When should you see a doctor if you think you have meningitis?
All suspected cases of meningitis should be evaluated and diagnosed by a medical professional (general practitioner or paediatrician) as swiftly as possible.
If you or someone you know experiences combined symptoms of fever, has a very bad / severe headache, nausea and vomiting, a stiff neck and signs of confusion, see a medical doctor as soon as possible.
A bacterial infection, once in the bloodstream, has rapid acting effects and can cause serious complications in a short space of time. Without prompt antibiotic treatment, the condition can result in serious brain damage or even death.
How is meningitis diagnosed?
A doctor will need to assess a full medical health history and perform a physical exam. They will look for common risk factors, as well as assess the nature of your symptoms. Your doctor will check for any signs of infection around your throat, ears, head, as well as the skin along the spine.
Questions your doctor will likely ask you include:
- How long ago did you start experiencing symptoms?
- Would you describe your symptoms as mild or severe?
- Have your symptoms gotten progressively worse (and how quickly has this happened)?
- Do you know of anyone you’ve been in contact with who has been diagnosed with meningitis recently?
- Are you aware of anyone in your household, school or place of work experiencing similar symptoms?
- What vaccinations have you had (full history)?
- Are you currently taking any immunosuppressant medications?
- What other known conditions do you have and are treating?
- Have you experienced allergic reactions to medications?
Meningitis Tests
In order to confirm (diagnose) meningitis, a series of tests will need to be done. These can include:
- Blood cultures: Samples of blood will be taken for testing. Samples are placed in a dish, stained with Gram’s stain and then analysed for the possible presence of microorganisms (bacteria growth).
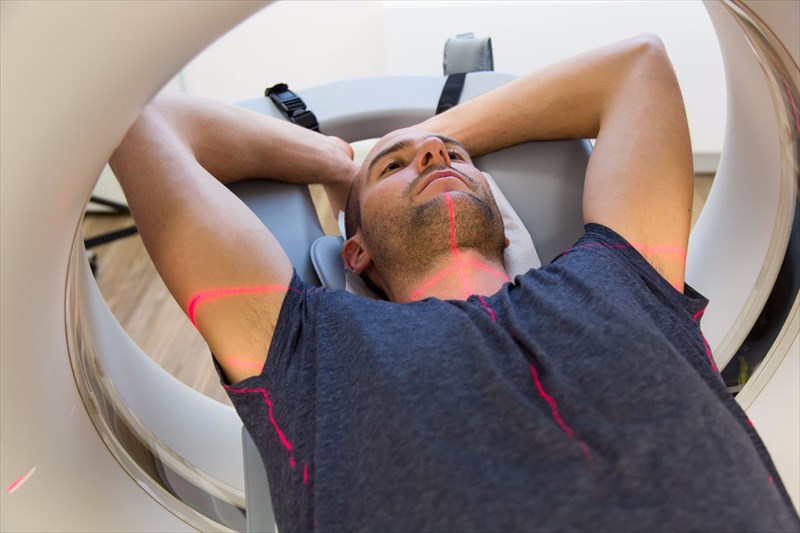
- Imaging tests: CT (computerised tomography) or MRI (magnetic resonance imaging) scans of the head may be recommended to check for any evidence of inflammation or swelling. X-rays of the chest or sinuses can also provide your doctor with a clear indication as to whether these areas are infected.
- Lumbar puncture / spinal tap: Cerebrospinal fluid (CSF) is one of the best and most definitive ways to diagnose meningitis. A spinal tap will be performed to collect CSF and tested to see if glucose (sugar) levels are low and white blood cell counts (white blood cells typically increase when an infection is in the body as a natural way to fight an illness) and protein levels are high. The type of bacteria causing the infection can also be identified. The test is also helpful for assessing the level of increased pressure that may be present in the central nervous system, as well as determining the presence of bacteria in the spinal fluid. A doctor will use his or her findings of this test to prescribe the most effective antibiotic and treatment plan.
- Polymerase chain reaction (PCR) amplification: If viral meningitis is suspected this test may be performed to check for viral DNA. This will help to determine a specific viral cause and as such, the most appropriate course of treatment.
Meningitis treatment
Once your doctor has assessed your medical history, conducted a physical exam and performed various tests, the results of all will be analysed to determine the type (cause) of meningitis diagnosis to be made. Once a type is determined, your doctor can implement the most appropriate treatment plan.
- Viral meningitis: This infection can clear up on its own (usually within 2 weeks), and as such does not require much medical intervention. There is little risk of serious long-term problems. Your doctor may merely send you home to recuperate in bed and suggest plenty of fluids. He or she may also recommend over-the-counter medications to help alleviate any symptoms of fever and body aches. Corticosteroids can also be recommended to alleviate swelling in the brain. If a patient is experiencing seizures, an anticonvulsant medication may be prescribed. If a herpes simplex virus is determined as a cause of a meningitis infection, antiviral medications will be recommended.
- Bacterial meningitis: Your doctor will immediately admit you for hospitalisation. A patient will need to be treated with intravenous antibiotics (sometimes a combination), and corticosteroids as swiftly as possible to prevent further health complications. The antibiotic will depend on the type of bacteria identified as the cause. If a specific bacterial cause is not determined through initial testing, a doctor may prescribe a broad-spectrum antibiotic until such time as he or she can determine the type causing the infection. Any bacteria infected sinuses or mastoids (the bones on the outer ear) may also be drained.
- Fungal and chronic meningitis: A patient with fungal meningitis will be treated with antifungal agents. The exact cause of chronic infections will need to be determined in order to determine the best course of treatment.
- Other: Allergic reactions (to medications etc) or autoimmune diseases can lead to non-infectious meningitis. These cases are generally treated with corticosteroids. In some cases, no medicinal treatment may be required. Any cancer-related meningitis infections will be treated with therapies specific to individual cancer types. In some instances, the underlying meningitis cause is unclear. In this instance a doctor will prescribe antiviral and antibiotic treatment while conducting various tests.

