Once at the doctor’s office, a full medical review and symptom discussion will help to begin pinpointing a possible infection, as well as the extent of illness. A doctor will ask a series of questions that aims to help identify and or / rule out a specific medical problem.
Questions can include:
- How have symptoms been experienced – are they continuous or occasional?
- How would you describe the nature of symptoms being experienced – mild, moderate or severe?
- Do you regularly take over-the-counter pain-relieving medications, like ibuprofen or aspirin?
- Are you aware of a family member with similar symptoms or who may have a history of digestive problems?
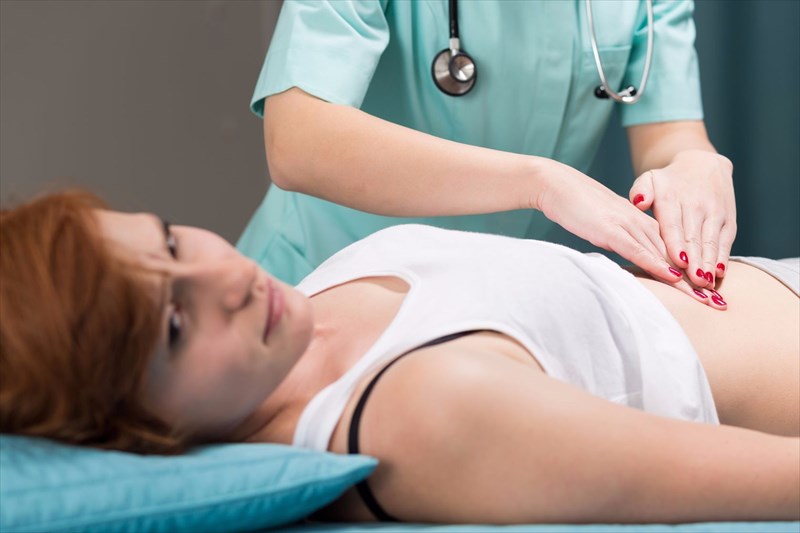
A doctor will then conduct a physical examination to assess one’s overall condition and further identify specific discomforts associated with symptoms being experienced. A doctor will be looking for signs of abdominal bloating, pain or tenderness in the stomach area during palpation (gently feeling various areas of the abdomen). He or she will also listen to the stomach and check for any sounds indicating possible discomfort.
With these noted physical signs, he or she will recommend tests in order to determine an H. pylori infection:
- Blood test: A sample of blood will be drawn from a vein in the arm and sent for analysis at a laboratory. An analysis can reveal a current or previous bacterium infection and can give a doctor a good indication as to whether further testing is required.
- Urea breath test: A doctor will provide a liquid to drink, or a pill to swallow, which contains tagged carbon molecules (urea – a chemical consisting of nitrogen and a minimally radioactive carbon). Bacterium (H. pylori) in the body will trigger the release of the carbon once the substance has broken down in the stomach. The bacterium produces urease, an enzyme, which breaks down urea into carbon dioxide and ammonia. The body naturally absorbs the carbon, but also expels it when exhaling. Around 10 to 20 minutes after the liquid or pill has been administered, a doctor will request that the patient exhales into a device that can pick up and identify carbon molecules. For this test, it is important to know which medications are active in the system as certain acid-suppressing medications (proton pump inhibitors / PPIs), antibiotics or bismuth subsalicylate drugs can interfere with the accuracy of this particular test, as well as that of a stool test too (see below). Medication use could also indicate a cause of symptoms as many pain-relievers are known to cause stomach lining damage with extensive use. For these reasons, before performing this test, a doctor will have noted any medications that the patient has recently taken (including those in the past week or two prior to the consultation).
- Stool antigen test: A sample of stool (faeces which can be collected in a supplied container at home and brought back) will be sent for laboratory analysis to look for antigens (foreign proteins) that indicate an infection with H. pylori bacterium. If it is determined that interfering medications have been taken, a doctor may wish to wait a week or two for the drugs to work out of the system before performing either the stool or breath test. Both of these tests are otherwise fairly accurate for diagnostic purposes. Both breath and stool tests are also effective for determining the eradication of the bacterium following a period of treatment (i.e. checking that bacteria are no longer active in the body).
- Scope screening: An upper gastrointestinal (GI) endoscopy (also known as a Gastroscopy) procedure may be recommended. This test gives a doctor ‘eyes inside’ the gastrointestinal tract. To perform the screening, a patient will be booked into a hospital environment and sedated (under anaesthetic). A doctor will then thread a long, thin and flexible tube with a tiny camera attachment at the end (endoscope) down the throat and oesophagus all the way into the stomach and duodenum (small intestine). This type of screening allows the doctor to view the inside of the digestive system (on a computer monitor or screen) without the need to make any cuts (incisions) into the body. Any abnormalities (signs of an infection) within the upper digestive tract can be detected. If any are identified, tissue samples can be extracted at the same time using appropriate tools attached to the scope in order to send for laboratory testing (biopsy). The samples can then be analysed for the bacterium (using CLO test slides which contain urea) causing problematic symptoms. A scope screening is more likely to be recommended if there are serious signs and symptoms of infection present, in order to aid in the diagnosis of conditions which have arisen as a result, such as an ulcer. Alternatively, this procedure can also help to rule out other conditions, for instance cancer. The aforementioned tests (blood, stool and breath) are less invasive for a simple identification of Helicobacter pylori bacterium in the system. Alternative visual screenings may include recommendations such as X-rays or a CT (computerised tomography) scan in order to acquire detailed images of the gastrointestinal tract.
