- Gum disease (Periodontitis)
- What is the difference between periodontitis and gingivitis?
- What are the stages of periodontitis?
- What are the symptoms of periodontitis?
- What are the different types of periodontitis?
- What are the causes, risk factors and prevention for periodontitis?
- How is periodontitis diagnosed and treated?
- FAQ regarding gum disease
What are the causes, risk factors and prevention for periodontitis?
What causes periodontitis?
The majority of cases of periodontitis begin with plaque (the sticky coating on your teeth that is mostly composed of bacteria). When plaque is not cleaned off the teeth through daily brushing and flossing, plaque build-up can advance, causing infection and ultimately periodontitis. The following explains this progression:
- Plaque will form on your teeth when the sugar and starch found in the food that you eat interacts with the bacteria that naturally reside in your mouth. Flossing daily (once a day is adequate) and brushing your teeth twice a day will aid in removing plaque. It is necessary to brush and floss your teeth daily as plaque re-forms at a rapid rate.
- Plaque may harden under the gum-line and form into tartar if it is not removed. Tartar, also known as calculus, has a higher quantity of bacteria and cannot be removed through brushing and flossing alone. An oral hygienist or dentist will have to professionally remove the tartar. The longer plaque and tartar remain, the more likely they are to do harm and damage to your gums and teeth.
- Plaque can lead to the mildest form of periodontitis, being gingivitis. This is the inflammation and irritation of the gums (gingiva). This condition can be reversed through sound oral hygiene practice and regular professional cleaning.
- When gum inflammation is not treated, it can result in periodontitis. Gum inflammation can cause pockets to develop and deepen between the teeth and gums when they fill with bacteria, plaque and tartar as the infection progresses. If this inflammation is left untreated and infection occurs, then these deep pocket formations can result in the loss of bone and tissue, and eventually the loss of teeth. This ongoing inflammation may also put strain on the immune system as it tries to defend itself and fight off the infection.
What are the risk and prevention factors for periodontitis?
The bacteria found in plaque are the most prominent cause of periodontitis. However, there are a number of other factors that may also have a role to play in the development of gum disease. These include medications, oral hygiene habits and some diseases. The factors that can increase the risk of gum disease developing can also worsen the infection should gum disease already be present.
These contributing/risk factors include:
- Genetics – Some may be more susceptible to gum disease than others due to their genes. However, genes do not make gum disease an inevitable condition as those who have a higher chance of gum disease developing are able to control and even prevent periodontal disease through sound oral hygiene and care.
- Smoking cigarettes and the use of tobacco products – Smoking will increase your risk of developing gum disease. It will also adversely impact the infection should you smoke when you have periodontitis, as smoking may increase your resistance to treatment. If you smoke, you may find that you have more tartar build-up on your teeth and develop deeper pockets between your teeth and gums due to gum disease. The nicotine found in cigarettes can result in less blood flow to your gums, thus masking the condition until it has reached a point of considerable severity. Stopping smoking can greatly increase your chances of undergoing successful treatment and recovery.
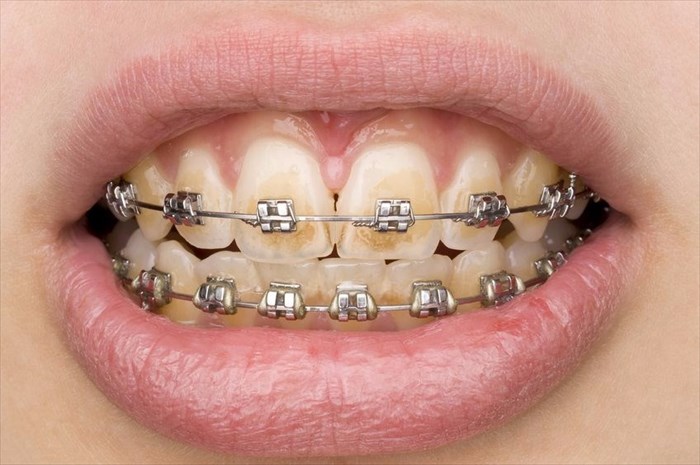
- Crowded or misaligned teeth, bridgework or braces – If there is any kind of obstruction that makes it hard to floss and brush your teeth, your chances of infection are increased due to the formation of tartar and plaque in hard to reach areas. Your dentist or periodontist may be able to show you different techniques to apply in which you can slide the floss under your braces or clean around and between the crowded teeth. You may also be referred to an orthodontist. An orthodontist is a kind of dentist who specialises in the straightening of crooked teeth and misaligned jaws. Ultimately, any dental issue you have regarding crooked teeth, braces and bridgework should be corrected as further complications can arise because of these conditions.
