What happens during an ultrasound scan?
Ultrasound imaging is based on sonar principles similar to those used by ships, bats and fisherman. Sound that strikes an object reflects or bounces back (echoes). The echo waves (small pulses of high-frequency sound waves) enable identification of an object, as well as its distance, size, shape and consistency.
In the field of medicine, these echoes assist with identifying the appearance, size (or contour) and consistency of tissues, blood vessels, organs and other structures, including masses and tumours. The sensitive nature of the transducer records every tiny detail change in sound wave pitch and direction, and these are instantly measured to create real-time images. An ultrasound scan can record still frame visuals of moving pictures, or short video loops.
When it comes time for the ultrasound scan (normally within a hospital radiology environment, outpatient clinic or at some general practitioner offices), a radiologist or technician (sonographer) will request that all jewellery be removed, as well as necessary items of clothing. For instance, before a breast ultrasound, a woman will be asked to remove all clothing from the top half of her body and wear the medical or hospital gown provided.
From there, a person will be asked to lie down on a table in a comfortable manner which exposes the portion of the body being examined. A contrast dye can be injected into a vein should it be safe to do so (i.e. the person being examined does not have any allergies to the contrast substance) and if it can help the radiologist or technician with being able to obtain a clear visual during the scan.
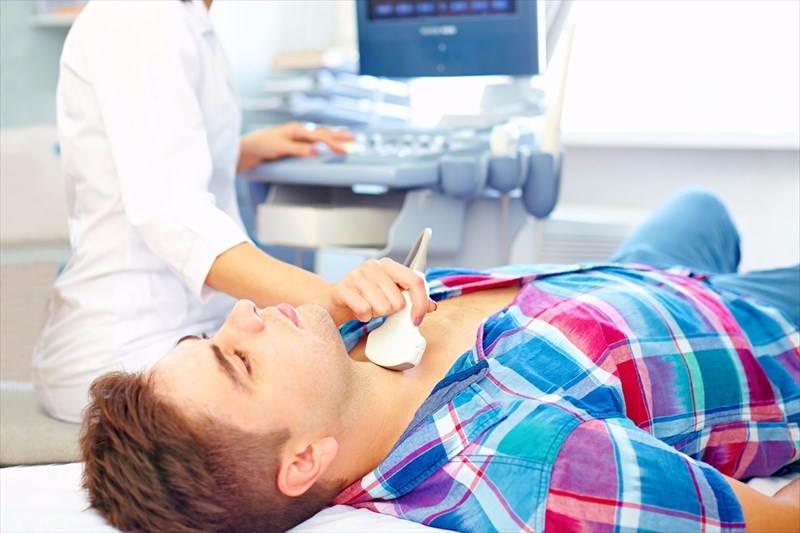
If the thyroid is being examined, a radiologist or technician will place a soft pillow at the back of a patient’s neck in order to tilt the head backwards and expose the throat area. This can be a little uncomfortable, but is not painful. Sometimes a patient can sit upright for a thyroid ultrasound.
For an external ultrasound, the radiologist or technician will then apply a lubricating water-based gel to the skin in the area being examined. This is done to prevent friction and air pockets when the ultrasound transducer (hand-held device) is applied to the skin, as well as to assist with transmitting sound waves during the scan. The gel may feel a little cold at first but warms up once the transducer is applied and moved around.
Once in motion, the transducer emits high-frequency sound waves through the body, returning echoes as they connect with dense structures or objects (like organs and bones). A visual is created and can be viewed in real-time on a computer monitor for interpretation by the doctor or technician. The sound waves will not be heard as they are at too high a pitch for the human ear.
During the examination, a person may be asked to adjust their position in order to provide the doctor or technician with easier access to the specific area being examined. A doctor or technician will analyse the visuals in real-time, assess specific markers and make notes during the examination.
During a musculoskeletal examination, a person may be asked to sit on a chair or examination table, or alternatively lie face-up or face-down on an examination table. He/she may also be asked to move portions of the body being examined (joints, muscles, tendons or ligaments) in order to determine functionality.
A woman having a breast ultrasound will be asked to raise her arm above her head for the duration of the scan procedure.
