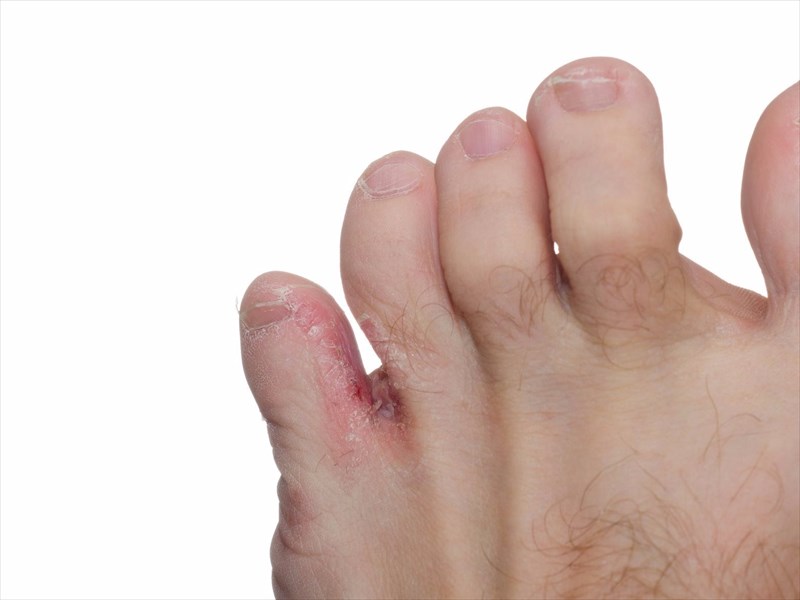
General signs and symptoms which are most common in athlete’s foot infections include:
- Skin which is red (rash-like and raw), dry or moist and / or flaky, cracked (fissuring) and scaly lesions (peeling) – especially in the toe webbing and / or soles
- Soggy skin
- Itchy skin (or varying degrees of stinging or burning sensations) – that often worsens when shoes and socks are removed
- Small blisters (which may be painful) or ulcers (which may leak fluid)
Athletes foot may affect one or both feet at one time. A ‘two feet, one hand’ pattern is fairly common with fungal growth spreading to the hands via direct contact (i.e. scratching or picking) with infected feet.
Hand fungal infections are known as tinea manuum. Infection can spread to the toenails as well. Some fungal infections result in rash-like, red, raw and blistery symptoms, while others produce thick, dry and scaly types of effects.
Types of Athlete's Foot
The different types of athlete’s foot are5:
- Toe web infections: Infections are initially seen between the fourth and fifth toes, which appear scaly (or peeling) and cracked. Infection can spread to the rest of the foot, particularly the soles. Also known as an interdigital infection, the skin becomes red (inflamed), rash-like, scaly or peeling and may give off a smelly discharge. In severe instances, the skin may turn green in colour.
- Moccasin infections: The first signs of infection may be a little soreness on the sole of the foot, and skin along the heel may become thick, itchy and cracked (dry). Dryness and scaling (which can resemble eczema) can extend from the soles up the sides of the feet. Toenails can also discolour and thicken when infected, and begin to crumble. Toenails may also pull away from the nail bed, and in some cases, loosen and fall out. If toenails are infected, combination treatment may be required (toenails are required to be treated separately).
- Vesicular infections: This type of infection may begin with an outbreak of tiny fluid-filled blisters (which may be itchy and / or painful), usually along the soles of the feet. Blisters can surface anywhere on the foot, however, and can sometimes be accompanied by a bacterial infection as well (if blisters burst open). Open sores or ulcers can also develop causing a bacterial ulcerative infection. These can become inflamed, painful and may ooze. Signs of a bacterial infection can include a honey-yellow crust on the foot, redness, swelling, warmth and pain.
How to tell the difference between athlete’s foot and psoriasis
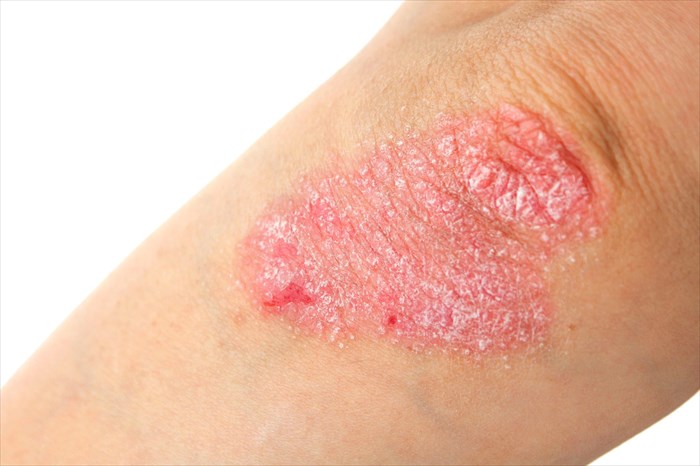
Psoriasis is a genetic autoimmune condition6 which is not as a result of a fungal infection, and is not contagious. In the case of psoriasis, skin cells are produced at a faster rate than is normal, accumulating on the surface of the skin. The skin cells do not fall off naturally and instead develop into thick scales and / or white/silver patches. The result is dry and itchy skin which can also be painful. The condition can either affect just a small area of the body or in some patients, cover large areas.
Symptoms between the two skin conditions are a little similar, but there are a few differences:
- Psoriasis: Skin is covered by scales and red patches, which may be painful. Dry cracked skin may also bleed. Joints may also become swollen and painful, and nails may thicken or become pitted.
- Athlete’s foot: Skin may be red and scaly (peeling).
- Both: Itching or burning sensations on or around red, rash-like areas of skin.
Location on the body may also be a tell-tale sign
The feet are the main area of the body affected by athlete’s foot, with the potential for the infection to spread elsewhere. Patches of skin irritation that occur around the knees, elbows, back, trunk etc. are more typical of psoriasis than a fungal infection (athlete’s foot).
Athlete’s foot may be easily treated with anti-fungal ointments and creams which can be bought over-the-counter. Psoriasis is not likely to clear with the use of the same ointments and works better with the use of systemic medications which slow down the production of skin cells.
When in doubt, a consultation with a medical doctor can help to clarify which of the two conditions a person may have. This can be done with a physical inspection of the affected areas of the body (physical examination) and a laboratory test (using a sample).
References:
5. HealthLinkBC (British Columbia). October 2017. Athlete's Foot: https://www.healthlinkbc.ca/health-topics/hw28392 [Accessed 29.08.2018]
6. National Center for Advancing Translational Sciences. Psoriasis: https://rarediseases.info.nih.gov/diseases/10262/psoriasis [Accessed 29.08.2018]