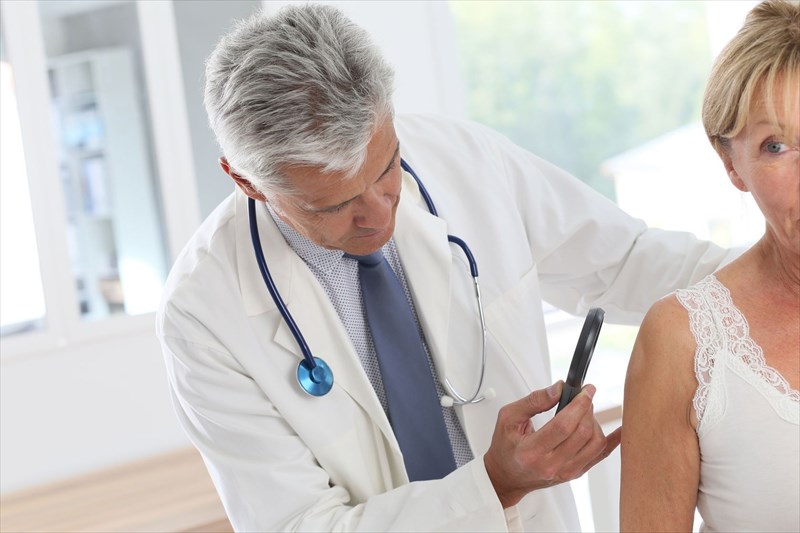
How is vitiligo diagnosed?
A doctor (dermatologist) will generally diagnose vitiligo following a thorough physical examination to assess all the relevant clinical factors of the condition. Along with physical assessments of the skin, a doctor will note a patient’s medical history. This is important for assessing relevant symptoms, as well as to potentially determine any other underlying health related problems.
In order to acquire a comprehensive medical review, a doctor may ask several relevant questions, some of which may include:
- How long ago were patches noticed on the skin?
- Did any patches develop following some form of injury to the skin, such as a skin rash or sunburn?
- Does any itching occur in the affected area/s?
- Are you normally quite sun-sensitive (i.e. do you burn easily)?
- Is there a known family member with a similar skin condition?
- Is there a known family member with a diagnosed thyroid problem or autoimmune condition?
- Have you noted any greying hair before the age of 35?
- Have patches similar to those currently being experienced ever developed before?
- Are you currently taking any medication or supplements?
- What is your occupation and are you ever exposed to chemicals?
- Is the development of these patches making you self-conscious or potentially having any effect on your quality of life?
A physical examination is conducted using a microscopic hand-held device. A wood lamp may also be used if a patient has particularly fair skin, shining ultraviolet light on the skin’s surface in order to evaluate whether or not there is a complete loss of epidermal pigmentation (i.e. no melanocytes present in the affected area of skin / signs of destroyed melanocytes). To use the lamp, an examination may be done in complete darkness. A patient’s skin will be thoroughly cleansed (wiped, not washed) of any grease, make-up or ointments while the lamp is warmed for examination. A doctor will hold the lamp over a patient’s skin (about 10 to 12 centimetres away). A lack of melanin in the affected skin is unable to block / absorb light (which is the normal function of melanin). The lamp will shine a blue white light, displaying vitiligo patches with sharp margins.
To further visualise melanin or pigment loss a doctor may make use of Fontana-Masson staining, a type of silver staining agent (silver nitrate) which is applied to assess a reaction. Melanin cells (melanocytes) take up the silver, reducing it to a metallic state that is visible to the naked eye, without the need for a reducing agent. This staining technique may confirm the absence of melanin.
Immunohistochemistry testing may also be suggested to assess a potential lack of melanin (melanocytes), or a reduced number of cells / residual melanocytes preserved in depigmented skin,) in the affected areas.
A doctor will consider the location of the patches (commonly affected areas include the face, neck, scalp, forearms, hands, fingers, toes and legs). He or she will also look for periocular (surrounding the eyes) or perioral (surrounding the mouth) distribution of markings on the facial area (this is a common distribution pattern when depigmentation affects the face). The distribution of macules may also be more generalised or widespread, affecting the areola and nipples, genital area, or in portions that are easily subjected to traumatic contact, such as the elbows and knees (this is known as Koebner phenomenon – patches develop at the sites of burns, cuts and abrasions to the skin).
A doctor will assess:
- The colour of the markings (macules), which are normally milk-white or chalky.
- The shape of the markings – round, oval or linear.
- The margins or borders – which are normally well demarcated and convex.
- Whether or not the margins are consistent with a total loss of pigmentation associated with vitiligo, and if there are borders which are raised and red (normally associated with marginal inflammatory vitiligo and may be accompanied by some itching).
- Potential changes which appear degenerative in keratinocytes (the epidermal cell which produces keratin) and melanocytes, as well as the skin surrounding the markings.
- Possible epidermal vacuolisation (i.e. the formation of membrane-enclosed sacs which are filled with fluid within the basal cell-basement membrane zone area or tissue that separates the lining of the external body from the internal underlying connective tissue).
- The thickening of the basal cell-basement membrane.
- Whether excess numbers of Langerhans cells (antigen immune cells / dendritic cells of the skin’s surface – these normally help to protect the body from harmful microbes) are present.
- Body hair within the markings to determine whether it has become depigmented (leukotrichia / ‘whiteness of the hair’) – this may indicate a poor prognosis for potential re-pigmentation treatment.
- The possibility of trichrome vitiligo (this will involve an assessment of the areas affected by depigmentation, as well as the area in between affected and unaffected skin where three shades of colour may be evident). Quadrichrome vitiligo can also occur whereby a fourth (normally dark brown) colour develops on the markings (this is knowns as perifollicular re-pigmentation).
During the physical evaluation process, a doctor will likely determine the clinical classification of a patient’s condition – segmented (not normally associated with any other autoimmune disorders or thyroid abnormalities) or non-segmented (typically accompanied by diagnostic markers of inflammatory or autoimmune conditions), also considering the various sub-types of distribution patterns – such as generalised, localised, unilateral etc. Classification is important to determine as this will have an impact on the diagnosis, and recommended treatment procedures.
If a doctor feels the need for laboratory assistance in differentiating types of vitiligo, or there are signs of other inflammatory or autoimmune disorders, further relevant testing may be suggested. He/she may on occasion, suggest a biopsy (skin tissue sample for laboratory testing) in order to make a definitive diagnosis, and potentially rule out any other hypo-pigment or de-pigment types of disorders. It is, however, rare for a skin biopsy to be necessary for a diagnosis of vitiligo.
If an underlying medical condition, such as diabetes, alopecia areata, Addison’s disease, thyroid disorders or pernicious anaemia, appropriate testing will be recommended in order to either rule out or diagnose. This typically involves a blood test (a small sample is drawn from a vein in the arm). A doctor may request a thyroid panel (assessing thyroid-stimulating hormone (TSH), T3 / triiodothyronine and T4 free thyroxine) of hormone levels, or an assessment of antinuclear antibodies, a CBC (complete blood count), measurement of blood sugar and vitamin B-12 levels, as well as anti-thyroid peroxidase antibodies.
In some instances where an autoimmune disorder is determined as a potential underlying condition, a doctor may refer a patient to an appropriate specialist. A counsellor or psychologist may also be considered for referral if a patient’s vitiligo appears to be troubling them emotionally / psychologically.
