
How is vitiligo treated?
There are a variety of different treatment options available for vitiligo once it has been diagnosed. Treatments can help to restore pigment in the affected areas (through re-pigment techniques), but not all work equally well for everyone. Currently there is no single treatment option for vitiligo that can achieve predictably good results for all. Results or responses to the therapies available appear to vary from one person to the next. Certain portions of the body also respond differently to treatment than other areas affected by vitiligo. Pleasing results, are however, possible.
In a patient with particularly fair skin and mild vitiligo macules, a doctor may not suggest much medical intervention at all. Instead, a conscientious effort to protect the skin from sun exposure may be highly recommended. This protects the affected skin patches from exposure damage and also ensure that the surrounding skin does not darken, making patches more obvious.
Many of the treatments available also carry displeasing side-effects, so it is important for the patient to understand the nature of everything available before deciding on a recommended course of action. Results achieved cannot be guaranteed to last for the remainder of a patient’s lifetime or prevent the formation of new patches.
Treatment options can be classified as either non-surgical or surgical.
Non-surgical options for re-pigmentation include:
1. Topical corticosteroids / topical calcineurin inhibitors
These ointments may be prescribed individually or for use in combination. Normally a first-line treatment for localised and segmental vitiligo, topical corticosteroids are a convenient treatment method for many patients and can achieve moderate results. This is also true for those who have an inflammatory element to their condition.
Topical corticosteroids can be applied on a daily basis for several months before being tapered. A doctor will monitor the patient using topical steroids and assess the response to the ointment, as well as to prevent damage resulting in steroid atrophy of the skin (thinning of the skin).
Calcineurin inhibitors are sometimes most effective for vitiligo which involves the head and the neck. Topical tacrolimus ointment and pimecrolimus cream are common recommendations which can also be used in combination with steroid creams. Sometimes topical calcineurin inhibitors can achieve better results when used along with NB-UVB laser therapy.
2. Phototherapy
This treatment, which most often uses narrowband UV-B (NB-UVB) aims to restore pigment in those with early onset or localised vitiligo. It is also recommended as a first-line treatment for those with disseminated areas of pigment in multiple sites across the body that affects less than 10% of the total body surface area and those with stable, nonsegmental vitiligo. Sessions may be recommended in courses (2 to 3 times a week) over a period of at least 6 months and generally between 9 and 12 months in order to achieve some satisfactory re-pigmentation of the affected skin.
Sessions may initially cause the surrounding skin to darken (tan), which makes the depigmented patches more noticeable. A patient who is particularly sensitive to the appearance of their patches should be made aware of this before treatment commences.
Phototherapy treatment is deemed safe for use in paediatric patients (children), as well as pregnant or breastfeeding women. Some side-effects may include skin burning, itching (pruritus) and dryness (xerosis).
NB-UVB has become the more widely used phototherapy technique due to shorter treatment sessions, the lack of nausea following treatment and little need for photoprotection following a session. The overall response to this therapy has also proved better than previous techniques (some of which are still in use, like PUVA / psoralen and ultraviolet A therapy).
3. Laser therapy
If vitiligo patches are limited and appear stable, this treatment option can be effective. Laser therapy may involve an excimer laser which produces monochromatic rays for the treatment of limited or stable vitiligo patches.
Treatment is typically well-tolerated by patients and is deemed safe for most. It is however, a treatment which comes at a bit of a cost. A patient may require 2 treatments a week, totalling between 24 and 48 sessions (depending on the nature of vitiligo patches).
Laser therapy for segmental vitiligo may be combined with topical products (tacrolimus or short-term corticosteroids). Earlier stages of vitiligo may respond better to laser treatment and achieve more desirable re-pigmentation results.
4. Micropigmentation
Micropigmentation, sometimes referred to as ‘permanent cosmetics’ involves medical tattooing in order to re-pigment the affected skin areas. A non-allergic iron oxide pigment is used to cover the depigmented skin by implanting minute particles (or granules) of colour beneath the skin (in a process similar to normal tattooing). the aim is to blend the contrasting skin tones, re-pigmenting the affected skin as closely as possible to the normal surrounding skin. The effect can also soften the texture of vitiligo patches.
