- Colonoscopy
- Why do I need a colonoscopy?
- What are the risks for a colonoscopy?
- How do I prepare for my colonoscopy?
- What should I expect when having a colonoscopy?
- What do my colonoscopy results mean?
- Factors that may affect your colonoscopy and what to know about the procedure
- I have some more questions regarding my colonoscopy…
What should I expect when having a colonoscopy?
Prior to the procedure
You will generally be admitted to hospital as a day patient, and once you have checked in you will be assigned a bed in the day ward and given forms detailing personal and medical information as well as emergency contacts.
You will be issued a standard hospital gown (that opens at the back) and asked to change into it (having your own gown to put over it may make you feel more comfortable).
Nursing staff will take your vitals (pulse and blood pressure) and if you are undergoing sedation for the procedure, the anaesthesiologist supervising this procedure will visit you to take a full medical history, find out if you have any allergies and discuss the sedation process with you.
You will generally not be offered any medication to calm your nerves before the procedure as these may coat the bowel and obstruct the view thereof.
Once the doctor is ready to perform the procedure, you will be wheeled into the procedure room. People in the room during the procedure will include the gastroenterologist performing the procedure, the anaesthetist and one or two nursing staff and/or assistants.
During the procedure, you will only wear a gown and nothing else (underwear is removed for obvious reasons).
While some doctors may allow patients to be conscious for the procedure, most gastroenterologists will recommend that you undergo some form of sedation, not just for your own comfort but also to allow the procedure to proceed swiftly and without interruption.
Depending on your doctor’s recommendations, one of the following forms of sedation may be administered:
- Conscious or “Twilight” Sedation: This is a mild to moderate form of sedation using a combination of sedatives (usually Propofol or benzodiazepine) and pain medications that are administered intravenously (via a vein in your arm). Depending on the depth of the sedation, this will either leave you feeling comfortable and relaxed but not completely unconscious (you will be aware of and able to respond to auditory and tactile cues), or you may undergo a deeper form of sedation after which you will have absolutely no recollection of the procedure and feel as though you slept through the entire process.
- General Anaesthesia: This is generally not a preferred method for colonoscopies, however, if it is used, it will be administered by a trained anaesthesiologist using a combination of Propofol (Diprivan) and pain medications. You will not be conscious or responsive during the procedure, and a breathing tube for airway support will be required.
- The SEDASYS®System: Some professionally trained gastroenterologists and nursing teams may use this FDA-approved system to induce mild to moderate sedation with Propofol without the presence of an anaesthesiologist.
**My Med Memo: The names “Propofol” and “Benzodiazepine” may be familiar to you as the administration of these were associated with the death of Michael Jackson in 2009. This should, however, not make you feel anxious as his death was due to inappropriate and irresponsible use of these medications and numerous clinical studies have shown that when used appropriately and administered by a trained anaesthesiologist or doctor in the correct doses, these drugs are safe and effective for use in sedation for a colonoscopy.
During the colonoscopy
Prior to being sedated, you will be asked to lie on your side (usually the right side as this results in greater comfort and a quicker procedure time) on the examination table, having your knees drawn upwards towards the area of your chest.
