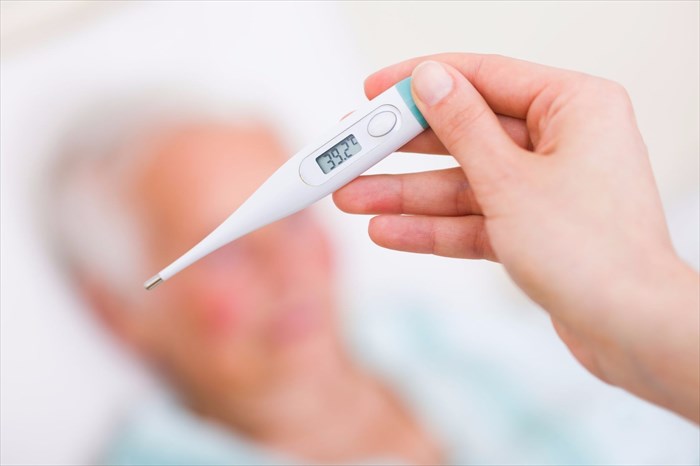
What is hyperthermia (heat-related illness)?
Understanding the basics of body temperature
The body’s ability to regulate heat (i.e. to produce or reduce heat, controlled by the region of the brain known as the hypothalamus) describes how body temperature is determined. Normally, the body is well equipped to maintain temperature within a safe range even when external temperatures fluctuate dramatically. The hypothalamus is effectively the body’s very own thermostat. So, the hypothalamic thermoregulatory centre balances the heat produced by the metabolic processes in the body with heat loss from the skin and lungs.
Heating and cooling functions are regulated in the following ways:
- Excess heat loss: Blood vessels (veins, capillaries and arteries which circulate blood to the body’s tissues and organs) in the skin expand (widen or dilate) in order to carry more heat to the surface of the skin. This can lead to perspiration (sweating), which helps to cool down the body (as sweat evaporates).
- Heat retention in cold exposure: Blood vessels narrow (constrict) and reduce blood flow to the skin. This helps to preserve heat within the body, which reacts by shivering (trembling of muscles helps to produce more heat from within).
Normal body temperature is considered to be an oral measurement of 36 to 37°C (98.6°F), but fluctuates during the course of the day. Body temperature peaks (at its highest) around early evening (6 pm), and reaches its lowest levels around 3 am, then increasing gradually during daytime hours (fluctuations are slight). Fluctuations may also be influenced by other factors such as exercise activity or, for women, the menstrual cycle. Body temperature is quite sensitive to fluctuations in hormone levels and adjusts accordingly.
Body temperature can be measured using a thermometer in various ways:
- By mouth
- The ear
- The armpit
- The rectum
Defining hyperthermia
Hyperthermia, also referred to as heat-related illness, is characterised as a medical condition that is caused by exposure to heat (hot temperatures). Exposure to high temperatures can lead to a range of illnesses which vary from minor ailments to life-threatening conditions.
Exposure to heat results in the ineffective ability of the normal internal temperature control system to regulate itself. Normal cooling mechanisms (sweating or perspiration) start to become less effective beyond an air temperature of around 35°C (95°F). Perspiration evaporates quickly so as to reduce the rate of lost heat. When this becomes ineffective (especially if increasingly inefficient), electrolyte imbalances lead to dehydration, among many other symptoms, and internal body temperature is at risk of rising rapidly. Once body temperature exceeds 40°C (104°F) a person is regarded as hyperthermic.
Hyperthermia versus hypothermia
Hyperthermia effectively means that the body’s internal temperature is rapidly reaching dangerously high levels and is incapable of cooling down through normal functioning mechanisms. Exposure to extreme heat is one of the main reasons why this occurs.
The following are medical conditions which result in hyperthermia:
- Heat stroke:
- Exertional heat stroke (EHS): The most severe form of heat related illness affecting athletes and those who are required to exert themselves in hot conditions such as military personnel, firefighters and manual labourers.
- Non-exertional / classic heat stroke: Risk factors for this include the elderly and bedridden, certain drugs, and individuals who are confined to poorly ventilated rooms in hot conditions.
- Drug induced hyperthermia: This can occur as a result of antidepressant, amphetamine and illicit drug use.
- Malignant hyperthermia which is related to anaesthetic agents.
- Neuroleptic malignant syndrome resulting from the use of anti-psychotic medication.
- Serotonin syndrome as a result of SSRI (selective serotonin reuptake inhibitors) use.
- Endocrine disorders such as hyperthyroidism and phaeochromocytoma (adrenal tumours).
Signs of heat-related illness show very quickly and in mild instances can be effectively controlled. If severe, hyperthermia is a dangerous illness and can result in extreme symptoms leading to brain damage and life-threatening effects on the body’s internal organs.
By contrast, hypothermia refers to a severe loss of internal heat and is deemed a medical emergency. When the body loses warmth quicker that it can produce heat to balance its internal temperature, levels become dangerously low. Loss of body temperature, below the 35°C (95°F) mark places a person at risk for hypothermia, which can lead to a complete failure of the heart and respiratory system.
Exposure to cold (weather or elements such as ice-cold water) may lead to hypothermia. Treatment is required immediately so as to prevent a severely life-threatening situation (severe organ function complications or death).
Hyperthermia versus fever
When there are signs of infection in the body which causes fever and various other symptoms, the hypothalamus reacts by elevating the set point of 'normal' temperature to fever levels as a means to rid the body of infectious agents or toxins. Body temperature rises as part of the immune system’s reaction to ‘unwelcome’ infectious elements such as a virus, bacteria, parasite or fungus, and a person becomes feverish. Once an infection begins to clear, a fever breaks and signals the hypothalamus to ‘reset body temperature’ back to normal.
In the case of hyperthermia, the hypothalamic thermostat remains the same, but changes in the environment which interfere with this thermostat are too excessive for the body’s natural cooling systems. Mechanisms for cooling the body down become overwhelmed by external heat and thus cause a rapid increase in internal temperature.
Medications, particularly those obtained over-the-counter, are effective for providing assistance with breaking a fever, but are not all that helpful when it comes to hyperthermia. In this instance, a change in aggravating factors, such as external environment, rehydration measures and external cooling measures are best for helping the body return to its normal (safe) temperature.
Other Articles of Interest

Frostbite
A serious medical condition, frostbite can lead to severe and irreversible tissue damage. A common freezing injury, we breakdown what happens, what causes it and how best to go about treating it...

Blood Pressure (Hypotension and Hypertension)
Hypotension (low blood pressure) and hypertension (high blood pressure), mean two different things. Find out about blood pressure readings, what they mean, the causes of blood pressure changes & more.
Ultrasound scan
What is an ultrasound scan and how does it work? We look at the numerous ways this screening and monitoring tool is used in medicine today. Learn more about this test here...