- Eczema (Atopic Dermatitis)
- What are the symptoms and signs of eczema?
- What are the causes and risk factors for eczema (atopic dermatitis)?
- What are the different types of eczema?
- How is eczema (atopic dermatitis) diagnosed?
- How is eczema (atopic dermatitis) treated?
- Answers to frequently asked questions regarding atopic dermatitis
The most commonly seen skin symptoms and signs of eczema as a general condition include:
- Extremely itchy and dry skin
- Dry, leathery areas that may appear lighter or darker than your normal skin tone, this is known as lichenification
- Thickened or scaling skin
- Blisters that may be crusty and ooze (these usually occur during flare-ups)
- Red skin forming around blisters
- Raw areas of skin that develop from scratching, these can cause bleeding
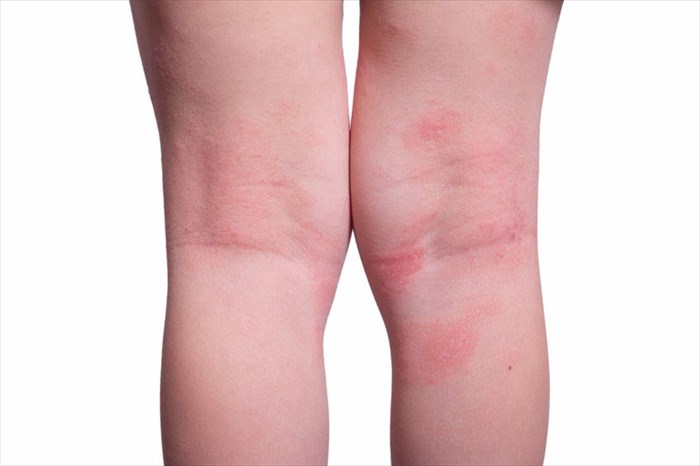
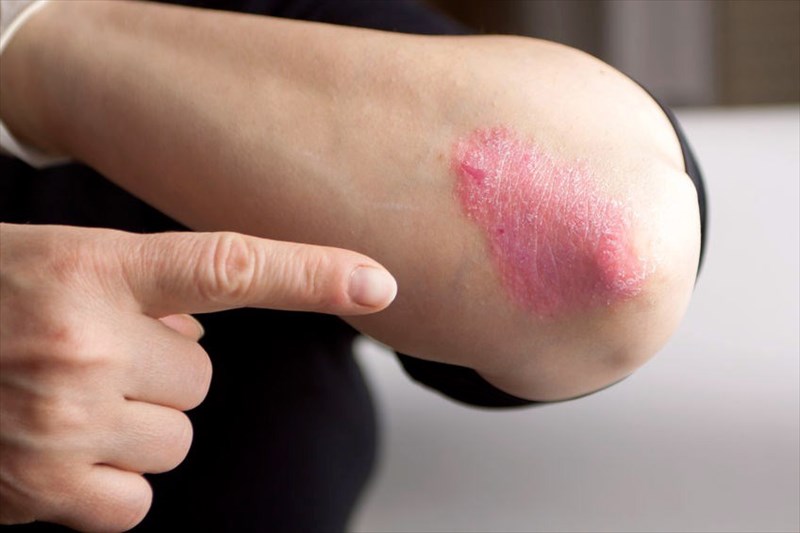
Children who are younger than two years old5 will generally develop a rash on their elbows, cheeks or knees as the initial signs of eczema. Adults with eczema tend to experience it on the insides of the elbows and knees.
What are the symptoms of atopic eczema (dermatitis)?
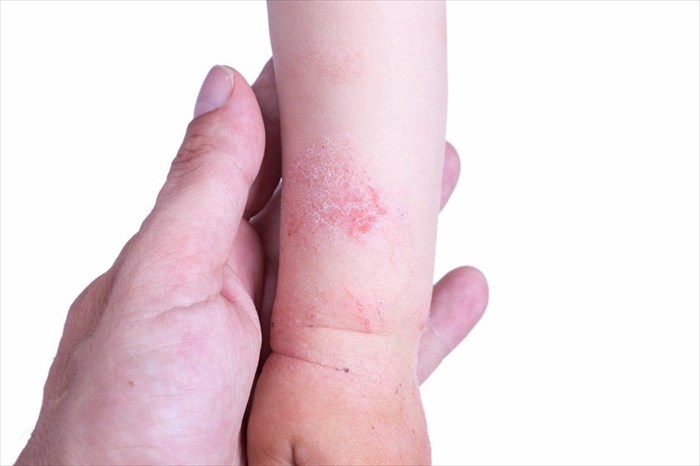
Atopic dermatitis results in patches of the skin becoming red, cracked, itchy and sore. Dry skin is a common complaint among those suffering from this condition.
The skin can also begin to form tiny blisters (this known as vesicle formation) which may crack and weep. This symptom, also referred to as an eruption is termed an eczematous skin reaction, which is characterised by the outbreak of lesions on the skin.
Those affected by eczema are likely to experience periods of symptom improvement or resolution for a time (this is known as remission), followed by flare-ups where the symptoms reappear or worsen. These flare-ups may occur as often as once a week or a few times a month.
Atopic dermatitis can occur in all areas of the body, however, the condition is commonly seen on the hands, with the fingers being affected in particular, as well as the backs of the knees, insides of the elbows and the scalp and face (especially in children).
