How is COPD diagnosed?
Diagnosis is made through a combination of assessed symptoms and a physical examination, as well as a few tests.
Your doctor may ask the following during your consultation:
- Are you a chronic smoker or have you smoked for a period of time in the past?
- Do you frequently inhale second-hand smoke - either at home or in the workplace?
- Are you generally exposed to chemicals and fumes in your place of work?
- Has anyone in your family been diagnosed or treated for chronic bronchitis, emphysema or COPD?
- Do you frequently suffer respiratory conditions, such as viral or bacterial infections?
- Are you asthmatic?
- Are you currently taking any over-the-counter or prescription medications and supplements?
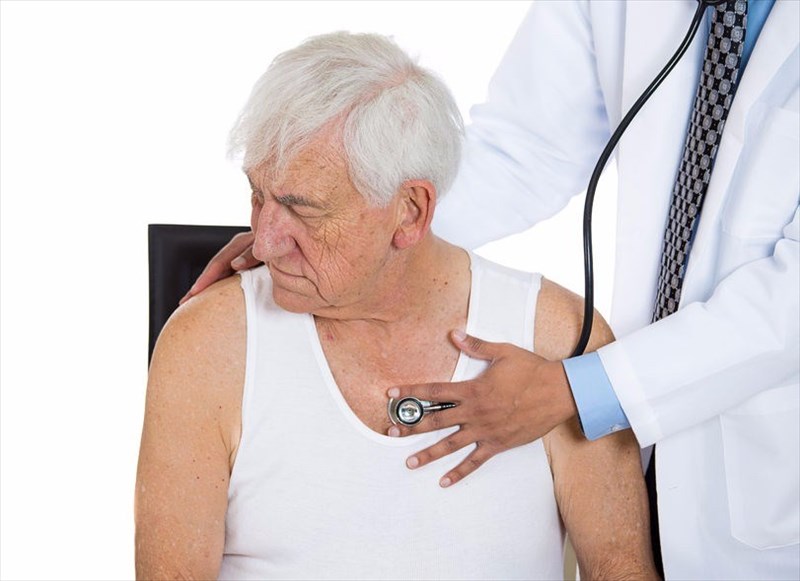
Your doctor will use a stethoscope during your physical examination in order to listen to your lungs as you inhale and exhale. He or she will be looking for any abnormalities or sounds which may point to impaired lung function.
Tests for COPD
Should your doctor feel there is any reason to check your lung function following a short discussion about your symptoms, medical history and physical exam, he or she may recommend the following tests:
- Spirometry: This non-invasive pulmonary (lung) function test is commonly used to determine the nature of a person’s lung function. Your doctor will use a spirometer and tube which he or she will ask you to blow into. The test will measure how much air you are capable of inhaling and exhaling (how much air your lungs have the capacity to hold and how quickly you can blow air out of your lungs). The results will help your doctor assess whether or not enough air is reaching your lungs. This test can detect COPD even before you begin showing any progressive symptoms of the condition. Throughout your treatment, your doctor will also use this test to track and monitor your progression and determine whether your treatment plan is working. If necessary your doctor may perform other lung function testing which will assess lung volumes, pulse oximetry and diffusing capacity.
- Imaging tests: These can include a chest X-ray or CT scan which will help your doctor to see in detail the condition of your lungs, heart, and blood vessels. A chest X-ray can clearly show deterioration due to emphysema and also potentially rule out other potential problems such as heart failure. A CT scan can also detect emphysema and rule out other conditions, such as lung cancer. Your doctor may also use CT scan results to determine if surgery is a beneficial treatment option for you.
- An arterial blood gas test: For this test, a blood sample will be taken from an artery in order for blood oxygen levels to be measured. Results will show how much oxygen is present in your blood and how much carbon dioxide is being removed.
Your doctor may wish to see if he or she can determine a cause of your symptoms as a way to rule out any other suspected diagnoses. For this reason, and not necessarily to make a COPD diagnosis, he or she may recommend other laboratory tests. One such test may be recommended to determine whether you have an AAt deficiency if there is evidence that there is a family history of COPD.
If you suspect impaired lung function for any reason, it is best to consult your family physician (general practitioner) as soon as possible. The sooner COPD is diagnosed, the better the treatment plan can be to enhance your quality of life.
COPD treatment and medications
A diagnosis for COPD may come as a huge shock, particularly because it is not a curable condition. Your doctor will encourage you to take the diagnosis seriously and implement their treatment plan effectively. It is important to understand that the damage already caused cannot be undone, but also that further harm can be effectively reduced and symptoms reasonably controlled.
Your treatment plan will likely include regular consults with a pulmonologist (lung specialist), as well as physical and respiratory specialists (therapists), all working together to provide symptom relief, reduce complication risks and slow down disease progression as much as possible.
Your treatment plan will address the following:
Smoking: If this is the predominant cause of your condition, it is vitally important that you quit smoking completely. Continued smoking in any amount will worsen your condition and eventually reduce any ability to breathe at all. For many with this condition, becoming a non-smoker is not such a simple task. Talk to your doctor about possible nicotine replacement products or medications which may ease you out of your smoking habit and help you to cope with relapses. Your doctor will not only discourage your smoking habits, but also recommend that you stay clear of second-hand smoke exposure wherever possible too.
- Medications: Your doctor may recommend several kinds of medications to manage your symptoms. Most will be recommended on a regular basis, and others as and when needed (treating flare-ups). Some medications will cause side effects. It is important to take your medications as recommended and keep you doctor in the loop should you experience any adverse reactions. Included in the mix of medications are bronchodilators (inhalers or nebulisers which relax the muscles around the airways and help relieve symptoms of shortness of breath and coughing), inhaled steroids (inhaled corticosteroid drugs which reduce inflammation of the airways and minimise the risk of flare-ups), combination inhalers (bronchodilators and inhaled steroids), oral steroids (usually prescribed in short courses to prevent worsening symptoms), Phosphodiesterase-4 inhibitors (relaxes the airways and reduces inflammation), Theophylline (alleviates chest tightness and eases shortness of breath) and antibiotics (or antivirals as and when needed for treating respiratory infections).
- Lung therapies: Oxygen therapy (supplemental oxygen through lightweight, portable units with a mask or nasal prongs while doing activities or sleeping) and pulmonary rehabilitation programmes (specialist tailored programs combining education, nutrition plans, exercise training and counselling) may be recommended to enhance your quality of life and enable you to participate in everyday activities a little easier. These therapies can also help to shorten hospital stays.
- Surgery: Where a condition is severe, particularly in cases of serious emphysema, and a person’s symptoms have not been sufficiently managed with medications, options for surgery may be recommended. These can include lung volume reduction surgery (small wedges of deteriorated lung tissue are removed from the upper lungs, allowing healthier tissue to expand), a lung transplant (a major procedure which carries significant risks but can dramatically improve quality of life) and bullectomy (bullae or large air spaces are removed from the lungs to alleviate problems with breathing and improve air flow).
Your doctor may also recommend vaccinations as a way to lower your risk of contracting respiratory infections. A yearly flu vaccine, pneumococcal vaccine and tetanus booster protecting you from pertussis (whooping cough) may be recommended. Vaccines may not totally prevent an infection, but can help to lower the severity risk should you fall ill.

 Smoking:
Smoking: