Preparing for liposuction
Recommendations before surgery
Should a patient be determined as a candidate for liposuction, a surgeon will request the following where relevant:
- Cessation of anticoagulants / blood thinning medications (particularly aspirin) and NSAIDs (non-steroidal anti-inflammatory drugs), as well as (extra) vitamin E supplements (at least 2 weeks before surgery)
- Cessation of alcohol and tobacco product use (at least 3 weeks prior to surgery (4)) or illicit drugs (if applicable)
- Reduction of sodium / salt intake at least a week before surgery - Excess sodium (salt) can result in unnecessary swelling following a major surgical procedure.
Blood thinning medications and NSAIDs can result in complications associated with bleeding (prolonged or excessive bleeding) during the procedure. These medications bind to blood platelets impairing normal coagulation (the process whereby blood changes from liquid to a more gel-like state). Excess vitamin E in the body can interfere with the function of Vitamin K, which can then result in an increased risk of unnecessary bleeding. For this reason, levels which are determined as too high may prompt a doctor to request that supplement us be temporarily ceased just prior to surgery. It may also be recommended that iron supplements, as well as ginger and garlic not to be consumed in the days before surgery as these substances can sometimes interfere with anaesthetic and contribute to a longer recovery period.
Females taking contraceptive pills may be asked to stop taking them in the lead up to surgery. This is to avoid the increased risk of possible deep vein thrombosis which can occur as a result of surgery, birth control pills themselves or a combination of the two.
The intake of substances such as alcohol, tobacco and illicit drugs can result in anaesthetic-related complications (adverse reactions during surgery). These substances can also have adverse effects on the circulatory system putting a patient at higher risk of developing an infection or bleeding excessively.
A surgeon will recommend that a patient stay well hydrated in the days before their scheduled procedure. If a surgeon favours compression garments during recovery, these may be custom-fitted during pre-operative consultations.
Preparation for liposuction on the day of surgery
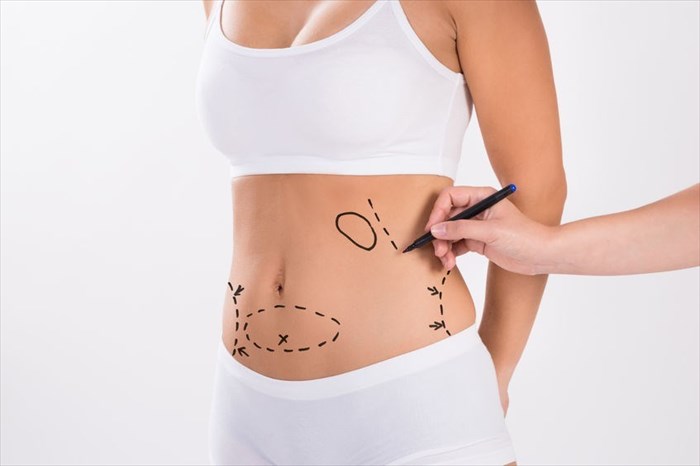
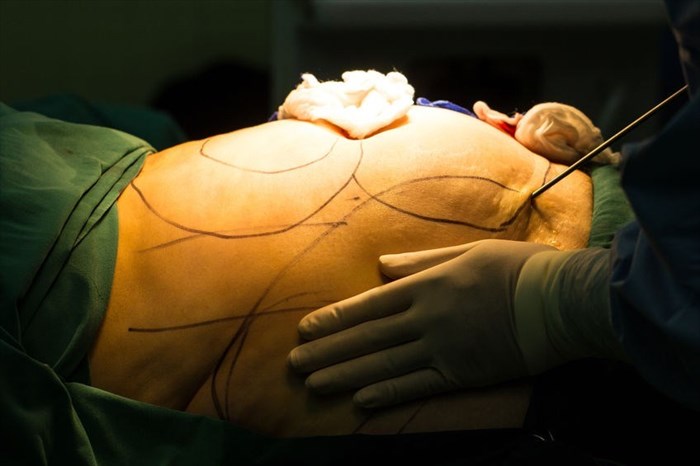
Surgical markings
A surgeon will make use of surgical markers on the day of a liposuction procedure for the purposes of marking the targeted treatment areas. Normally a patient will be asked to stand during the marking process – when lying down marking becomes more difficult as targeted areas become distorted and fatty deposits shift hindering accuracy.
Topographic markings using surgical markers are typically estimations, but the use of digital three-dimensional topographic surgical maps (using 3D photography and analytical software) can provide more precise and accurate markings in the operating theatre. In this instance, images are projected onto a patient before surgical techniques begin.
Topographic-type markings are intended to indicate the location of the fatty deposit (or bulge) at its most central point. Successive concentric circles will then be marked father away – this is to indicate liposuction tapering for the surgeon. A surgeon will also mark off any depression areas, usually in another colour which indicates portions to be avoided during the procedure.
Port sites will also be marked while a patient is standing. It is normal for a surgeon to plan between 2 and 3 port site markings for each targeted body area, allowing for cross-tunnelling removal (aspiration). Multiple sites help to reduce surface irregularities.
Surgical equipment
A surgeon has a selection of cannula tools which can be used for liposuction treatments. He or she will make a selection based on the requirements of a patient, the targeted areas, volume to be removed and tissue types. Some tool designs contain 3 windows / openings which are situated 120 degrees apart and have a blunt tip. Other designs have openings which are downward-facing (these help to prevent the suctioning of superficial fat). Blunt tips are helpful for reducing injury to the surrounding soft tissues.
A surgeon can also make use of cannulas with different shaft lengths, taking into account the target area access required. Shorter lengths (1.5mm, 2.4mm and 3.8mm) are more suitable to the facial and neck areas. Shorter lengths and smaller cannulas offer increased control over fat harvesting, most often with lower risk of contouring abnormalities. Longer lengths (3mm to 6mm) are more suitable for accessing the abdomen, back, hip and thigh areas. When more aggressive fat harvesting is required, a surgeon can make use of other tipped cannulas (known as ‘sabre-toothed cannulas’ or ‘tiger-tip cannulas’). These are useful when working with tougher tissues, sometimes during secondary procedures.
If a surgeon is targeting areas of the body affected by cellulite, ‘loop-de-loop’ or ‘pickle fork’ cannulas are available. These cannula styles can also be used to re-inject fat into the body for contouring purposes, helping to correct and smooth over any irregularities. The ‘Micro-Aire’, a power-assisted cannula with a rotating tip is a reasonably new addition to a surgeon’s ‘toolbox’. Fat harvesting can be performed with less physical strain on the surgeon when using this option.
Body positioning and procedure preparation
A patient will be placed in a supine (or prone) lateral decubitus (SLD) position (lying flat / horizontally with the entire length of his or her body supported by the operating table beneath) during liposuction. This position provides the surgeon with the most comfortable access to the target areas of the body. Minimal position adjustment should multiple areas be targeted during the procedure, is also easier to do when a patient is lying horizontally (either face up or down as is necessary).
A patient’s knees and hips may be flexed and rotated, especially if a surgeon requires easier access to the gluteal and hip areas.
The surgical team will take particular care to prevent pressure injuries during surgery. Sensitive pressure points, such as the face, breasts, elbows, pelvis, knees and heels will be carefully padded. The eyes will be protected with lubricated padding and a patient’s head will be comfortably placed on a headrest.
The anaesthesiologist will also be able to have easier access to a patient’s windpipe or trachea in supine or prone positions, should complications with breathing arise during the procedure and an endotracheal tube be required for treatment.
A surgeon and his or her team will prepare the patient’s entire body circumferentially and lay him or her upon sterile blankets / sheets. Preparation involves a scrub with a povidone-iodine solution (such as Betadine) which functions as a disinfectant. Once the body has been scrubbed, a povidone-iodine paint is applied and the areas to be treated draped with sterile sheets.
If the patient’s hips and legs are flexed or rotated a sterile stockinette and self-adherent tapes or wraps are placed around them, keeping the lower extremities away from the target areas a surgeon will be working with. This helps to keep the lower extremities sterile too.
Antibiotics (normally a first-generation cephalosporin) will be given to a patient at least an hour before the surgical procedure commences to help prevent bacterial infection.
The majority of liposuction procedures require a patient to be under sedation or anaesthetic (regional anaesthesia with conscious sedation, local or general anaesthetic). If toxicity is a concern, a patient will be placed under general anaesthesia and lidocaine will not be used as part of the wetting solution. Spinal anaesthesia (lumbar epidural) is often preferred if a surgeon is working with the lower half of the body. General anaesthesia may then not be necessary. General anaesthetic is generally preferred for large volume procedures or if specifically requested by a patient. Local (or spinal) anaesthesia with careful monitoring is suitable for small volume liposuction procedures.
Large volume procedures for obese patients may be best performed in 2 or 3 sessions to avoid too much body repositioning during the procedure. In this instance, a surgeon will concentrate each session on specific body portions without having to turn a patient over mid-way.
What to expect during a liposuction procedure
Tumescent / super-wet liposuction
As the most regularly used techniques, tumescent or super-wet liposuction involve the following:
A surgeon and his or her team may make use of body warmers and blankets to help maintain a patient’s core body temperature during the surgery. Alternatively, warmed fluid solutions (38°C -40°C /100.4°F - 104°F) can also be used in this regard. Warming is necessary to avoid hypothermia. If a procedure is expected to last for longer than one hour, blood clot formations causing deep vein thrombosis or pulmonary embolism complications may be prevented with the use of pneumatic compression devices (cuffs or compression stockings). These may be placed around the legs, as well as the arms (if the legs are being liposuctioned).
Throughout the procedure, the surgeon and the medical team will continuously monitor a patient’s heart rate and blood pressure. For those having large volume procedures, more invasive monitoring may be required this will involve central venous pressure and arterial blood pressure measurements monitored hourly. The colour and amount of urine collected in an indwelling catheter will also be periodically checked.
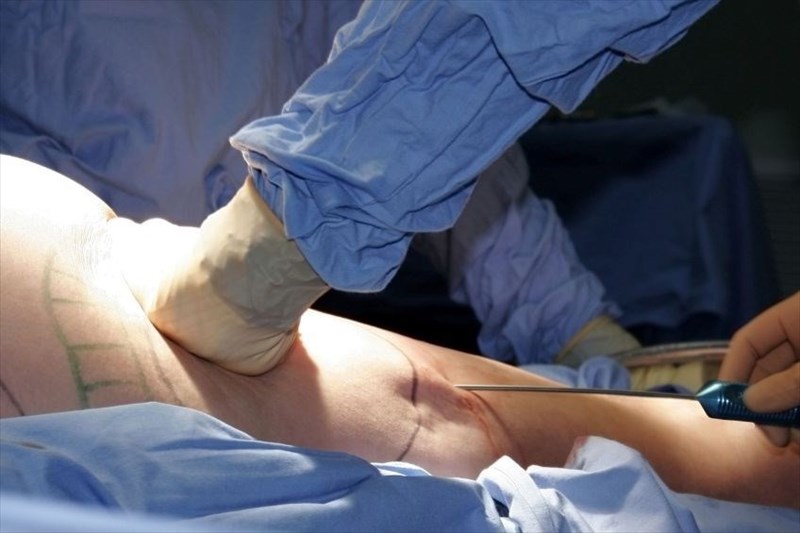
The liposuction procedure will start with small incisions being made in the skin / subcutaneous tissues as needed using a blade, needle or punch. These are then widened (just enough to accommodate the tools being used) in pre-tunnelling preparation. Pre-tunnelling allows for easier cannula control (aiding in technique precision, harvesting accuracy and safety) and aids in preventing the harvesting of the subdermal fat layer, which can then result in contouring abnormalities instead of the desired result.
A haemostat (or haemostatic clamp) is used to compress blood vessels and reduce or prevent blood flow. A blunt catheter is then inserted, allowing for the anaesthetic to be delivered to the deepest fatty layer first using an electric-powered peristaltic pump, followed by the more superficial layers. A spinal needle can also be used for certain targeted areas if it proves easier to administer. Pre-suctioning fluid solutions are then injected.
The surgeon will then insert the cannulae into the deep fatty layer (the various lengths and styles used will be pre-decided depending on the body portions being treated) – normally at two separate axes – at perpendicular (right) angles. This is done to aid in achieving a smoother result and to prevent sharp, irregular contour effects at the surgical site. The cannulae are attached to aspiration machines (or syringes) which are then activated to vacuum the harvested substances. To administer the fluid required for this type of liposuction, a surgeon may use handpiece (in his or her dominant hand) or foot pedals for ease of control. Fluids are administered until the surgeon can see uniform skin distention and firmness at the targeted site. Within 10 minutes the patient’s skin will begin to blanche (pale) as a result of vasoconstriction (the constriction of blood vessels). During fluid administration some fluid spurting from the incision / port sites may occur.
The surgical team will monitor fluid administration carefully so as to avoid any residual overload which can remain in extravascular compartments. Residual fluids can be slowly absorbed into intravascular compartments and thus result in complications, such as pulmonary oedema (fluid on the lungs), fat embolism or acute respiratory distress syndrome (ARDS) which can be life-threatening.
A surgeon will begin treating the deep layers of the target areas first, followed by the superficial ones. The deep to superficial layer sequence will be done in parallel tracks. As a surgeon sees fit during the procedure cannula sizes can be decreased and the intensity of suction altered. Care will be taken to maintain the cannula tips at a downward angle in order to prevent unwanted suction of the superficial fat layer while working with the deeper layers.

A blunt cannula without suction can be manoeuvred in a lateral pattern so as to loosen any adjacent tissues to the target area. This helps to soften the edges between treated and non-treated tissues, preventing contour irregularities.
Soft tissues are also rolled with a roller or rolled laparotomy sponge so as to remove tumescent fluids. This helps to reduce post-operative drainage at the incision / port sites. Should a patient lose a considerable amount of fluid (including blood) during the procedure, fluid replacement will be administered intravenously. It is rarely necessary, but a patient may require a blood transfusion due to excessive blood loss.
The removed aspirate can be sent for pathologic examination shortly after the procedure should a surgeon wish to determine or rule out any abnormalities, like carcinoma (cancerous cells).
A surgeon may choose to suture / stitch up the insertion (port) site immediately using absorbable stitches. Others may choose to leave smaller incisions open so as to allow for postoperative wetting solution drainage which can result in less inflammation or bruising. Larger incisions made (where larger cannulae are used) may be loosely stitched, allowing for drainage. Drainage tends to taper off over the two days following surgery. Instead of stitches, absorbable (ABD) dressings can be placed to minimise soiling.
Once the procedure is complete, a surgeon will fit compression garments (already made to fit the patient – including binders, girdles wraps or compression hoses) and absorptive gauze pads and sterile dressings to the surgical sites before a patient is taken to recovery. Compression garments can help a patient to feel more comfortable in the days and weeks following the procedure while recovering, helping to reduce swelling and bruising. Compression foam (known as TopiFoam) can also be used beneath the garment (this will be left in place for between 3 and 5 days), as well as abdominal binders (around the abdomen and hips) if necessary. A surgeon may prefer using girdles on the thighs.
Some surgeons may request that compression garments be worn continuously for 2 weeks. Others will request that garments be worn for 23 hours each day for up to 4 weeks. After the initial 2 weeks following surgery, compression garment sizes may need to be adjusted as swelling decreases and any open access wounds in the process of healing will be stitched.
Liposuction is an outpatient procedure which only requires several hours of hospital admission. Following the procedure, and once discharged from the hospital, a patient can return home for recovery.
Ultrasound-assisted liposuction (UAL)
If ultrasound technology is to be used, a surgeon will make use of a coupling gel to prevent any air interferences while using the probe (transducer) before applying the ultrasonic energy.
During this technique, fluid infusions are administered into the subcutaneous fat layers, followed by ultrasonic energy to liquify / emulsify fat cells. Administration of the ultrasonic energy may be done before suctioning or a surgeon can apply it directly to the cannula enabling simultaneous emulsification and suctioning. Administration (using circular strokes) occurs in continuous or pulsed cycles. Continuous cycles cause more destruction of targeted tissues than the pulsed action.
For most parts of the body, ultrasound application is used for no more than 10 to 15 minutes. Once the ultrasound application is complete, a surgeon will proceed with the standard tumescent liposuction technique to remove the fatty deposits.
A surgeon may prefer this technique for the back, upper flank, male breast or chest – as these are areas where super wet or tumescent techniques may not have previously achieved the desired results. Scarring with this technique is minimal.
What to expect after liposuction
A patient may be able to return to mild activity (e.g. walking) within a few days to a week. A surgeon will encourage some mild activity instead of complete bed rest as this helps to encourage better drainage, alleviates slowed blood flow in the extremities (preventing blood clot formation and deep vein thrombosis) and promotes the resorption of fluids. Short, easy walking may be encouraged from day one (i.e. the day of surgery) and gradually increased thereafter.
A patient must avoid strenuous activity for at least 2 to 3 weeks following this type of surgery. Within several weeks, a patient should be able to fully return to normal activity. A working adult can return to work, normally after a week, but this will depend on the amount of liposuction done and an individual’s overall physical condition.
If a patient has had a large volume liposuction procedure (i.e. more than 5 litres of removed aspirate) or has had additional cosmetic surgery, he or she may be subject to a longer hospital stay for observation (usually overnight).
Once discharged from hospital, caregivers will be instructed on the appropriate care procedures with regards to drainage and compression garments. Showering or bathing may be permitted 1 to 3 days after the procedure and compression garments will need to be replaced. Garments must be worn as per the surgeon’s care instructions for up to 6 weeks following surgery.
A surgeon may recommend massaging the treated areas during the first few weeks of recovery – this is to assist in easing swelling and aids in improving any contour irregularities. It can take between 4 and 6 months for swelling to completely resolve.
A patient is likely to feel lethargic, tired and sore a week after surgery but can generally function normally. It’s also not uncommon for individuals to experience numbness and tingling sensations during the first week Those who have large volume procedures should not try to return to normal routines before 2 weeks post-op. A patient will be advised to drink plenty of fluids and consume a high-protein diet. Pain, which is managed with prescribed non-steroidal anti-inflammatory drugs (NSAIDs), may be experienced for about 7 days after the procedure.
Drainage experienced over the initial 1 to 2 days may be red-tinged (due to a small amount of blood being present therein). Swelling can be expected to reduce within 3 to 5 days. Bruising that is experienced tends to ease within 7 to 10 days following surgery.
A surgeon will request follow-up consultations after 5 days, then at 2 weeks, and again at 6 weeks post-procedure. Further follow-ups may be requested at 3 months and then at 6 months.
Light-headedness may be experienced in some patients who have had large volume procedures and is commonly experienced when the compression garment is removed for the first time. These patients will be advised to bring along a trusted individual to the first post-op consultation in the event that a patient be unable to safely travel home on their own.
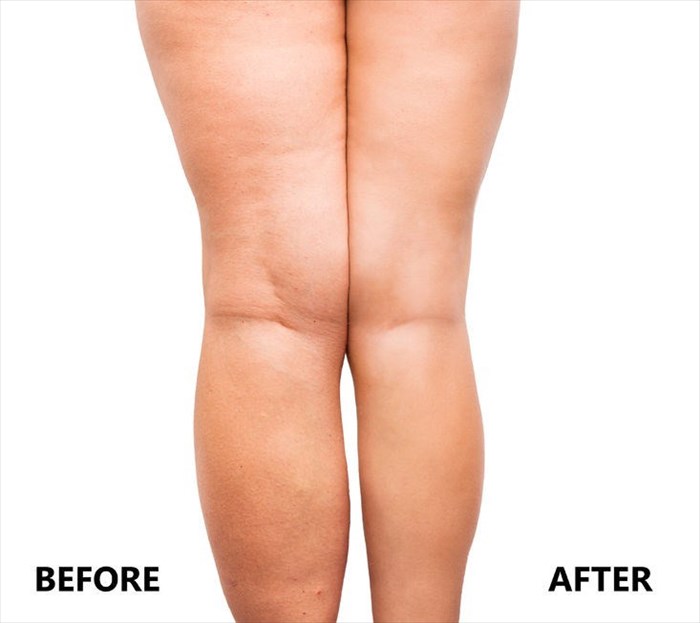
Liposuction Results
Should initial consultations and the candidate selection process have been done thoroughly and in an ethically correct manner, the majority of patients should find their liposuction results satisfying. A surgeon should always ensure that a patient understands that ‘perfection’ by their standards may not be realistically attainable. Provided that pre-surgery consultations included this discussion ensuring that a patient understood exactly what aesthetic enhancements could be achieved, a patient should technically not have ‘perfect body’ expectations when it comes to assessing the results. In this way, self-confidence issues can be significantly improved.
Weight gain following liposuction is not uncommon and is seen in nearly half of all patients who have had the procedure. The area of the body most prone to weight gain is the abdomen. While the procedure effectively and permanently removes fat cells that are unevenly distributed, the fat cells that remain in the body can still expand, storing fat and thus causing weight gain. Liposuction is thus aimed at balancing out weight (fat) distribution and cannot be used as a weight loss tool.
Although weight can be gained, overall shape does tend to more balanced with only a small percentage of liposuction candidates potentially requiring touch-ups at a later stage (several months following the initial procedure).
A surgeon will always encourage a patient to maintain a healthy exercise routine and nutritious diet so as to best maintain the new body shape achieved with liposuction and prevent the need for future touch ups.
Reference:
4. US National Library of Medicine - National Institutes of Health. May - August 2013. Unfavourable outcomes of liposuction and their management: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3901919/ [Accessed 17.04.2018]