Fungal infections such as athlete's foot do not generally clear up on their own. It is best to begin treating infection as soon as minor symptoms appear. Antifungal treatments are usually recommended, much of which are available over-the-counter. If these do not show signs of improvement, it is best to consult a doctor for further assessment. It is important to remember that not all foot irritation is necessarily as a result of a fungal infection and may involve other bacterial infections.
Antifungal treatments work to prevent the fungus that is causing infection from spreading or multiplying any further (hindering growth). (8) Treatments are available in cream / lotion, spray, powder or liquid forms. A doctor or pharmacist will recommend an antifungal treatment that is most suitable for a person’s age (child, adult or senior). Pregnant or breastfeeding women and children may not be able to use certain products. Pregnant women will also not likely be prescribed oral medications due to risk to an unborn baby.
A doctor or pharmacist will recommend that they be used in the following way:
- Affected areas should be washed and dried thoroughly (including between the toes).
- Hands should be washed and dried thoroughly after touching affected skin and before and after applying any medications.
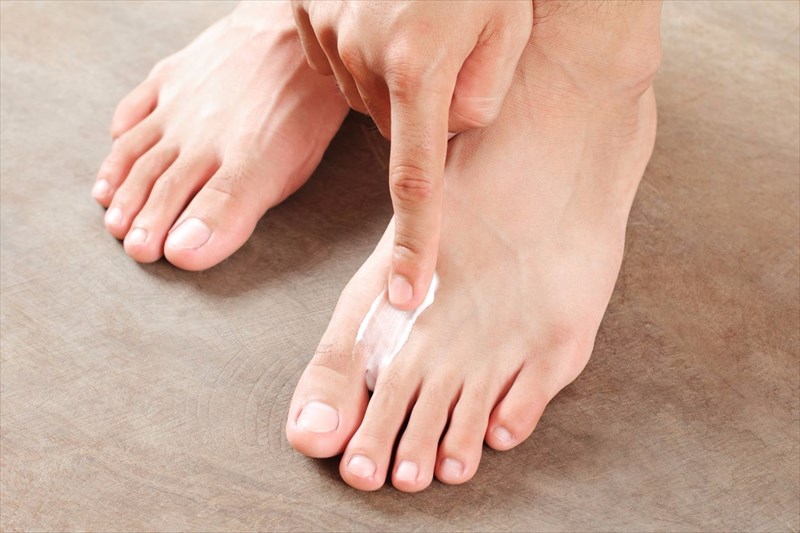
- Antifungal treatment (i.e. cream, powder, spray or liquid) is directly applied to the affected skin. A small amount is usually all that is needed for at least one application a day.
Itchiness and pain may be alleviated with the use of a mild steroid cream for a short period of time as well. Your doctor may prescribe these creams to be used at the same time as antifungal treatment products to help with the symptoms but they do not help clear the fungal infection.
Treatment should be continued even when symptoms begin to clear which in mild cases is usually within a week). You should continue with the treatment for at least one week after symptoms clear and may safely continue your treatment for up to 4 weeks after the symptoms have cleared. This is to ensure that the fungus clears completely and has little chance of recurring. If symptoms do not appear to be clearing and are still highly uncomfortable after about a week, antifungal medications of prescription strength may be recommended by a doctor. He or she may also request blood tests to ensure sufficient liver function before prescribing medications which may be stronger in order to combat more resistant instances of athlete’s foot.
A doctor or pharmacist may also recommend antiperspirant sprays containing aluminium chloride (Drysol) for those who tend to sweat a lot. Powders may also be recommended to alleviate moisture on the feet.
If an infection has spread to the toenails, this must be treated as well so as to avoid potential reinfection. Treatment for infected toenails may require separate treatment products but should be administered at the same time as treatment for the remainder of the foot. Fungal nail infections are more difficult to treat and require recommended oral antifungal medications for at least 12 weeks. (9)
Along with the application of antifungal treatments, a doctor will suggest good foot hygiene habits, as well as adjustments which promote a clean, dry (moisture-free) and friction-free environment. It may be recommended that vinyl shoe materials be avoided as these promote moisture when worn, which does not help to keep potential fungal infections at bay. Wearing sandals in communal areas where fungi are likely to thrive will also help to keep risk of infections low.
Clean, absorbent socks (leggings or stockings) are best to wear, and should be changed if feet become sweaty or moist. The insoles of shoes can also be removed from shoes, so as to allow them to dry out when not worn. Shoes and socks can also be dusted with powder (medicated antifungal powder or even talcum powder) to help decrease moisture when worn. It can also help to alternate pairs of shoes, and not wear the same pair every day. This can help to allow for time to dry out a pair of shoes for a day or two before being worn again.
A doctor or pharmacist will also recommend that skin not be torn, picked at or scraped off during treatment as this can result in healthy skin cells becoming infected (and spreading the fungi).
Mild cases of athlete’s foot typically respond well to antifungal treatments, but can recur. Severe cases must be seen, diagnosed and treated by a medical doctor.
Home remedies for athlete's foot
Can a vinegar foot soak alleviate athlete’s foot?
