickly over a period of a few weeks, after which they begin to form a raised, reddish nodule. Growths can either be completely smooth or have a slightly rough or crusty surface. They typically occur on the face, neck, arms, hands, fingers, back and genitals. They can also develop on the eyelids and lips too. Although rare, these can develop on the cornea of the eye (or conjunctiva), the clear covering protecting the iris and pupil. During pregnancy, hormonal changes can lead to the development of these growths on the gums. These are often referred to as ‘pregnancy tumours’.
- Cause: Pyogenic granulomas (also known as lobular capillary haemangioma or granuloma telangiectaticum) typically form as a result of excessive capillary (small blood vessel) growth and swelling. This can happen following injury to the skin or for those who bleed easily. Injury can be as a result of insect bites, scratching of the skin (broken skin), hormonal changes in the body, as well as certain medications (such as birth control or oral contraceptive pills). The actual growths are prone to bleeding as they contain a large number of small blood vessels. They can bleed for quite a while, so it is best not to pick at one or scratch it.
- Diagnosis and treatment: The only thing to really be concerned about when it comes to these growths is how easily they rupture and bleed. They are almost always non-cancerous and thus don’t typically pose a threat to your overall health. They can be removed, but must be done by a medical doctor who ensure to remove the growth completely. If not removed completely, these growths can recur. In many instances, pyogenic granulomas clear on their own. A diagnosis is likely to be made during a physical examination, but a doctor may recommend a biopsy to either confirm or rule out any possibility of malignancy or other underlying conditions. Treatment may depend on the size and location of the growth on the body, but must be performed by a medical doctor to ensure the entire growth is handled with care (during removal or when using appropriate tools for bleeding control). Small growths may be left alone to clear in time, as they often do naturally. Larger growths may be removed by scraping and cauterisation (burning). This can prevent bleeding and considerably reduce the possibility of recurrence. Larger growths can also be surgically removed and the wound stitched up. A doctor can also opt to treat bleeding of the growth by applying chemicals, such as silver nitrate, or remove it in a less invasive way using laser surgery. Growths may be left alone during pregnancy, and removed thereafter if they do not resolve themselves during the time it takes for the body to adjust in the months following birth.
Seborrheic keratoses
- Characteristics: These growths typically develop with age (especially after middle age and older). A seborrheic keratosis is usually a round or oval shaped, wart-like growth that looks like a separate object that has been stuck down on the skin’s surface. These growths are normally flesh-coloured, white, tan, yellow, brown or black in colour (hyperpigmented), occurring more commonly on the scalp, back, shoulders, abdomen or chest. They can, however, occur anywhere on the body but do not usually develop on the palms or soles of the feet. The growths enlarge slowly in clusters or on their own and are often roughly textured, bumpy, scaly (hyperkeratotic) or grainy (crumble easily). Sometimes they can also have a smoother, raised texture which is waxy. Seborrheic keratoses are often mistaken for moles, warts, skin tags or melanoma, but are more often than not, benign (not harmful at all).
- Cause: Age and frequent sun exposure do appear to be linked as common causes (or underlying reasons) for development. These growths do appear to run in families, so genetics may play a role too. Risk may increase according the number of blood relatives with the skin condition.
- Diagnosis and treatment: A doctor can diagnose these growths during a physical examination, but may order a biopsy if he or she feels necessary for confirmation, as well as to potentially rule out any other underlying health / medical conditions. Although the growths are not usually harmful, it is a good idea not to ignore them. Any change to the skin is best assessed by a medical doctor. It can happen that a person experiences a sudden eruption of these growths. This normally signals some form of internal malignancy which will need medical evaluation (testing) for diagnosis and treatment. The appearance of melanoma (a serious form of skin cancer) and seborrheic keratoses are quite similar. Thus, a doctor should assess them to be sure, especially if the appearance of a growth begins to change (size and colour). A doctor should check any growth that changes in size, shape (develops irregular borders which are jagged or blurred), colour (especially if the growth becomes blue, purple or reddish-black), swollen, inflamed or ruptures (causing bleeding). If the growth is small and is not a cause for further concern, a doctor may not implement any treatment procedures. If requested any growth can be safely removed for cosmetic reasons. Removal can be done via cryosurgery (frozen off with liquid nitrogen), electro-surgery (high frequency electrical current applied to the tissue to cut, scrape or desiccate it) or curettage (a scraping technique in a scoop-like manoeuvre).
