What is lupus?
Lupus is a chronic autoimmune disease1. In autoimmune diseases the body’s immune system mistakes its own tissues for foreign ‘invaders’ and ‘attacks’ them. This causes abnormal inflammation and the destruction of healthy cells.
In those with lupus, the inflammation the autoimmune response causes can affect various tissues and organs in the body including the skin, joints, lungs, brain, heart, kidneys and bloodstream. In some cases, this can lead to complications and permanent damage in one or more areas of the body1.
There are four types of lupus:
- Systemic lupus erythematosus (SLE): This is the most commonly diagnosed form of lupus. It can be mild or severe and affects various areas of the body.
- Discoid lupus: This type of lupus causes a red rash that doesn't resolve (i.e. go away on its own)
- Subacute cutaneous lupus: In those with this form of lupus, sores develop after exposure to sunlight.
- Drug-induced lupus: As the name implies, this form of lupus is caused by taking certain medicines. It usually resolves when the medication in question is discontinued.
- Neonatal lupus: This rare form of lupus affects newborns. It is believed that it may be caused by certain antibodies produced by the baby's mother.
Many of the common lupus symptoms mimic those of other ailments and conditions, as such, many sufferers delay seeking medical help. This fact can also make medical diagnosis difficult unless a sufferer exhibits the telltale signs of lupus like a butterfly rash (malar rash). For many people it takes up to six years to be accurately diagnosed from the time they first notice symptoms2.
While the exact cause of lupus is unknown, various genetic, hormonal, and environmental factors, as well as immune abnormalities are thought to play a role in its development.
Who gets lupus?
Some individuals appear to be naturally more prone (born with a tendency) to developing lupus. Typically, lupus affects African, Asian or Native American ethnic groups more frequently than Caucasians3.
While lupus affects both sexes, it is more common in women. In fact, nine out of ten people diagnosed with lupus are women, generally over the age of 403. Lupus can, however, be diagnosed at any age.
Lupus can be severe, and for some, is potentially life-threatening. Some may suffer life-long disabilities due to the disease. Many, however, experience a milder form of it. In all cases, lupus is currently an incurable disease and can only be treated and managed with the help of a medical professional.
References
1. Gergianaki I, Bertsias G. Systemic Lupus Erythematosus in Primary Care: An Update and Practical Messages for the General Practitioner. Front Med (Lausanne). 2018;5. doi:10.3389/fmed.2018.00161
2. Lupus facts and statistics. Lupus Foundation of America. https://www.lupus.org/resources/lupus-facts-and-statistics. Accessed December 17, 2018.
3. Pons-Estel G, Alarcón G, Scofield L, Reinlib L, Cooper G. Understanding the Epidemiology and Progression of Systemic Lupus Erythematosus. Semin Arthritis Rheum. 2010;39(4):257-268. doi:10.1016/j.semarthrit.2008.10.007
Other Articles of Interest
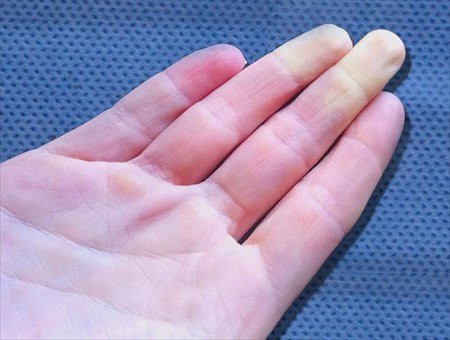
Raynaud Phenomenon / Syndrome / Disease
Why are your hands and feet always so cold? It could be poor circulation, or it may be a condition known as Raynaud phenomenon / syndrome / disease. Here's everything you need to know...

Anxiety
Anxiety is a psychological, physiological, and behavioural state that may cause a sufferer intense distress. An anxiety disorder can be disabling, but it is manageable. Learn more about it here...

Anaemia
Did you know that there are over 400 variations of anaemia? We define the condition, it's causes, symptoms and how to go about effectively treating it.
