In mild cases of croup, it is often not necessary to seek medical intervention. Most children will return to normal within a week.
If at any point a parent or caretaker develops concern or a child does not appear to be responding favourably to home treatment, precautionary measures are advisable. Any symptoms which do not improve or if these seem to worsen must be evaluated by a medical doctor. Seeking medical assistance in the case of severe symptoms is essential and must be done as soon as possible (i.e. treated as an emergency).
At a medical consultation, a doctor may ask questions in order to determine the underlying causal nature of symptoms. This will help to determine the best course of treatment too.
Questions can include:
- What symptoms have you noticed the child experiencing?
- For how long have symptoms been present?
- Has the child been feverish? Has this happened once or on more than one occasion? Did you take a temperature measurement? If so, how?
- Have you noted any difficulties with the child being able to swallow?
- Has the child had croup before?
- Has the child ever had any other upper airway problems leading to breathing difficulties?
- Has the child recently been exposed to others who have been unwell (such as individuals with signs of a viral infection)?
- Has the child’s cough worsened? If so, how quickly has the cough become worse?
- Does the child’s cough appear to be worse at night?
- Does the child have any other known medical conditions (such as asthma or an allergy)?
- Is the child currently taking any medications? If so, what and for how long?
- Has the child been fully immunised? (This is usually to assess routine vaccinations, specifically immunisations against the bacteria Haemophilus influenzae type B / Hib which can lead to complications of epiglottitis infections)
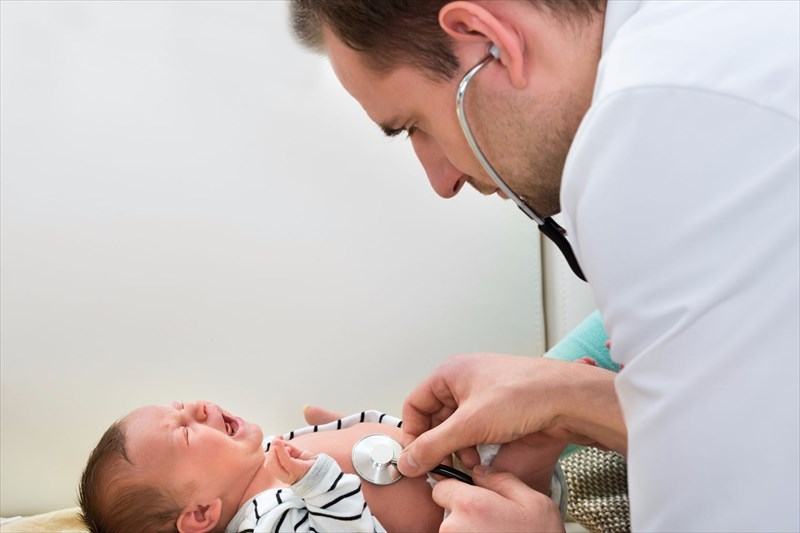
A doctor will then proceed to perform a physical examination of the child. He or she will observe the child’s breathing (and also listen to it with a stethoscope), as well as listen to the sounds of the cough and stridor. Normally a diagnosis can be made during the physical exam by observing characteristic symptoms alone.
If necessary, a throat exam or X-ray to assess the nature of narrowed airways (normally the top of the airway appears narrowed on an X-ray forming a ‘steeple sign’) may be recommended so as to rule out any other respiratory conditions which may be causing similar symptoms.
Laboratory tests which may be recommended are usually reserved for severe cases of croup and are only really necessary if there are any suspected bacterial causes. Sometimes a consultation with an ENT physician (ear, nose and throat specialist) or otolaryngologist may be recommended especially if there is concern of upper airway anatomical malformations. In this instance, a fibreoptic laryngoscopy may be recommended to provide a more direct visual of the airways.
