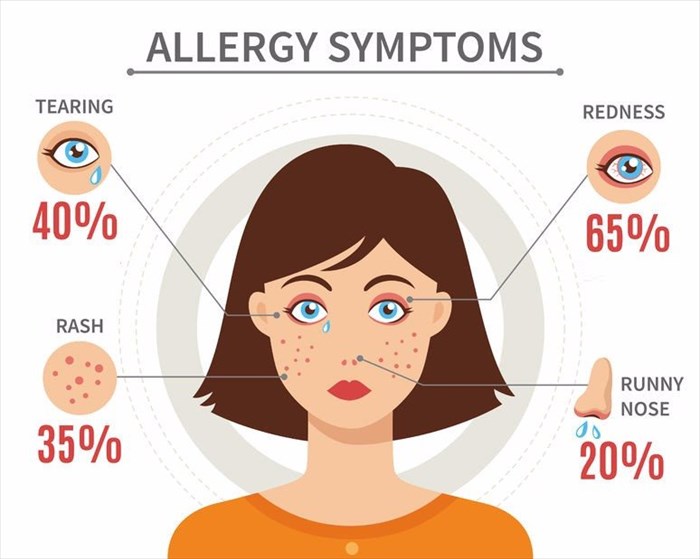
What are allergies?
Allergies are the immune system’s response to allergens. Allergens are substances that are typically harmless to most, but can trigger an allergic reaction in some. Allergies are a common occurrence and can be categorised into groups such as food, drug (medication), substance (latex), seasonal (caused by pollen, grass or mould), insect (bees, wasps, hornets, fire ants) or animal or pet allergies (usually caused by pet dander).
To understand allergies, one must first understand how the immune system functions. The immune system is the body’s primary defence mechanism against invading foreign substances (also known as antigens). When threatened, it creates antibodies (immunoglobulins) to fight off any invading viruses, bacteria, fungi or parasites (i.e. antigens) that have the potential to cause infection or disease. Usually, antibodies identify antigens as harmful invaders and bind to them, rendering them inactive so that they can be destroyed and removed from the body.
When it comes to allergens, the immune system will usually adjust to its environment. For example, when most people come into contact with a cat, the immune system will note the change of environment and detect that any pet dander present is harmless. In allergy sufferers, however, the body mistakenly perceives an allergen such as pet dander (dead skin cells present on a dog or cat’s coat) as an ‘invader’ and treats it as a pathogen (a disease-causing agent such as a virus or bacteria) that is trying to attack or weaken the body.
This elicits an abnormal overreaction of the immune system which results in the overproduction of a chemical known as histamine. When this happens, histamine causes inflammation and the constriction of smooth muscle within the body and an allergic reaction with accompanying symptoms is the result.
Depending on the type of allergy and the manner in which the allergen is encountered, some people may experience tingling, itching, sneezing or wheezing, swelling, breaking out in a rash or inflammation of the throat, nasal passages or digestive system. A number of other possible symptoms including headaches, nausea, diarrhoea, and difficulty breathing may also develop. Inflammation is, however, the primary symptom when it comes to allergies.
The severity of allergies varies from one person to the next and can range from minor irritation to severe, resulting in anaphylaxis. Anaphylaxis is a life-threatening condition and should be treated as an emergency wherein the patient requires immediate medical attention.
The majority of allergies cannot be cured. There are, however, a number of treatments to help relieve the symptoms of allergies.
As you can probably tell, allergies have a lot more to them than meets the eye. The information in the menu at the top of this article provides an in-depth look into what causes allergies, the associated complications and risk factors, symptoms, treatment and more.
Other Articles of Interest
Asthma
An asthma attack can be a terrifying experience for anyone suffering the condition. An inflammatory disease, asthma is not curable, and typically changes over time. Learn more about the condition...
Hives (Urticaria)
Hives are characterised as clusters of swollen, raised welts on the surface of the skin. What causes them? Are there different types? And how should you go about treating them? Learn more here...
Lumps, Bumps and Swellings
Lumps, bumps and swelling is more common than you might think, but when should you worry? Find out more here ...