What are hives (urticaria)?
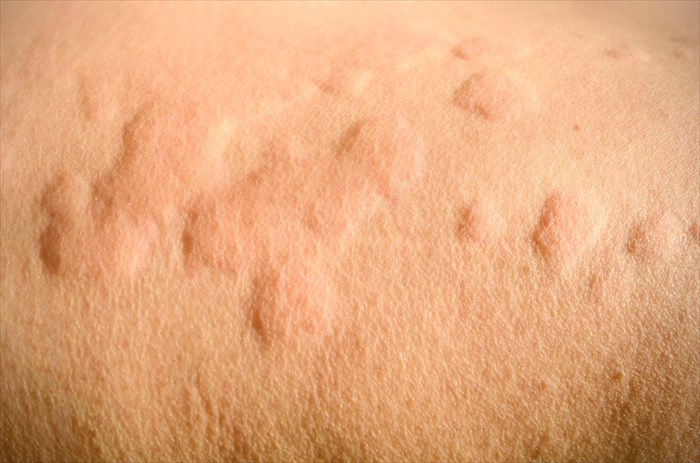
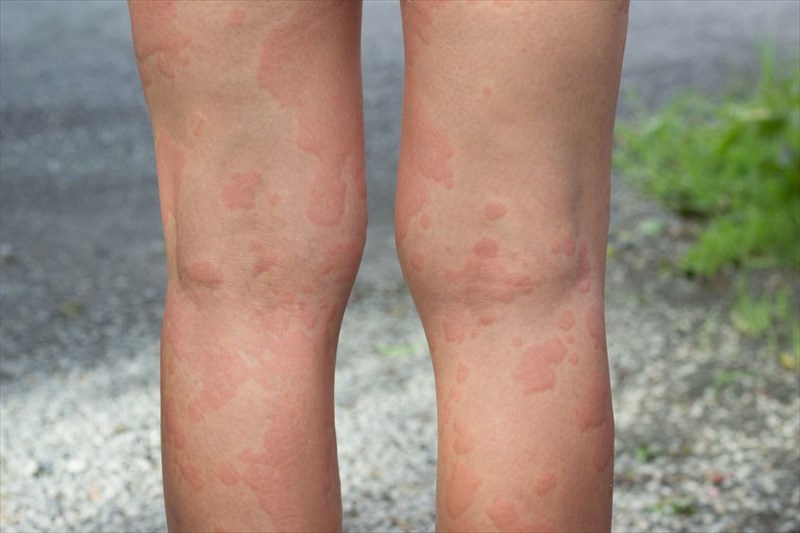
Also known as urticaria (pronounced as ur-ti-kar-ee-uh), hives are characterised as clusters of swollen, raised welts(1) on the surface of the skin which are pink, red or flesh-coloured and blanched (pale) in the centre.
Often these bumps (cysts, wheals or nettle rash) are itchy, and can be painful, causing a burning or stinging sensation. Physical sensations range from mild to severe. Hives can appear suddenly, sometimes for no distinctive reason, and vary in size (small spots to larger markings or blotches) and shape. A bout of hives can occur in anyone of any age and at any stage.
Hives are mostly classified as an acute condition (i.e. temporary) and are most often triggered by an allergen (foodstuff, medication or environmental irritant). Hives can, however, occur on a frequent basis and become a chronic condition. Chronic hives are generally accompanied by severe allergic reactions which can have serious complications. They are thus not considered a contagious condition.
Hives can occur anywhere on the body and can sometimes join together to form larger inflamed welts, known as a plaque. Hives typically flare-up quickly and can remain for several hours to a day (24 hours) or so at a time before fading. Hives do appear to have a tendency to rapidly change in size once a flare-up occurs, and ‘move around’ (i.e. they can disappear from one location of the body, and flare-up in other portions of the body, sometimes in a matter of hours).
Hives are one of the few skin conditions which occur and then appear to resolve in such a short space of time. This can make for difficult diagnosis if the condition is severe enough that medical treatment is sought. It is advisable to photograph the markings while they are at their worst in order for a doctor to analyse if necessary.
References
1. US National Library of Medicine. December 2011. Chronic urticaria. Available: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3276885/. [Accessed 20.08.2018]
Other Articles of Interest

Allergies
Allergies are something many people battle with but do not understand, this article explores all you need to know about allergies and how to deal with them...

Strep Throat (Streptococcal Pharyngitis)
Throat a little sore? If it’s not a viral infection such as the common cold or flu, it could be strep throat. Learn more about this bacterial infection here...
Urinary Tract Infection (UTI)
What are urinary tract infections (UTIs)? We take a look at the most prominent causes, types, diagnostic procedures and effective treatment measures to help clear an infection. Learn more here...