While colour matching can be challenging, when done by an experienced professional, the result can be aesthetically dramatic, especially for darker skinned individuals, with a difference in skin colour being immediately noticeable. The process may cause a degree of discomfort which can be eased through the use of topical anaesthetics and some swelling occurs after each session.
Colouration typically fades somewhat within the first six weeks following treatment after which the final result is evident and further fading is minimal.
On average, between 2 and 4 sessions of up to 2 hours each are required to achieve the desired result and these can be done in a doctor’s consultation office. On occasion follow-up treatments may be required.
The side-effects of micropigmentation are typically mild and few. Some risks which will be discussed prior to a treatment schedule taking place include problems with re-pigmentation, inflammation, infection, the possibility of developing an allergic reaction or the formation of keloids (raised scars).
5. Depigmentation therapy
This option may be suggested for patients with vitiligo that is extensive or has been resistant to other re-pigmentation measures. A patient with obvious disfigurement (involving more than 50% of the body, particularly the face and other cosmetically sensitive areas) due to extensive patches can consider this option, but very carefully.
Depigmentation therapy is a permanent solution which permanently removes skin pigmentation from the normally pigmented areas of the skin, effectively “bleaching” it so that vitiligo patches are less noticeable. This is achieved using Monobenzyl ether of hydroquinone (MBEH), which is FDA approved in the USA. Other agents which may be used include 4-methoxy phenol and 88% phenol, imatinib mesylate, imiquimod and diphencyprone. There are other experimental agents being researched as well.
A patient must factor in that depigmentation takes time and may require numerous treatments over many months, as well as periodic touch-up sessions. Thus, this treatment option is also a costly one.
Depigmentation therapy comes with various considerations and side-effects that should be discussed and understood by the patient before commencing treatment. These include:
- Committing to strict sun protection measures for life in order to maintain the results, and prevent the development of skin cancer.
- The potential for the development of adverse reactions to treatment (which are mostly mild) include burning sensations, itching, blistering, dry skin, scaling and swelling.
- The possibility of developing an allergic reaction (contact allergic dermatitis).
- The emotional, cultural and/or social implications that the treatment may have on the individual (A doctor may recommend a consultation with a mental healthcare professional during the decision-making process).
This treatment will not likely be considered for women who are pregnant or breastfeeding. A doctor isn’t likely to consider this treatment for paediatric patients under the age of 12 either. Although a patient with extensive vitiligo may be considered a candidate, for safety purposes, many doctors may suggest depigmentation as a limited therapy option, targeting only the areas of the body a patient feels most sensitive about, like the facial area or limbs (including the hands and feet).
Surgical treatment involves re-pigmentation techniques
Surgical options are normally considered for segmental and localised vitiligo that affects small portions of the body. A doctor will also assess a potential candidate according to whether their vitiligo patches are in areas of the body that are usually resistant to non-surgical re-pigmentation treatments, such as the forehead or hairline, ankles or dorsal fingers.
Patches must also be stable in order for surgical means, which can be time-consuming, to be most beneficial. A patch must not be actively progressing. To determine this, it must be identified that no growth has occurred for a least 2 years (or that no more than 10% worsening has occurred within a 6-month period), melanocytes are not actively being destroyed, and there is no evidence of Koebnerisation (macules / lesions which develops following skin injury healing).
The primary aim of surgical treatment is to achieve a cosmetic result. The methods used will therefore be carefully discussed in order to determine which may best achieve this result. A doctor will carefully assess, not only the nature of vitiligo patches and their location on the body, but also a patient’s age and a potential keloidal tendency.
Surgical techniques generally involve one of two grafting options: (5)
- Tissue grafting: This method involves transferring whole skin tissue grafts to the recipient’s skin.
- Cellular grafting: This technique involves separating grafted tissues into cellular components.
The technique used will depend on the characteristics of the lesion being treated, its location, the age of the patient, their social needs and expectations as well as the expertise of the surgeon.
