
How is PCOS diagnosed?
To diagnose polycystic ovarian syndrome (PCOS), a doctor will take you through the following steps:
- Medical history: A doctor will ask specific questions relating to a woman's overall symptoms (What are you experiencing? How long ago did you notice your symptoms? How often are you experiencing your symptoms? How severe are your symptoms?) to gather as much specific information as possible. He or she will discuss areas such as weight (Have you gained weight? How much have you gained?), the condition of hair and skin, as well as the nature of menstrual cycles (When was your last period? How frequent are your periods? Do you bleed heavily?). He or she may also ask if a woman is currently trying to get pregnant and experiencing any trouble. A doctor will need to know what medications and supplements are being taken, as well as get a good idea about eating and exercise habits. A woman may be asked to share specific details abouther family medical history (as much as she knows). Specific questions around this may include any known hormonal issues in the family (Has your mother or a sister been diagnosed with PCOS?) or diabetes. It is important to be as honest as possible, even though much of what is being experienced in terms of symptoms is highly personal, which can be very uncomfortable. Honesty will help the doctor to test appropriately and make the most accurate diagnosis in order to treat in the most effective way.
- Physical exam: A doctor will then want to conduct some physical checks to help either diagnose or rule out potential causes. He or she will look at the thyroid gland, the overall condition of your hair and skin (including the chest or breast area and abdomen), as well as assess your BMI (body mass index). Your doctor will check your blood pressure and then request a pelvic exam. This will help the doctor determine if there are any abnormalities with your ovaries (particularly if they are enlarged).
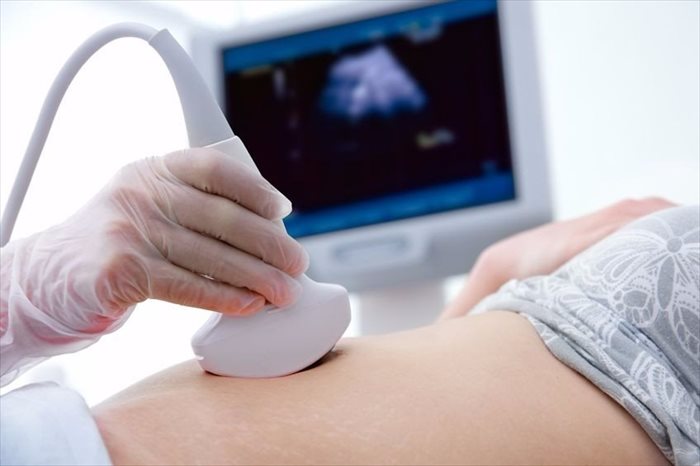
- Ultrasound: A doctor may then request a pelvic ultrasound to look at a visual of your ovaries and determine whether there are any follicles. An ultrasound won’t necessarily confirm PCOS as some women do not have follicles on their ovaries, but have other symptoms related to the disorder. An ultrasound will create real-time images of your reproductive system to assess any areas of concern or help to pick up any abnormalities which will be tell-tale signs of a malfunction in the body. If there are any growths spotted at this stage, a doctor may recommend a pelvic laparoscopy. This is a minimally invasive surgical procedure that allows your doctor to make a very small incision in the lower abdomen area. A tiny camera will then be inserted to get a better view of any potential growths of cysts. If it is determined that there are growths or cysts, more tools will be inserted to retrieve a small tissue sample (biopsy) to send away to the lab for further examination or testing.
Tests involved in diagnosing PCOS
A doctor may recommend several blood tests to examine the following:
- Thyroid function: A blood sample may be used to assess how much thyroid hormones (thyroid-stimulating hormone / TSH) in the body produces and whether there are any signs of an overactive or underactive thyroid.
- Blood sugar levels: A sample of blood will be used for a fasting glucose test to measure sugar levels. A doctor may also wish to check insulin levels and assess glucose tolerance levels to see if there any signs of abnormal function (such as insulin resistance). If there are any signs of possible diabetes as a result of PCOS, this test is more than likely to be recommended.
- Cholesterol levels: A lipid level test will assess the amount of cholesterol and triglycerides in your blood. If there are strong signs that a woman’s blood pressure, cholesterol and triglycerides need to be checked frequently or if she is at higher risk of heart disease, atherosclerosis (hardening of the arteries), heart attack or stroke as a result of PCOS, a doctor may like to perform this test.
- Sex hormone levels – Androgen, oestrogen, progesterone and testosterone.
- Adrenal gland hormone levels: Problems with DHEA-S or 17-hydroxyprogesterone can lead to PCOS-like symptoms.