Studies have looked into whether foot baths containing vinegar may have healing properties. Vinegar is effectively a diluted form of acetic acid, which may have antifungal healing properties. Vinegar is capable of working as a disinfectant which can also reduce bad odours.
Mild cases of athlete’s foot may benefit from a vinegar based solution foot soak, especially if toenails have become infected as well.
To make a foot bath solution, use 1-part vinegar to 2 parts water. Before submerging feet into the solution, they should be thoroughly washed with soap and water. Feet can be soaked in a solution at night, cleaned, moisturised or treated with antifungal products before bed.
A 10 to 15-minute daily soak for several weeks (or until signs of infection subside) is a relatively inexpensive way to help alleviate symptoms of fungal infection. The vinegar odour is a strong one but does tend to subside once feet are dry.
There’s little harm in giving feet a vinegar bath, but if symptoms worsen it is best to see your doctor for further advice on the foot soaking and for possibly other treatment options.
Listerine for athlete's foot
A bold mouthwash product that is formulated to kill up to 99% of bad breath germs that cause gingivitis and cavities, has been used by some in a similar foot soak bath for the treatment of athlete’s foot. Some have been known to use Listerine on their feet for the removal of dead skin cells, as well for treating fungal infections (including those of the toenails). The thinking in using this product is associated with known antifungal properties in thymol and menthol – two ingredients in Listerine.
Does it work?
Studies have not been able to clinically prove that Listerine use is an effective antifungal treatment. Some studies have only focussed on fungal infections in the mouth, however, and not the feet. As yet, it has not been clinically proven that the antifungal properties in the mouthwash are in fact an effective treatment for fungi affecting the feet and nails. As a mouthwash, however, antibacterial and antifungal properties are proven to be effective. A foot bath with this ingredient may not necessarily cause any further harm or side-effects, but may not be the most effective means to clear an infection. It is advisable to seek treatment from a medical doctor or pharmacist instead.
Alternative natural remedies for athlete's foot
There are several other alternative means that have been tried for treating fungal infections. Some may provide relief, such as alleviating inflammation, but as yet, have not been entirely clinically proven to treat infections such as athlete’s foot any more effectively than over-the-counter and prescription medications.
Before trying any home or natural remedy it is best to talk to a pharmacist or medical doctor.
Some natural alternatives which have been tried include:
- Tea tree oil (10): Oil produced from the leaves of the tea tree (also known as melaleuca) is known to have antiseptic properties which can kill off certain types of fungi and bacteria. Tea tree oil is an ingredient in many home treatment products on the market. Tea tree oil rubbed into the skin may help reduce swelling, itching and burning sensations associated with athlete’s foot, but is not a proven remedy for everyone who uses it. For some people, it can cause side-effects of skin irritation, such as rash or trigger an allergy. Sometimes dilution of a product can alleviate side-effects. Tea tree oil should never be taken orally as it can be toxic to the body.
- Bitter orange: Some studies have found that watered down (diluted) bitter orange oil with regular applications can help to alleviate symptoms of athlete’s foot. (11) Undiluted, bitter orange oil can cause skin irritation and inflammation, and can also make the skin more vulnerable to sunburn if not protected with a sun exposure cream.
- Ajoene: A natural chemical found in garlic, ajoene has been tested in studies to see the effects on athlete’s foot symptoms. Taken in a gel form or orally, symptoms in at least one study showed relief within a week. (12)
- Green tea: Polyphenols in green tea are known to help with alleviating redness (or inflammation). Studies have not yet determined whether the antifungal properties in green tea can actually cure athlete’s foot. It may be that a good, regular soak in green tea simply makes feet feel a little better. (13)
Outlook for athlete’s foot
Mild infections typically clear up within a few weeks, responding well to antifungal treatments. Severe cases may take a few months to clear. Recurrences are common, but if treated when symptoms first begin, the spreading of the infection is prevented. For some who are more prone to infections, long-term treatment may be necessary.
References:
8. Pubmed Health.June 2018. Athlete's Foot: Overview: https://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0072733/ [Accessed 29.08.2018]
9. Centers for Disease Control and Prevention. January 2017. Fungal Nail Infections: https://www.cdc.gov/fungal/nail-infections.html [Accessed 29.08.2018]
10. US National Library of Medicine - National Institutes of Health. 1992. Tea tree oil in the treatment of tinea pedis: https://www.ncbi.nlm.nih.gov/pubmed/1303075 [Accessed 29.08.2018]
11. National Center for Complementary and Integrative Health. September 2016. Bitter Orange: https://nccih.nih.gov/health/bitterorange [Accessed 29.08.2018]
12. US National Library of Medicine - National Institutes of Health. 1996. Efficacy of ajoene, an organosulphur derived from garlic, in the short-term therapy of tinea pedis: https://www.ncbi.nlm.nih.gov/pubmed/9009665 [Accessed 29.08.2018]
13. US National Library of Medicine - National Institutes of Health. June - September 2013. Effects of a foot bath containing green tea polyphenols on interdigital tinea pedis: https://www.ncbi.nlm.nih.gov/pubmed/23499394 [Accessed 29.08.2018]
