Treatment for deep vein thrombosis focusses on three critical things – preventing the blood clot (thrombus) from growing any larger, averting the potential for the development of new clots, and thwarting risk for developing a life-threatening complication, such as a pulmonary embolism.
A treatment plan may involve the following:
1. Medication (anticoagulants)
Blood thinners may be prescribed to combat clotting, as well as help to treat existing clots in the system by preventing them from becoming larger. This effectively allows the body to break down the clot naturally. Blood thinning medications also actively lower a person’s chances of developing new clots. Blood thinners or anticoagulant drugs effectively interfere with the process that forms blood clots (known as the clotting cascade). Common medications that have been popularly prescribed include Heparin (injected via syringe just under the skin or within a vein in the arm) and Warfarin / Coumadin (in oral pill form). Both drugs require medical monitoring while being taken.
Medications, known as Xa-inhibitors (injectable and oral forms) are also available for use with effective results – these include apixaban, dalteparin and dabigatran (direct thrombin inhibitor), to name a few. These medications have notably fewer interactions with other drugs, diet (foods and vitamins) or dietary changes. Prescribed anticoagulants are typically taken for at least 3 months (sometimes longer) once treatment commences in order to both treat and prevent clots. Some medications are prescribed as injectables for a few days, after which others will be prescribed to be taken orally.
An alternative to blood thinners is thrombolytic medications / agents (also known as clot busters), which work by breaking up clots directly through the use of a catheter (often with the guidance of an X-ray). These medications are normally used if blood thinners have failed to sufficiently treat the clot or where DVT is diagnosed as severe (with high risk of complications such as severe pain, large clots, clots in the arm or serious risk of a pulmonary embolism). The drugs will be administered intravenously (IV line) so as to enter the system quickly and rapidly get to work, but the patient will be carefully monitored as there is an increased risk for life-threatening complications.
If a doctor feels that the vein containing the clot is too narrow, he or she may widen it with a balloon angioplasty procedure or place a stent so as to alleviate symptoms and reduce the risk of future blockages. It’s important to take any prescribed medications exactly as recommended and also keep a treating doctor well in-the-know regarding the need for any other substances, such as medications and supplements that are being taken. These will need to be very carefully managed. Any medications that are not taken at prescribed doses (too little or too much) can result in serious side-effects. Pregnant women must disclose their condition as certain medications can result in birth defects if taken.
2. Surgery for DVT
Filters
A surgical procedure known as a vena cava filter (or IVC filter) may be recommended if anticoagulants are not a viable treatment option. The small, cone-shaped filter is placed inside the vena cava vein (a large abdominal vein) so as to prevent (by catching a clot) the possibility of a pulmonary embolism (entering the lungs). The filter does not prevent blood flow from circulating, just the clot.
Venous thrombectomy
Rarely, a blood clot will need to be surgically removed (i.e. cut out). This procedure is reserved for severe cases which do not respond well to any other treatment methods.
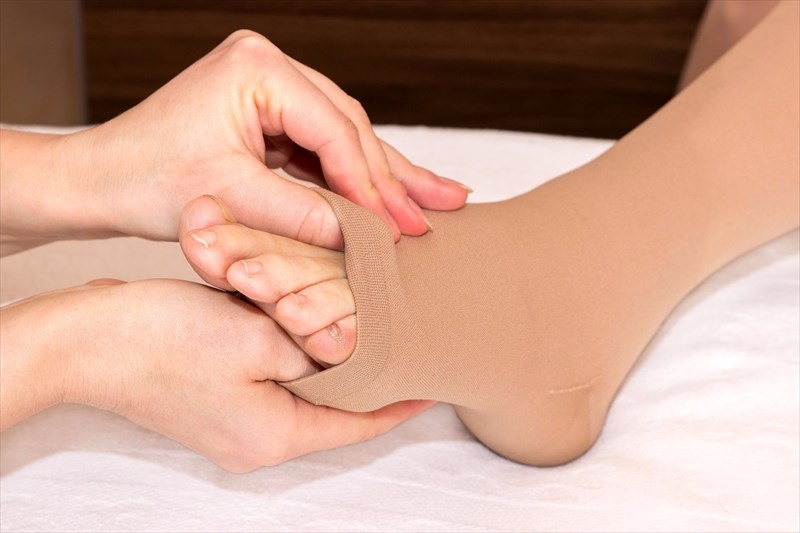
3. Compression stockings (graduated or medical)
A doctor may also recommend these to alleviate swelling and help to significantly reduce the development of new blood clots. Stockings are generally worn over the feet and are long enough to reach just below or a little above the knee. They are tight at the ankles and gradually become looser as they reach the knee. These can safely be worn daily to help alleviate the symptoms of DVT (reducing the chances of blood pooling and clotting in the veins) by assisting with contraction. Stockings can be worn for extended periods of time if need be. Three types are available for wearing – support pantyhose (offering the least pressure), over-the-counter compression hose (providing more pressure) and prescription-strength compression hose (these afford the greatest amount of pressure and are fitted specifically by a trained professional).
What are some of the risks with anticoagulation medications (therapy treatment)?
The main concern with taking blood thinners is bleeding. A doctor will have carefully assessed this risk over the potential benefit for treatment and advise appropriate steps to ensure the safest means of implementing treatment with selected medications. Side-effects include major trauma such as bleeding on the brain or stroke.
How does Warfarin (Coumadin) interact with diet?
If Warfarin, as an anticoagulant is prescribed for the treatment of DVT, a doctor will advise on how to take the medication in a safe and effective way. Blood clots must be treated so as to avoid serious complications, such as a pulmonary embolism, heart attack or stroke.
It has been noted, that the drug does interact with certain foodstuffs and liquids and this must be taken into consideration at the beginning of treatment.
The drug is designed to interfere with the way blood clots (i.e. its clotting factors) and thereby reduces risk. Clotting factors essentially assist blood with clumping together, forming a clot. Each and every person has 13 types of clotting factors in their system. Vitamin K-dependent clotting factors (Factors II, VII, IX and X and protein C and S) are the types that Warfarin deactivates.
The drug effectively decreases the amount of vitamin K in the body, which the affects the bloods ability to clot naturally. All clotting factors are needed to do their bit to maintain the process and keep the body at its most healthy. The body itself produces consistent levels of vitamin K, but can also obtain it from dietary means. This is where care must be taken. An excess of the vitamin, in short, renders the medication ineffective and continues to disrupt normal clotting capabilities, thus placing a person at higher risk for bleeding.
Foods which a doctor may recommend limiting or avoiding include:
- Spinach and chard
- Green lettuce
- Kale
- Parsley
- Collard and mustard greens
- Brussels sprouts
- Endive (Cichorium)
- Red cabbage
- Green tea
- Cranberry and grapefruit juice
- Alcohol
Many leafy greens contain vitamin K, as does green tea and can make the drug less effective in the treatment of DVT. Juices such as cranberry and grapefruit, as well as alcoholic beverages can considerably increase the chances of internal bleeding while taking the drug. For this reason, the above will all be on the list of things to ‘avoid’ once treatment with the medication has commenced.
A doctor will also warn against the use of certain medications and supplements, including herbal products as these too, can have adverse effects.
Substances known to have adverse interactions with Warfarin include:
- Antibiotics
- Medications for seizures
- Some anti-inflammatory drugs
- Oral contraceptive pills (birth control pills)
- Some anti-depressants
- Certain antacids
- Other anticoagulants or blood thinners (namely aspirin or heparin)
- Garlic
- Gingko biloba
- St. John’s wort
- Co-enzyme Q10
The most common adverse reactions include:
- Allergic reactions
- Rash
- Itchy skin
- Gastrointestinal problems or disorders
- Disorders or problems with the liver and or / gallbladder
- The chills
- Hair loss
- Inflammation of the blood vessels
- Excessive bleeding (bruises and open wounds or cuts)
- Skin tissue damage or death (clots which block oxygen flow to the skin and cause deterioration and pain)
Tips a doctor may provide when prescribing Warfarin
- Keep any treating doctor in-the-know regarding all medications, supplements, herbal products etc. being taken or which one is interested in taking for specific health purposes.
- Refrain from making any dramatic changes to one’s diet without the knowledge of the treating doctor.
Home care for deep vein thrombosis
Care beyond the doctor’s office or hospital is just as important. A doctor will have carefully discussed risk factors and signs of potential complications to watch out for once treatment commences. Excessive bleeding may be sudden or a new clot may form.
- Maintain regular appointments with the treating doctor: Frequent check-ups may be required, especially with regards to the taking of certain medications. Some medications need to be monitored and blood tests will be required to ensure that blood is flowing and clotting in a normal manner. A doctor will generally assess uncomplicated DVT occurrences at the 3-month mark and determine if further treatment is necessary. Any other underlying conditions or chronic clots may require a longer treatment period.
- Take medications exactly as prescribed: Any medication must be taken as recommended by a treating doctor. Blood thinners (anticoagulants) can lead to sudden bleeding which can quickly become excessive. A doctor will thus advise for care to be taken with activities while on the medication because any cut or bruise (including minor injuries) can rapidly become serious, and require prompt medical attention.
- Movement: It’s important for those who are able to move around as much as possible. This will help to prevent the formation of any new clots. A doctor can best advise safe means to move, especially if a person is recovering from a surgical procedure or has been on bed rest for some time prior to DVT.
- Wearing compression stockings: If these have been recommended, it is important to continue wearing them daily.