Tissue grafting methods
1. Split thickness grafts / thin dermo-epidermal grafts / ultra-thin skin grafting
Vitiligo that is stable but not terribly responsive to non-surgical treatment means may be considered for this grafting procedure. The depigmented epidermis is removed using superficial dermabrasion techniques. The thin dermo-epidermal sheets, which include the papillary dermis (the uppermost layer of the dermis) and dermatome (a cutaneous area of skin that is supplied by a single spinal nerve root) are then grafted onto the affected skin.
Cosmetic risks include wrinkling or curling of the graft (which may have a beaded appearance as a result), graft displacement, mismatched pigmentation, perigraft halo (depigmentation around the outside of the lesion), milia formation (a keratin-filled cyst beneath the skin’s surface) and scarring.
To reduce the risk of complications, the ultra-thin grafts must be uniform in thickness and free of any dermal tissue (i.e. almost translucent). Results of this type of grafting, when successful, are normally quite satisfactory when it comes to colour matching.
2. Punch mini-grafting / miniature punch grafting
Of all the tissue grafting procedures, this technique is fairly simple and the least expensive to perform. Punched out skin tissue (circular pieces of skin tissue) are taken from selected normal skin areas, and placed into similar shaped pits in the vitiligo patch. These small punched tissue samples and pits are mere millimetres in size and spaced between 5 and 10 millimetres apart on the skin being treated. Treated areas are held in place with pressure dressings while the punch grafts heal.
Re-pigmentation may be assessed around 4 to 6 weeks following the procedure. Although simple and the least expensive, adverse effect rates are often highest with this grafting procedure and include a cobblestone appearance (or polka dot appearance), perigraft halo (a rim of depigmentation surrounding the lesion), rejection of the graft, graft depigmentation, keloidal scarring, or mismatched pigment. Risks for these effects, as well as the potential for newly formed vitiligo patches, must be carefully discussed beforehand.
3. Suction epidermal grafting
For this procedure a vacuum suction is used to harvest thin skin grafts. A patient may undergo suction, freezing or dermabrasion treatment at least 24 hours before the actual grafting treatment procedure. The skin graft causes a split at the dermo-epidermal junction (the portion of tissue that joins together the epidermal / outer skin layers and the dermal / deeper skin layers). The suction technique creates blisters, from which the tops (beneath the roof of the blister) are used for epidermal grafting.
These thin grafts, which retain melanocytes, can then be applied to skin affected by vitiligo with minimal scarring risks and close aesthetic matching of the normal skin tone.
Some risk factors for this procedure that are likely to be discussed beforehand include wrinkling or graft displacement, a rejection of a graft, scarring, Koebnerisation (the development of new skin lesions in uninvolved areas after injury or trauma to the skin) or a perigraft depigmentation halo (a depigmentation rim displays along the outer edge of the treated vitiligo patch). A doctor may recommend phototherapy to assist with more effective re-pigmentation results.
Cellular grafting methods
1. Non-culture epidermal suspension grafting (NCES)
This surgical technique is also known a melanocyte keratinocyte transplant procedure (MKTP) or cellular grafting and is aimed at replenishing some of the pigment that is lost due to vitiligo.
Cells from normal pigmented skin (usually from the buttocks, thighs or abdomen) are surgically removed and processed to produce a suspension of thousands of cells (i.e. these skin grafts are broken down further into cellular components and multiplied in culture media). These are then placed on the vitiligo patches being treated.
During the process blistering is induced by freezing the skin with liquid nitrogen (although other techniques like suctioning may also be used) and occurs at the source of the donor cells instead of being induced by cutting, which is a fairly unique aspect of the procedure as this typically leaves pigmentation that slowly fades over time.
A doctor will assess a patient as a candidate for NCES / MKTP should their patches be stable. The best results have been noted in those with segmental vitiligo (patches on one side of the body). Areas where the best results can be achieved include the facial area (cheeks and forehead) and the neck, as well as the chest, abdomen, and limbs. Areas that are more difficult to treat include the nose, mouth / lip areas, fingers, toes, knees, ankles, wrists and elbows and results may not be as satisfactory in these areas.
In the best-case scenario a patient is able to see a minimum of 50% improvement in re-pigmentation of the skin area that is treated. No doctor will guarantee perfect pigmentation as one of the risks of this procedure is that no pigmentation will be seen following it. Colour matching is also not assured and may be lighter than the patient’s normal skin tone, or even darker, and can also be blotchy.
Phototherapy may be suggested one week after the procedure (when dressings are removed) as a way to help enhance results.
2. Cultured epidermis with melanocytes / cultured melanocyte suspensions
A patient is typically placed under local anaesthetic prior to this procedure. The removal of skin tissue containing melanocytes is then performed with the use of liquid nitrogen, thermosurgery, superficial dermabrasion or carbon dioxide lasers. A doctor will discuss removal or harvesting methods with a patient beforehand, as well as success rates of each. Areas a doctor may suggest for the harvesting of grafts include the scalp or buttocks.
Removed skin tissue is then incubated with trypsin (a serine protease). Thin sheets of the cultured skin tissue are then grafted, or the suspensions are spread (transplanted) on the affected skin surface.
Large areas of affected skin can be treated during a single procedure and can make use of larger volumes of donor tissues than the non-cultured technique. Results may be evaluated at 3 months and again at 6 months following treatment. Phototherapy may also be suggested during this time to enhance these.
Taking a non-invasive approach
The decision to take a non-medical treatment approach also depends on the nature of vitiligo patches. Those with patches that are more extensive may wish to consider cosmetic re-pigmentation or even depigmentation in certain cases. Those with small patches that aren’t particularly bothersome, and appear to be stable (also depending on their location on the body) may opt for more conservative care.
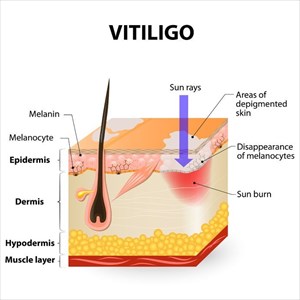
Protecting the skin from the sun is highly recommended, whether opting for medical treatment or not. Vitiligo patches are particularly sensitive to sunlight exposure and can burn easily, further damaging the skin. Applying a good sunscreen (with an SPF of at least 30 or higher) daily to skin that is exposed to sunlight and re-applying as needed is one of the best things a person with vitiligo can do.
Aside from protecting the skin against sunburn, an added benefit includes helping the skin to maintain an overall even tone (tanning of the skin can further enhance the contrast between depigmented and normal skin complexion). It is also advisable not to make use of tanning beds or sun lamps as tanning alternatives. Skin affected by vitiligo can still experience damage and burn during these processes.
Another conservative option for mild vitiligo is to make use of skin camouflage. Coloured cosmetic creams and make-up products are widely available in a variety of different tones to match a person’s natural skin colour (as closely as possible). Applied correctly, many products are manufactured to last between 12 and 18 hours, or more. Many products are waterproof as well, which helps with longer wear.
Before using any camouflage creams or make-up products, or even self-tanning lotions (those that contain dihydroxyacetone are FDA-approved), it is wise to consult a medical doctor (dermatologist) for advice on the best products to use, and those to avoid. No matter the intention, caring for the skin in the best possible way, and thereby preventing any further damage, is important.
Although micropigmentation is a technique used in the treatment of vitiligo, it is not advisable to try and conceal vitiligo patches with conventional tattoo processes. This can further damage skin and may also stimulate the formation of new patches (activating the Koebner phenomenon within weeks of getting a tattoo).
The emotional impact of vitiligo (6)

In instances where vitiligo is extensive, those with the condition can easily fall into emotional distress and anxiety over feeling stigmatised. If not addressed, this can result in the development of depression. This has a major impact on a person’s quality of life. It’s a tricky condition to have due to its chronic nature, and lack of predictability in terms of progression and the ability of uniform treatment measures offering effective long-term results. This in itself may be somewhat demoralising, having a significant and profound impact on a person’s self-confidence levels. Those that feel particularly self-conscious struggle with feeling unattractive, which extends into their ability to have healthy and happy relationships with others. Fear, shame, adjustment disorders and even suicide have all been linked with the emotional and psychological distress experienced by vitiligo patients.
Added to a person’s own personal discontent with patches on their skin, the vocalised or perceived opinions of others can have a psychological and emotional impact too. Many sufferers have been subjected to nasty comments, vocalised insults, antagonism, teasing and sometimes isolation from social circles.
Unfortunately, the history of human nature has a lot to do with adverse perceptions. Ancient texts have shown how individuals with vitiligo were treated in the same manner as lepers, with their condition viewed as ‘white leprosy’. Historically, vitiligo also has strong cultural and religious links, whereby those with the condition were badly treated. For instance, in India, a person with vitiligo was believed to have committed some form of rebellion (‘Guru Droh’) in a past life, and their current skin condition is the punishing result. In countries where religious or cultural perceptions aren’t understanding of the medication condition, the impact can be quite negatively profound. Women may not be considered marriage material and are thus ostracised within their community.
The impact of vitiligo on a person’s self- image, along with any changes achieved through treatment can affect the individual not only physically but psychologically. Those with darker skin complexions may feel the impact even more so, since the contrast in skin tones may be most obvious in them. Many struggle to cope with embarrassment, especially if patches occur on areas of the body that are difficult to cover up (like the face or hands), or cause a fair amount of disfigurement. If these feelings are not properly addressed and persist for considerable amounts of time, they can lead to depressive states and social isolation. Withdrawal from public spaces is often due to an expectation of rejection.
Emotional distress also extends into a person’s working life or schooling, making attendance difficult and interfering with performance in these areas. Children are particularly vulnerable to psychological trauma and self-esteem issues, especially if the attitudes of those around them are negative.
If a person develops difficulty in coming to terms with their skin condition, it is a good idea to seek counselling from a mental health professional. Vitiligo is generally recognised as a medical condition of the skin, but in recent decades has also been regarded as one that can benefit from psychological approaches in order to assist the affected person in developing a positive outlook for their condition, and thus improving self-image. In this way, quality of life can also be improved.
When considering treatment options, a doctor may suggest counselling to a patient with vitiligo that appears to be emotionally distressing, as part of their standard treatment procedure. Counselling is also recommended should a person consider treatment options that could greatly impact their appearance, such as in the case of depigmentation for extensive vitiligo. Like the dramatic changes to the skin caused by vitiligo, changes in reverse can also have an emotional and psychological impact.
Vitiligo may not be a life-threatening condition, but it can have a profound effect on a person, and this is becoming more and more recognised in the medical field.
Is a potential cure for vitiligo still a far-off idea?
While there is no cure for vitiligo at present, current treatment options have shown some success. New discoveries in medicine have led research teams down a path of exploration. For medical professionals and patients alike, this can be viewed with some degree of hope. Much of what is being learnt about vitiligo could potentially result in the breakthrough many are hoping for down the line.
Some avenues research has explored include:
- Pseudocatalase: In 1995, researchers tested PC-KUS (Pseudocatalase), a compound which could be modified as a topical gel for possible re-pigmentation purposes. A total of 33 participants in one study did achieve some success with this topical application, along with short-term NB-UVB light exposure (which is used to activate the compound) and calcium supplementation. Re-pigmentation was noted in the majority of participants between 2 and 4 months after treatment, with complete re-pigmentation of the hands and face in 90% of the group being achieved. No new patches developed in any of the participants during the treatment trial, and no recurrence of vitiligo was found during a follow-up after 2 years. (7) The compound has also been noted to be able to restore original colour for hair that has become grey. Other studies have also used children as participants, achieving some promising success (up to 75% re-pigmentation). (8) Creams with the compound are available for use (and if used should be done so with the consent of a medical doctor).