- Prolactin (PRL) levels: A protein hormone that enables women to produce milk. These levels can also play a role in infertility or disrupted menstrual cycles.
- hCG (Human chorionic gonadotropin): If a woman is sexually active, a doctor may wish to test if she is already pregnant before conducting further tests or prescribing a treatment plan.
PCOS treatment
Once diagnosed, a treatment plan is going to be one of focussed control. At present, there is no cure for PCOS. A doctor will make recommendations that will best manage the symptoms of the condition so as to reduce the risk or prevent possible complications, as well as make a woman as comfortable as possible to live her best life.
Treatment does tend to vary from one person to another, and largely depends on specific symptoms. Recommendations a doctor will make will involve the following:
Lifestyle: Diet and exercise habits will form a large part of the changes that will need to be adapted to for overall health and wellbeing. A healthy eating plan (that includes fruits, vegetables, whole grains and low-fat dairy) that is low-calorie or low in carbohydrates and regular exercise activity is highly recommended, especially those who are overweight. Carbohydrates shouldn’t be completely restricted. A woman may want to seek assistance from a dietician who can recommend carbohydrates which are high in fibre (whole-grain breads, whole-wheat pasta, whole-grain cereals, brown rice, beans, barley and bulgur wheat) as part of the diet plan. In this way food is digested slowly, and gradually stabilises your blood sugar levels. Maintaining this is also essential, in order to control a healthy weight, as well as help stabilise a menstrual cycle and balance out hormone levels. A good rule of thumb when it comes to exercise is to try and get in about 150 minutes’ worth of activity each week. A doctor will recommend that a woman does not smoke as this promotes higher levels of androgen in the system.
- Pregnancy planning / birth control: A doctor will discuss options available when it comes to pregnancy. If a woman is not yet (or not at all) interested in starting a family, a doctor may prescribe oral contraceptive pills (birth control pills). These are known to help regulate a woman’s menstrual cycle, lower male hormone levels in the body and also treat acne. An alternative to birth control pills is the patch or vaginal ring which also contains oestrogen and progestin hormones. Both options are also effective for reducing the likelihood of falling pregnant. If a woman is wanting to get pregnant and have a baby, a doctor may prescribe fertility medications (hormone therapy) to stimulate ovulation, helping the body along. Any hormone medications taken to stimulate ovulation will usually be accompanied by regular ultrasounds and consults with a reproductive specialist to keep a close eye on your progress and reduce the risk of any complications.
- Medications: Treatment in the form of medication will involve those that aid in reducing male sex hormone levels (this is known as anti-androgen medication). This will reduce excess hair growth and acne. If blood glucose and testosterone levels are high, diabetes medications may be prescribed to help stabilise this in the body. If a woman is working to lose weight through good nutrition and exercise, and is struggling to shed the kilos (or pounds), a doctor may prescribe medication to help stimulate ovulation in the meantime. Usually, reducing weight will help stabilise hormone levels and stimulate ovulation. Hormone therapy (which can include birth control pills) can also be effective in correcting menstrual cycle concerns. Oral contraceptives are also good with controlling hormones that can lead to a build-up resulting in uterine (or endometrial) cancer. Pills that contain both oestrogen and progesterone help to regulate menstrual cycles, decrease androgen production and thus correct abnormal bleeding.
- Surgery: One option is ovarian drilling. This procedure may be recommended if a doctor feels it necessary to destroy part of the ovary with a laser or electrocautery (which involves ‘puncturing’ the ovary with a small needle that has an electric current or by using an electrode) as a short-term solution that may help stimulate ovulation and reduce male sex hormone levels. If a woman has been unsuccessful in losing a sufficient amount of weight and has had a poor response to medication, this procedure may be recommended. Another surgical option is an ovarian wedge resection. This procedure effectively removes part of the ovary in an attempt to promote normal ovulation and regulate a woman’s menstrual cycles. As an option, this procedure is rarely recommended as there is a risk of damaging the ovary and causing scar tissue. A doctor will discuss the benefits and risks of all surgical options, and these are generally only recommended if all other treatment options have not been successful. One such risk is scar tissue which can cause pain or fertility concerns later down the line. Some benefits may be temporary and not last the rest of a woman’s lifetime. A woman should ask as many questions as she needs to in order to be well informed about any recommended procedure before consenting to it. The more a woman knows, the better she will be able to understand her body and how to alleviate present symptoms and reduce the risk of future complications.
A doctor will advise regular check-ups so as to monitor the body’s overall condition and reduce the risk of developing further health complications such as high blood pressure, cholesterol and heart disease.

 Lifestyle:
Lifestyle: