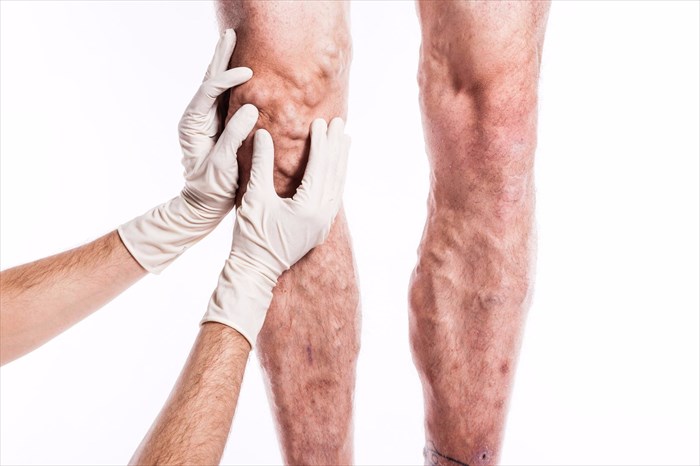
What causes deep vein thrombosis?
When blood is prevented from clotting normally or does not circulate as it should (becoming stagnant), abnormal clots form and disrupt the natural flow. Microscopic clots consistently form in the body, but are routinely broken down safely, without causing harm or damage. An imbalance in the formation and breakdown process can lead to significant clotting (thrombus).
Factors which can contribute to the formation of DVT blood clots include:
1. Limited movement or immobility: Examples which cause muscles to remain lax and promote the slowing down of blood circulation include:
- ‘Economy class syndrome’ or prolonged travel where a person is sitting or lying down for an extended period of time (in an airplane, car or train)
- A period of hospitalisation (including after a surgical procedure)
- Obesity
- Pregnancy (along with the added pressure of a growing baby on the pelvis and veins in the legs, as well as in the initial 6 to 8 weeks following birth).
2. Hypercoagulability: DVT can occur when blood coagulates faster than normal. Substances and factors which can lead to hypercoagulability include:
- The taking of medications such as oral contraceptives (birth control pills) and hormone replacement therapy (HRT) containing oestrogens
- Immune responses and bruising in the extremities
- Smoking (causes blood cells to become stickier, easily forming clots along the wall linings of blood vessels)
- Conditions such as cancer, irritable bowel syndrome, heart disease or polycythaemia (increased production of red blood cells)
- A hereditary disposition to the formation of clots (blood conditions which genetically cause blood to thicken)
- Complications which arise following an invasive procedure (surgery)
3. Injury / trauma: DVT can sometimes happen when an injury to a blood vessels or surrounding tissue occurs. Reasons for this can include:
- Trauma or injury to the lower leg (slowing blood flow)
- Injury or trauma to the veins due to fractures
- Inflammation
- Surgical intervention
- Complications which arise following an invasive procedure (surgery)
Symptoms of deep vein thrombosis
Not every instance of deep vein thrombosis shows up symptoms. This can sometimes result in a discovery of the condition once hospitalised and receiving treatment for a complication of DVT, such as a pulmonary embolism. Swelling and pain are the most commonly recognised signs of DVT and typically occur in approximately half of all cases (1). Symptoms mostly occur in one leg (sometimes the arm), and very rarely both.
Those who do experience symptoms most commonly note the following:
- Oedema (swelling) in the leg (typically on one side), the ankle and or / foot (this often comes without warning)
- Cramping pain (typically begins with a little soreness in the calf) and or / a severe pain in the ankle and feet (especially noticeable when trying to stand or walk)
- Warm skin sensations on affected areas (erythema of the skin)
- Skin discolouration (blanching / becoming pale, red and blue) of the affected areas
- Enlarged veins (visible to the naked eye)
- Tired legs (legs which feel sluggish, tired and or / achy)
Blood clots which occur in the superficial venous system (closer to the skin’s surface) may result in symptoms (signs of inflammation) of redness, tenderness, swelling and sensations of warmth. A vein can sometimes be felt – like a thickened, firm cord.
Any signs of DVT must be evaluated and appropriately treated by a medical professional as soon as possible, ideally before complications arise.
Signs that deep vein thrombosis may have escalated or worsened, requiring immediate medical care, include:
- Chest pain or discomfort in the chest area which worsens when taking in a breath or coughing
- A sudden shortness of breath
- Rapid pulse and or / irregular heartbeat
- A sudden coughing spell (especially if accompanied by the coughing up of blood)
- Dizziness / light-headedness (low blood pressure)
- Fainting
Reference:
1. National Heart, Blood and Lung Institute. 28 October 2011. What is Deep Vein Thrombosis: https://www.nhlbi.nih.gov/health/health-topics/topics/dvt [Accessed 05.09.2017]