The presentation of atopic dermatitis tends to vary between individuals with symptoms ranging from mild to severe. Those who have mild eczema will typically only experience smalls patches of dry skin that may be itchy occasionally. People with more severe cases of the condition generally have eczema that is more widespread throughout the body resulting in inflamed and red skin accompanied by constant itching.
The itching and scratching cycle may disrupt one’s sleep and cause the skin to bleed, this may result in secondary infections and the further progression of itching. This can make getting a good night’s sleep and concentrating at school or work difficult.
The areas of the skin affected by an atopic dermatitis rash may also temporarily become lighter or darker in colour after the condition has improved or healed. People who have darker skin will often notice these skin patches more than those with a lighter skin tone. These different coloured patches are not usually a side effect of topical creams or scarring, but are rather a remnant of prior inflammation and will return to normal in time.
Signs of an infection (atopic eczema)
In some cases, the patches of skin affected by atopic dermatitis may become infected. The below describes the signs of an infection in those with atopic dermatitis:
- Eczema begins to worsen with no signs of improvement
- Fluid begins to ooze from the rash
- Yellow crust forms on the skin’s surface or small white or yellow spots begin to appear
- The skin is extremely sore and inflamed
- A fever develops
If the above-mentioned signs of an infection begin to occur with atopic eczema, then it is advised that the affected individual make an appointment to see their doctor.
Can atopic dermatitis affect the face?
Atopic dermatitis can affect the face in a number of areas including eyebrows, lashes, skin around the eyes and the eyelids.
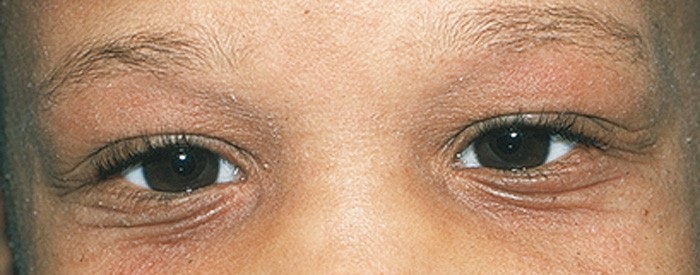
Rubbing and scratching affected areas near the eyes can result in the skin changing in appearance. A few people suffering from atopic dermatitis may develop an extra fold of skin under the eyes, this is known as Dennie-Morgan folds/lines or an atopic pleat. A Dennie-Morgan fold or line occurs due to oedema (swelling) and is often used as a diagnostic marker for allergies, hence the term ‘allergic wrinkles’.
Dennie-morgan lines
Other people may experience hyperpigmented eyelids, this refers to the skin on the eyelids darkening as a result of hay fever or inflammation. Patchy eyelashes and eyebrows may also be the result of rubbing or scratching.
The faces of babies with atopic dermatitis are commonly affected. Infants who drool excessively may also experience further skin irritation due to contact with their saliva.
The skin of those with atopic dermatitis will often lose a large amount of moisture from its epidermal layer. Some individuals with the condition lack a certain protein known as filaggrin, this is a vital component in moisture-retention. Lacking this protein is referred to as a defective genetic trait which allows the skin to become extremely dry and is often seen in those suffering from infectious disorders which include:
- Molluscum contagiosum (water warts)
- Staphylococcal and streptococcal bacterial skin infections
- Warts
- Herpes simplex virus
Conditions of the skin that may occur in people with atopic dermatitis include:
- Lichen simplex chronicus (LSC) – This refers the thickening of patches of skin that becomes raised and scaled as a result of frequent and repeated rubbing and scratching of the same area.
- Lichenification – This describes thick, leathery skin that results from constant rubbing and scratching.
- Ichthyosis – Refers to group of rare conditions that result in excessive amounts of dry scales forming on the skin, these skin formations are commonly seen on the shins and lower legs. There are several different types of ichthyosis, each one is characterised by differentiating scaling and dryness.
- Papules – Papules are tiny raised bumps that can open from scratching and become infected and crusty.
- Hyperlinear palms – This refers to an increase in the number and depth of skin creases (lines) found on the palms of hands.
- Keratosis pilaris – These are rough, small bumps that generally form on the thighs, upper arms and face due to keratinisation of the hair follicles within the skin. The condition is sometimes described as chicken skin or gooseflesh and each little bump may have a small hair that is coiled underneath it.
- Cheilitis – This refers to the inflammation of the skin around and on the lips (often referred to as chapped lips).
- Urticaria – Also known as hives the term urticaria refers to raised red bumps that often form after being exposed to an allergen, after a hot bath, exercise or at the beginning of atopic dermatitis flare-ups.
- Dark circles under eyes – These often result from atopy (a genetic tendency to develop allergic conditions such as asthma or hay fever) or allergens.
- Dennie-Morgan fold (Dennie’s sign / atopic pleat) – This is an extra fold of skin forming under the eyes due to oedema (edema) in those with atopic dermatitis.
- Hyperpigmented eyelids – Eyelids that are scaling (red, itchy and flaking) may darken from hay fever or due to inflammation.
- Prurigo nodules (prurigo nodularis / picker’s warts) – These are not really warts but rather thickened skin bumps that are intensely itchy. Constant scratching of the skin results in hyperpigmented or spot like lesions that are scaly and may become crusted.
References:
5. University of Maryland Medical Centre. 2015. Eczema. Available: http://www.umm.edu/health/medical/altmed/condition/eczema [Accessed 06.10.2017]