- Afameanotide: Another synthetic compound, alfameanotide was tested (2014 / 2015) as a means to mimic a-melanocyte-stimulating hormone (alpha-MSH) which is typically low in those with vitiligo. The natural hormone is known to aid in inducing skin tanning. Used in combination with NB-UVB light exposure, some successful re-pigmentation was also achieved when this compound was implanted beneath the skin (stimulating the production of melanocytes). Some side-effects have been noted in trials, the most common being nausea, abdominal pain and hyperpigmentation of normal skin. (9)
- Tofacitinib citrate: One of the latest studies centres around a medication used for the treatment of arthritis – tofacitinib, which inhibits an enzyme called Janus kinase that is also linked to vitiligo as a condition. Researchers are looking at the potential benefits of Janus kinase (JAK) inhibitors for the treatment of vitiligo, among others like eczema and alopecia areata. Thus far studies have been small, but the conclusions promising. In one study, half of the participants (5 out of 10) achieved re-pigmentation at patch sites treated with low-dose NB-UVB light therapy while on the treatment. (10) Comparisons were also made with suction blistering treatment, and it appears that the use of light rather than immunosuppression achieved better results while using JAK inhibitors (oral medications). Further trials are needed with larger study populations in order to draw more conclusive results. Topical JAK inhibitor therapy is another emerging treatment being researched where the topical application of ruxolitinib can achieve about a 23% improvement after 20 weeks. (11) This too requires further research but has shown some promise.
What is the outlook for someone with vitiligo?

Where treatment is successful for one, it may not be for another. That said, treatment options on offer do have a track record of success rates and can be beneficial. Often a doctor may recommend combining two or more treatment options in order to achieve the best possible results.
It is best to begin any treatment with a full understanding of what it will entail and the types of outcomes which can be expected. If vitiligo is emotionally distressing, undergoing counselling can also have a positive impact on the sufferer, often helping to improve their overall quality of life and self-image. Using knowledge of the disease and treatment options, as well as psychological tools, a vitiligo sufferer is better equipped to handle the physical changes that come with treatment for vitiligo.
Vitiligo is not life-threatening or too physically debilitating (a normal active lifestyle is still possible) and can remain untreated should a person feel that treatment options or camouflage are unsuitable or not something they are comfortable with. Thus, the outlook for this skin condition is also largely in the hands of the person concerned. There are options available and once armed with knowledge, and an affected person can make the most informed decision for themselves, as well as seek support from others in counselling groups. Re-pigmentation through treatment is possible but the results are not guaranteed.
References:
5. US National Library of Medicine National Institutes of Health. April - June 2013. Grafting in Vitiligo: How to Get Better Results and How to Avoid Complications: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3764767/ [Accessed 22.11.2017]
6. US National Library of Medicine National Institutes of Health. 23 October 2003. Quality of life in patients with vitiligo: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC269995/ [Accessed 22.11.2017]
7. US National Library of Medicine National Institutes of Health. 1995. Treatment of vitiligo with a topical application of pseudocatalase and calcium in combination with short-term UVB exposure: a case study on 33 patients: https://www.ncbi.nlm.nih.gov/pubmed/7599386 [Accessed 22.01.2018]
8. US National Library of Medicine National Institutes of Health. July 2008. From basic research to the bedside: efficacy of topical treatment with pseudocatalase PC-KUS in 71 children with vitiligo: https://www.ncbi.nlm.nih.gov/pubmed/18613887 [Accessed 22.01.2018]
9. US National Library of Medicine National Institutes of Health. January 2015. Afamelanotide and narrowband UV-B phototherapy for the treatment of vitiligo: a randomized multicenter trial: https://www.ncbi.nlm.nih.gov/pubmed/25230094 [Accessed 22.01.2018]
10. US National Library of Medicine National Institutes of Health. October 2017. Repigmentation in vitiligo using the Janus kinase inhibitor tofacitinib may require concomitant light exposure: https://www.ncbi.nlm.nih.gov/pubmed/28823882 [Accessed 22.01.2018]
11. US National Library of Medicine National Institutes of Health. June 2017. Treatment of vitiligo with the topical Janus kinase inhibitor ruxolitinib: https://www.ncbi.nlm.nih.gov/pubmed/28390737 [Accessed 22.01.2018]