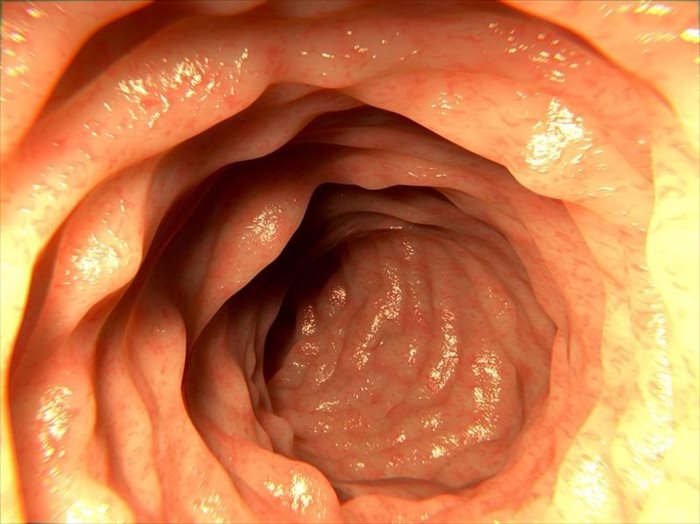
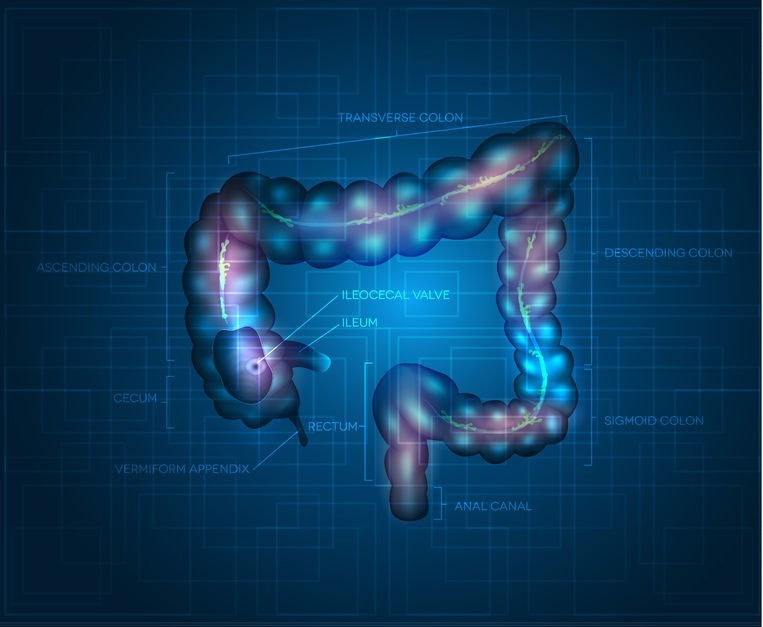
When you are sedated, your doctor will insert the colonoscope into your rectum. The scope is long enough to reach the entire length of the colon. It will also contain a tube, known as a channel and a light that will allow for your doctor to inflate the colon with air, this allows for a clear view of the inner lining of the colon. As the scope moves through your colon, air will be pumped into it. This may create abdominal cramping or the urge to go to the toilet once the procedure is complete.
The scope also has a small camera at the tip of it to record images of the colon and send them to a monitor for your doctor to record and get a clear view of the lining of the colon. Your doctor may also insert small instruments through the channel to take some tissue samples known as biopsies, or to remove any abnormal tissue or polyps.
A colonoscopy is a relatively quick procedure and will take 20 minutes to an hour at most, depending on the findings and whether abnormal tissue or polyps need to be removed.
How the colonoscopy feels
As stated, the colon prep prior to the actual colonoscopy is often reported as being the worst part of the entire procedure for most patients as it results in diarrhoea, some mild cramping and anal discomfort.
In general, if you undergo any form of sedation for the procedure you will feel extremely relaxed or sleep throughout the procedure and have no recall of it afterwards.
If you are conscious during the procedure, however, then you may have some pain when the scope moves through the colon, and may feel the need to have a bowel movement or pass gas. If the pain you feel is unmanageable, then it is best that you tell your doctor. The machine used to remove secretions and stools is a suction machine and does not cause pain, but it can be noisy.
After the test, you may experience cramping and bloating and be very gassy from the air that was pumped into your colon. Flatulence is a normal side effect and although it may seem embarrassing, you should not try to hold the gas in as this can increase cramping. Nursing staff are trained professionals and will generally handle any flatulence you experience after the procedure with humour as they try to put you at ease.
If you had a biopsy during the procedure, or if anything abnormal was removed or polyps, then you may have mild discomfort at the site of the biopsy or a slightly bloody stool for a couple of days post the procedure.
After the colonoscopy
Once the exam is over, it will take you about 45 minutes to an hour to ‘wake up’ from the sedative. Even if you were conscious during the procedure, you may not remember anything if a light sedative was administered.
It is generally advised that you arrange for someone to drive you home after the procedure, as the sedative may make you feel drowsy and will often take a few days to fully wear off. It is best to go home and rest and not go back to work on the same day.
If a polyp was removed during the colonoscopy, your doctor may recommend that you stick to a specific diet for a couple of days to aid in the recovery of your colon.
Sometimes walking a few hours after your procedure can help pass the gas you are experiencing.
When you have your first bowel movement, small amounts of blood in your stool is normal after this exam. Contact your doctor should you develop a high fever, have severe abdominal pain that is persistent, or if excessive blood is present when having a bowel movement.