- Gritting, grinding and/or clenching your teeth – Habits such as these do not directly cause periodontitis, they do however, lead to a more severe form of the condition should you already have gum inflammation (gingivitis). The progression of the infection as a result of these actions is due to the excess force that is placed on the teeth, this pressure has been seen to speed up the rate at which the periodontal bone and ligament break down to occur. In the majority of cases, these actions are a result of stress or frustration. Recognising these behaviours and becoming conscious of when you are performing them can aid in stopping them entirely. Some people may battle to stop habits such as teeth grinding as these are actions that they perform in their sleep. If you are unable to stop one of these habits, despite applying breathing techniques and finding other ways through which tension can be relieved, then your dentist may create a custom mouth guard to protect your teeth from grinding and help relieve some of the pressure associated with gritting and clenching teeth. This device is often referred to as a night guard, occlusal guard, bite guard or mouth guard, and is typically worn at night whilst sleeping.
- Stress – Elevated levels of stress can result in the rapid progression of periodontitis and contribute to the infection’s resistance to treatment. The extra hormones released during stress, cortisol being the main one, result in interference with memory and learning and lower the functioning ability of the immune system, which in turn results in a number of additional complications. When your immune system is compromised, this makes it difficult for your body to fight off an infection and heal adequately, this is seen particularly in the cases of infections related to gum disease.
- Fluctuating hormones – If your hormone levels fluctuate, due to puberty, pregnancy or menopause, this may temporarily put you at risk of infection. Fluctuations in the female hormones progesterone and oestrogen can cause blood flow in the gums to be increased which may affect the way that the gum tissue reacts to certain irritants such as plaque and bacteria, thus, the gingiva become inflamed and tender, bleeding more easily.
- Medications – There are several different kinds of medications that can result in dry mouth, also known as xerostomia. Certain drugs that are used for hypertension (high blood pressure) and depression are some examples of these medications. When you do not have an adequate amount of saliva, then the formation of plaque is more likely. Some other medications may result in the enlargement of the gingiva. This creates a more susceptible environment for bacteria and debris to be caught in. Some of the medications that have oral side effects include:
- Phenytoin (Dilantin) – This is used for the treatment of seizures
- Cyclosporine (Sandimmune, Neoral) – Used to control and supress the immune system during and after an organ transplant
- Nifedipine (Cardizem, Adalat) – These are used for the treatment of high blood pressure, angina (chest pain), heart arrhythmias and are known as calcium channel blockers.
- Diseases – Those who suffer from certain conditions and diseases are more likely to develop gum disease. One such example of this risk group includes those who suffer from systemic conditions such as diabetes. This same group is also more likely to have more severe cases of gum disease with additional complications and faster progression of the infection.
- Poor nutrition – Having a healthy and balanced diet is a vital factor for overall health, this includes having an efficient immune system, a healthy mouth and gums (healthy gums are a light pink in colour). Certain deficiencies such as those of vitamin C, also known as scurvy, can result in bleeding gums as the immune system is negatively impacted by the deficiency of vitamin C which is vital in the strengthening and supporting thereof.
Prevention
Periodontitis can be prevented by following a routine of sound oral hygiene that is practised from a young age and continued consistently throughout your life. This routine, which was basically outlined above, should consist of the below:
- Having good dental hygiene – This involves brushing your teeth at least twice a day for as long as two minutes. It is advised that you also floss before brushing to allow for food debris and bacteria to be loosened. Our article on gingivitis explains how to brush your teeth and floss correctly step-by-step.
- Seeing your dentist regularly – Seeing your dentist or oral hygienist every six months to a year will aid in detecting any issues and infections before they develop into gum disease. If your risk factors for infection are higher, then speak to your dentist about making these visits more regular.