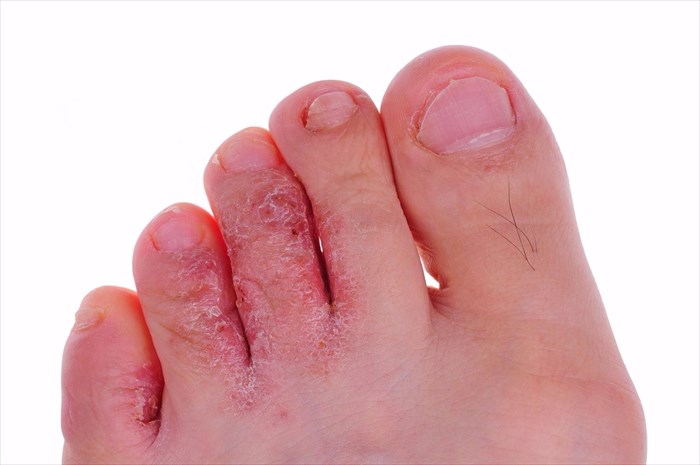
What is athlete's foot?
Tinea pedis, more commonly known as athlete’s foot, is characterised as an inflammatory fungal infection of the skin between the toes (toe webs), the soles of the feet, or on the heels. The condition can cause red (inflamed), raw and cracked skin eruptions or blisters, scaly flakes or on occasion, oozing or weeping wounds. The skin usually becomes itchy or has sensations of burning or stinging. An infection can spread to the toenails1, and sometimes the hands too.
Feet that are exposed to warmth and moisture provide an ideal environment for fungal growth. As many as 70% of the world’s population may develop athlete’s foot at some point in their lives.
Athlete’s foot is not classified as a serious condition, but must be treated so as to prevent spreading of the fungus to other parts of the body or to another person. It can easily be picked up from contaminated surfaces such as flooring, shared clothes or towels which have been in contact with infected feet.
Athlete’s foot can be difficult to ‘cure’ as it is common to experience recurring infections. Anyone is vulnerable to contracting this fungal infection, irrespective of age or gender.
The condition is also often called ‘jungle rot’ by armed forces serving in areas with tropical climates, and is closely related to other fungus causing infections such as jock itch and ringworm.
What causes athlete’s foot?
Dermatophytes are the group of fungi (tinea fungus) that causes athlete’s foot. The fungus grows on (or inside) the top layer of skin (epidermis) and multiplies, thriving on warmth and moisture. The webbing between the toes is usually where an infection first occurs as a result. An environment which is closed, dark, lacking airflow, moist and warm (humid), offers fungi the opportunity to feed on keratin (the protein which is found in the skin, nails and hair) and then multiply.
Athlete’s foot is easily spread by an infected person walking around barefoot or having touched their infected feet and then touching other surfaces. It is common for the infection to spread through skin particles left on the floors of public gyms, showers, lockers rooms, spa facilities, nail salons or swimming pools. (2)
Infection can also spread with the sharing of socks, shoes or other clothing and towels, which has been in contact with the fungus. Simply touching the feet or toes of an infected person (direct contact) can also spread the fungus.
References:
1. Centers for Disease Control and Prevention. January 2017. Fungal Nail Infections: https://www.cdc.gov/fungal/nail-infections.html [Accessed 29.08.2018]
2. Pubmed Health. June 2018. Athlete's Foot: Overview: https://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0072733/ [Accessed 29.08.2018]
Other Articles of Interest

Eczema (Atopic Dermatitis)
Atopic dermatitis is the most commonly seen type of eczema. This article unpacks the condition, the causes, symptoms and also explores other types of eczema...
Diabetes (Diabetes Mellitus)
Diabetes (diabetes mellitus) is a long-term disease that requires daily management and care. The illness refer to a group of metabolic health conditions. Learn more about the different types.
Candida
Candida is a type of fungus that naturally resides in our bodies. When it overgrows it can result in oral thrush, genital candidiasis, and in more severe cases, invasive candidiasis...