If an ultrasound is to be done internally, a small transducer (with a protective cover or sheath) is attached to a probe (thin, flexible tube) which will then be inserted into a natural opening of the body – oesophagus, rectum or vagina. If a transducer is to be inserted into the oesophagus (using an endoscope with a light attachment) through the mouth to examine a portion of the digestive system, a radiologist or technician will normally ensure patient comfort by administering a sedative for the scan.
A transvaginal ultrasound will require an empty bladder before being inserted into the vagina. The small tip of the transducer has a protective cover (or sheath) and will be lubricated with a small amount of the clear water-based gel before being used. Images taken are done from different angles in order to obtain the best possible views for interpretation. This ultrasound is done to view a woman’s endometrium and determine its thickness, as well as identify any ovarian problems or abnormalities. A sonohysterography is performed to obtain a more detailed view of potential abnormalities.
For a sonohysterography, a sterile saline will be injected into the uterine cavity. This is done to enlarge the uterus and produce a better visual. The injected saline effectively outlines the endometrium, making it easier to see and identify abnormalities such as masses or polyps within the uterine cavity. If the radiologist or technician wishes to look for air bubbles in the fallopian tubes (which could indicate blockages or patency), saline air may be injected into the uterus.
A transvaginal ultrasound may be done as a baseline exam and if necessary, a sterile speculum will replace the transvaginal probe for further examination. A radiologist or technician will cleanse the cervix before inserting the catheter or probe.
In the case of a child requiring an ultrasound examination, it is best to try and explain the nature of the scan to them beforehand so as to minimise any surprises which may raise anxiety levels. A doctor may also advise that familiar comforts be brought along to the examination room on the day, such as toys or books. Sometimes a television can be put on to distract a little one while the examination is taking place.
A typical scan can last between 15 minutes and an hour, depending on the nature of the examination. The entire process of an external scan is normally painless, sometimes with some temporary, but mild discomfort. Any discomfort or pressure felt normally occurs when the transducer is moved around over an area of sensitivity, such as a full bladder or if pain in the area was already being experienced. A patient must inform the radiologist or technician if any pain or discomfort intensifies or worsens during the scan. Some discomfort can be experienced during a transrectal ultrasound if a biopsy is necessary and a needle inserted to retrieve a tissue sample. Most scans are, however, well tolerated by patients.
Unless a sedative has been given, a person will normally be completely awake and alert throughout the process. An internal scan is a little less comfortable to experience (especially when a transducer is inserted) than one performed externally, and does carry a slight risk of some internal bleeding. Some occasional cramping may be experienced during a sonohysterogram when saline is injected. To curb this, a doctor may recommend some over-the-counter medications to be taken beforehand to help minimise discomfort. A woman may also experience some light vaginal spotting in the days following the procedure.
Once an external scan has been completed, the lubricating gel will be cleaned off of the skin and a person will be able to return home or go about normal daily activity shortly thereafter. The gel tends to dry quickly and does not discolour or stain clothing that may come into contact with it. There are generally no harmful side-effects following a scan. If a sedative was used, a person should not drive and arrange for safe transport home after the procedure.
Interpreting the results
A technician will make notes for a full analysis to be discussed during a later consultation or follow-up. Test results may be produced as still images or a video loop recording for analysis by a radiologist.
Once visuals have been analysed and interpreted, a comprehensive report will be compiled and signed by the radiologist, and given to the treating doctor or physician. The referring medical professional will then discuss the report results with the patient.
Depending on the nature of the results, follow-up examinations or tests may be necessary. If another testing or screening procedure is necessary due to the presence of an abnormality which requires further evaluation, or one which requires periodic monitoring, a doctor will discuss the need in detail.
Sometimes, a follow-up may require a biopsy of a suspicious mass or lump. Additional follow-up tests may be recommended to determine underlying causes and rule out various conditions, or diagnose a possible illness.
Follow-up scans may also be required during a treatment process in order to determine whether or not the chosen treatment programme is working.
If a doctor is able to make a diagnosis based on the results of ultrasound screening, a treatment plan may be implemented immediately.

