Rhinoplasty (overview)
Rhinoplasty is one of the most common types of plastic surgery, and is also well known as a ‘nose job’. Rhinoplasty is a surgical procedure that reshapes the nose by modifying the bone or cartilage for both aesthetic and functional purposes.
The procedure can enlarge the nose or make it smaller, as well as change the angle in relation to the upper lip, correct indentations, bumps or other defects, as well as alter the tip of the nose.
The most common reasons for a rhinoplasty procedure are to change the appearance of the nose (aesthetic) or improve a person’s quality of breathing.
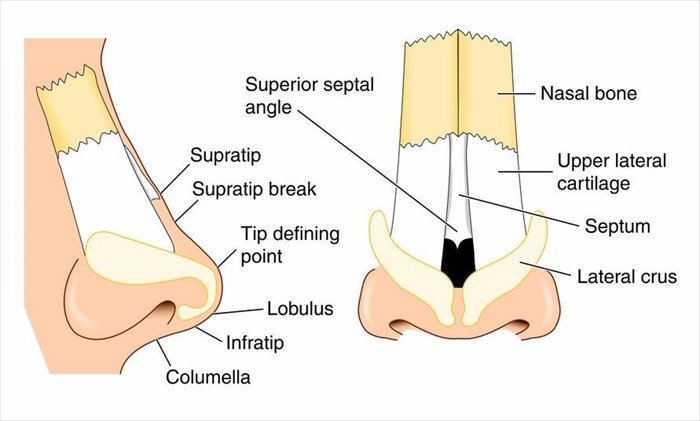
The upper portion of the nose structure is bone and the lower, cartilage. A rhinoplasty procedure modifies the cartilage and bone structure, as well as the skin surrounding it. A plastic surgeon may require additional material to augment (enhance or reinforce) the nose. Materials commonly used include alloplasts (synthetic implants), alloenous materials (these are obtained from cadavers) or autologous implants (materials harvested from a patient’s own tissue, usually the rib or fascia).
Functional reasons for this type of procedure include providing structural support for areas of the nose that are deficient of material (upper or lower lateral cartilages), and allowing a person to breathe a little more effectively.
Aesthetic reasons include increasing the projection of the nose (the nasal dorsum) in profile view (correct the proportion of the nose in relation to the rest of the face) and modifying the nasal tip. Grafts may be placed to camouflage any irregularities of the upper or lower lateral cartilage or the bony dorsum.
Surgeons qualified to perform rhinoplasty procedures are typically trained in plastic surgery, otolaryngology (specialising in the ears, nose and throat), or both.
A plastic surgeon will take into careful consideration your facial features, the skin on your nose and what specifically you would like to change. He or she will then discuss whether this procedure is appropriate for you and whether it can achieve your desired result.
If it is agreed that you are a candidate for surgery, a customised plan will be developed for you. Depending on your medical health insurance plan, some or the entire procedure may be covered. Procedures, purely for cosmetic reasons may not be covered at all and you will need to cover the costs independently.
Why is rhinoplasty done?
Changing the shape of the nose purposefully to repair, correct, or alter its appearance is done for both aesthetic and functional (health) reasons. Some may require a rhinoplasty procedure to repair abnormalities due to an injury, correct breathing problems or birth defects. Others primarily wish to make aesthetic adjustments to their nose.
Changes a plastic surgeon can make include:
- Adjusting the size and angle of the nose
- Straightening the bridge of the nose
- Reshaping the tip of the nose
- Narrowing the nostrils
An aesthetic adjustment should only be done when the nasal bone is fully grown. For females, growth tends to stop at around the age of 15 or 16, while boys may still be growing into their late teens (17 – 18 years of age). If the purpose of a rhinoplasty procedure is to correct a breathing impairment or chronic congestion, surgery can take place at a younger age.
Other Articles of Interest

Cinderella Surgery
Walking in heels is not exactly a walk in the park. The question is, how far would you go to fit into a great pair of heels?

Breast Augmentation
A cosmetic surgical procedure to increase the size and volume of a woman's breasts, a 'boob job' (breast augmentation) should be carefully considered. Here's everything you need to consider...
Botox
Botox, the miracle treatment for wrinkles and the reason why so many modern men and women seem to defy aging. But it also does more than this. Read on to find out all you need to know...