Which medical professionals should be consulted for Deep Vein Thrombosis?
- Primary healthcare provider (family physician) / general practitioner (GP)
- Emergency medical personnel
- Haematologist (may be consulted if there is presence of a blood disorder)
- Interventional radiologist (may be required to dissolve or remove a blood clot)
How is a Deep Vein Thrombosis diagnosed?
A diagnosis for deep vein thrombosis will be made based on:
- A medical history and symptom discussion
- A physical examination
- The results of a variety of tests
A doctor will try and identify all symptoms, risk factors for DVT and assess ways to rule out any other potential causes. In some cases, where a pulmonary embolism has already developed, emergency diagnosis and treatment will be necessary (i.e. bypassing the routine diagnosis of DVT).
During the medical history discussion, a doctor will determine a person’s overall state of health, known symptoms and their nature (mild or severe), as well as ask a variety of questions. These can include:
- Has there been a period of time recently where you have been inactive? (I.e. sitting or lying down for long periods)
- How long ago did symptoms begin?
- Do symptoms appear to come and go (i.e. ease off and then return) or are symptoms continuously bothersome?
- How would you rate severity of your symptoms?
- Have you tried anything that has appeared to worsen or improve symptoms?
- Are you currently taking any over-the-counter or prescription medications? If so, what? And for how long?
- Have you recently had any injuries or surgical procedures?
- Have you been diagnosed with any other medical conditions, such as cancer? Has any treatment been received? If so, what?
From there, a doctor will perform a physical examination and assess the affected areas for the characteristic signs of deep vein thrombosis, such as oedema (swelling), tenderness (or pain) or visible redness and discolouration. Heart and lung function will also be checked and a blood pressure reading taken.
Tests which a doctor may recommend include:
- Blood tests: An elevated level of D-dimer is normally present in the bloodstream when a blood clot forms and gradually dissolves. D-dimer is a small protein fragment known as FDP (fibrin degradation product). A blood sample may be requested for laboratory analysis to pick up the presence of D-dimer if a DVT clot is suspected. This test will be used as an indicator of a potential thrombus in the system. If an elevated D-dimer is found, an imaging test will usually follow the blood result in order to confirm and make a diagnosis. It is important to note that D-dimer tests can often produce a 'false-positive' result. This means that a result can be positive but a patient does not show signs of DVT. D-dimer tests can also be influenced by other medical conditions such as inflammation.
An international normalized ratio (INR), partial thromboplastin time (PTT) and full blood count will also usually be assessed. Any other blood samples for testing will be based on an individual's condition. If there are signs of another illness or disorder which could be an underlying cause, relevant blood tests will likely be recommended – either to confirm a diagnosis or rule out factors which will not be impacted by a specific treatment plan. Inherited blood disorders, for instance, can cause recurrent blood clots which can occur anywhere in the body. It is important to determine the location of the clot, especially if present in the kidneys, liver or brain. Once an underlying cause is determined, a diagnosis can be made, further relevant testing done and an appropriate treatment plan implemented.
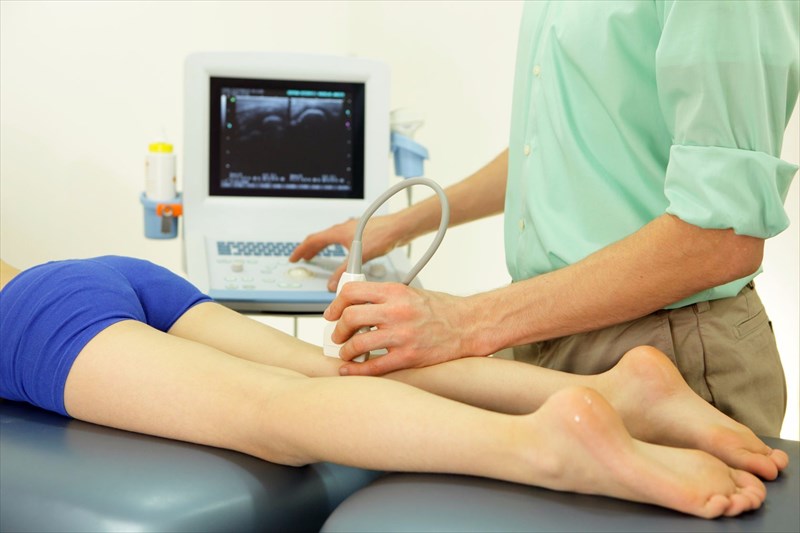
- Ultrasound scan: A gel is spread over the affected area. A transducer (wand-like device) will then be placed over the affected area in order to pick up any sound waves which are caused by a blood clot in the system. Sound waves travel through the body’s tissues and reflect back (as relayed echoes), creating a moving image on the ultrasound scan monitor. This then produces an image of the blood clot which makes for a visible diagnosis. An ultrasound scan can also help a doctor (or ultrasound technician) to determine the size of the clot, and whether it is a new formation or possibly a chronic occurrence. A series of scans can sometimes be done over a few days to determine if a blood clot is growing in size (or dissolving), or to identify the formation of any new clots. It may be more complicated to detect clots when they occur below the knee, in the pelvis or chest areas. Other imaging tests may be preferable in these instances.
- Venography: A doctor will inject a radioactive dye into a vein, normally in the ankle or at the top of the foot. The dye helps to ‘show up’ any abnormalities in the system and will assist with visualising the presence of a clot. From there an X-ray will be performed to create a visual of the veins in the lower extremities. This helps a doctor to identify and diagnose a blood clot, as well as determine whether blood flow is slower than it should be. Generally, many doctors prefer an ultrasound to this means of testing. A venography may, however, be done as an alternative to an ultrasound or if perhaps an ultrasound result was not as clear.
- MRI or CT scans: Other imaging tests can include magnetic resonance imaging (MRI) or computerised tomography (CT) scans. These can provide detailed internal images which can show up blood clots. These may be used to see clots which are rooted much deeper in the body, such as in the pelvis, especially if these can’t be picked up on an ultrasound or X-ray.
- VQ scan (lung ventilation perfusion scan): Should DVT have worsened and there are signs of pulmonary embolism at the time of a consultation, a doctor may recommend this scan to assess the nature of blood flow and oxygen levels in the lungs. This is necessary to determine how much oxygenated blood is reaching the lungs (or not) before adequate treatment is implemented.