Skin Tags
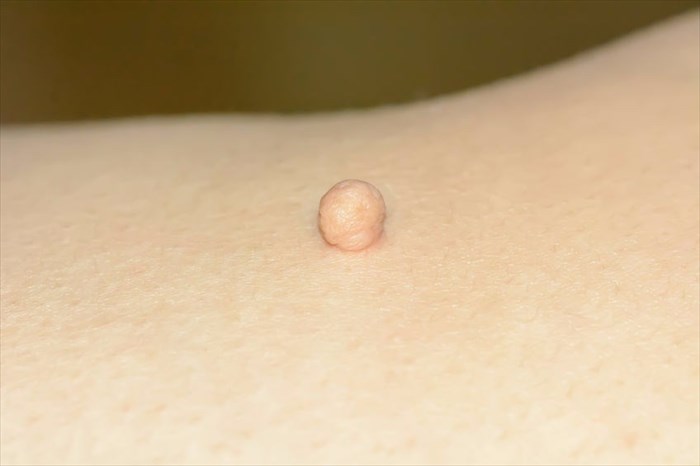
- Characteristics: These growths, also known as fibroepithelial polyps, acrochordons, cutaneous papillomas, and soft fibromas, are small, soft flaps of skin tissue that appear on the surface of the body. Most skin tags are harmless and do not pose a threat to a person’s health or cause any discomfort for pain. A hiccup in blood circulation in the affected area may result in some discomfort, but not necessarily pain. Skin tags are common around areas of the eyelids, neck, back, chest, armpits, beneath the breasts or in the folds of the groin and buttocks. As such they are exposed to contact and can cause irritation when rubbed against clothing etc. These growths look a little like small, soft, smooth balloons of skin, suspended on a slender stalk, and can vary in numbers (from just one up to a 100). These growths can form as small as a flat pinhead-sized bump of the skin or grow as big as a large grape.
- Cause: Skin tags have been noted as more common amongst women, especially those who are middle-aged or elderly, or who have gained weight. A distinctive cause is not entirely known. It is thought that tags may occur as a result of skin surfaces rubbing against one another (hence the reason why some areas of the body more commonly experience tags than other parts). Skin tags are common amongst pregnant women too. The reason for this is thought to be changes in hormones during the 9-month gestation period.
- Diagnosis and treatment: Skin tags are more often than not, completely harmless. Some may even spontaneously fall off the body on their own. Many aren’t likely to be bothersome or become cancerous (if left alone untreated), but they can be a little unsightly. They can be removed for cosmetic reasons or if they become bothersome. A doctor will assess the tag and diagnose by sight. Tags can sometimes resemble growths caused by other conditions, such as accessory tragus or an accessory digit. If questionable (especially if a tag grows, displays multiple colours or begins to bleed), a biopsy of tissue can be done to assess for other conditions or check if the growth has become precancerous. A biopsy may also be done for larger growths. For the most part, skin tags can be removed with a scalpel or scissors, an electro-surgery (burning off with an electric current) or cryosurgery (freezing with liquid nitrogen). Skin tags can recur and aren’t preventable.

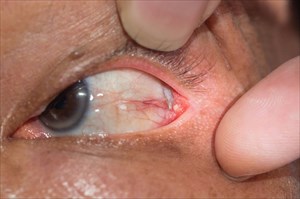 Dermoid Cyst
Dermoid Cyst
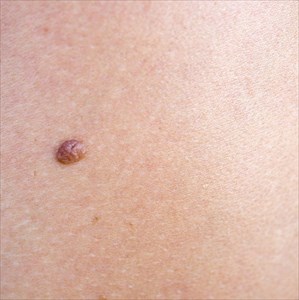 Moles (pigmented nevi)
Moles (pigmented nevi)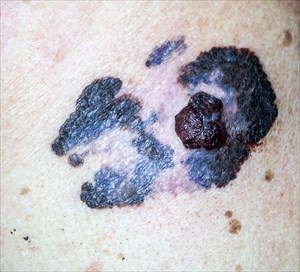 Diagnosis and treatment:
Diagnosis and treatment: