Are there ways to prevent PCOS?
An endocrine system disorder, PCOS cannot be prevented. Early diagnosis, effective treatment and lifestyle changes can help to lower a woman’s risk of developing any long-term health complications. This disorder is not yet curable, and is merely managed according to a woman’s symptoms throughout her life.
What can you do to manage excessive / abnormal hair growth?
For a woman, excessive hair growth in areas of her body that aren’t normal can be upsetting and uncomfortable. It can make a woman feel very self-conscious about her appearance and affect her self-confidence.
For a woman with PCOS, the best option in dealing with this symptom is to understand what is happening in her body so that she can better deal with its effects. When androgen hormone levels are high, hair growth in abnormal areas (the chest, stomach, toes and face) occurs. Medications will help to regulate hormones and decrease these levels of androgen.
A woman can still make removing unwanted hair part of her beauty regimen (and choose a method that works for her budget) in the following ways:
- Electrolysis: Permanent hair removal process by means of an electric current that is applied to the hair root.
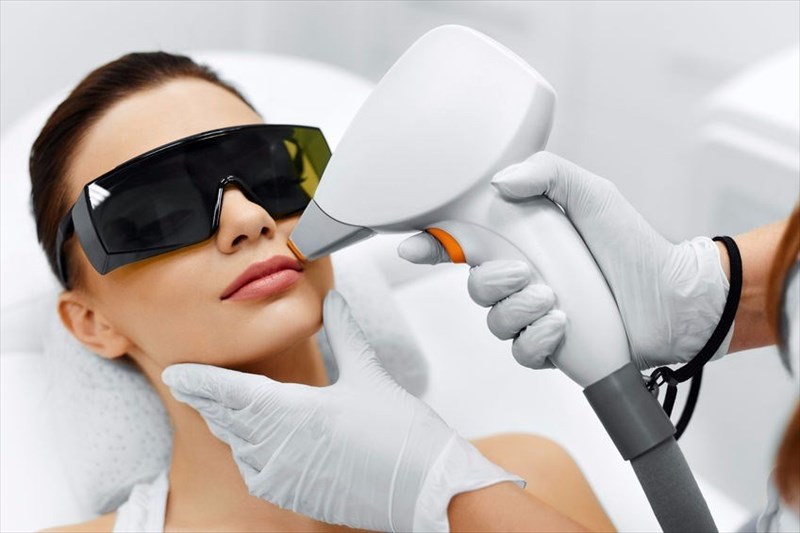
- Laser hair removal: A process using a laser beam which destroys hair follicles.
- Depilatories: A chemical hair removal product is applied to the skin in order to remove unwanted hair.
- Waxing: Semi-permanent hair removal which pulls hair follicles out by the root.
- Bleaching, tweezing and shaving
How will diet changes really affect PCOS symptoms?
One of the biggest changes a woman diagnosed with PCOS will make is an adjustment to her diet. What she puts into her body is of vital importance and has a direct impact on her body and in turn, the nature of her symptoms.
A healthy and nutritious diet will need to be a lifelong commitment. Aside from hair growth, weight gain in excessive amounts can also deeply affect a woman’s self-esteem and make her very self-conscious about her appearance. As well as the physical aspects of this, excessive weight, and even obesity can have a debilitating effect on a woman emotionally.
A woman can kill two birds with one stone (in a sense) by working with a dietician or nutritionist to develop the best diet plan for her overall health, reduce her size (and thereby the increased risk of other health complications) and improve her emotional and mental wellbeing.
The best place to start is to learn about how what one eats affects the body (and by extension the disorder). With abnormalities in hormone levels, insulin levels are higher than normal. This affects the function of cells in the body be able to process glucose (sugar) into energy which sustains a person throughout the day.
Without enough insulin in the body, blood sugar levels increase. A woman may also become insulin resistant as a result of an imbalance and become unable to process the amount the pancreas does produce effectively enough. As a result, the body attempts to regulate itself and maintain blood sugar levels at a normal rate by pumping out higher levels of insulin. Insulin resistance affects a woman’s weight and makes it more difficult for her to lose a sufficient amount.
The result of high insulin levels also directly affect a woman’s ovaries, causing an excess production of male sex hormones (androgens) such as testosterone.
To combat high insulin levels and abnormal or excessive hormone levels a woman with PCOS should look to add the following foodstuffs to her diet on a regular basis:
High-fibre foods such as broccoli, cauliflower, lentils, beans, red leaf lettuce, brussels sprouts, green and red peppers, berries, almonds, squash, pastas or pasta noodles (with lentil or bean flour), pumpkin and sweet potatoes.
- Lean protein such as fish, tofu and chicken.
- Anti-inflammatory foods such as tomatoes, kale, turmeric, spinach, olive oil, almonds, walnuts, blueberries, strawberries, spices and fatty fish, such as sardines and salmon that is high in omega-3 fatty acids.
As with introducing more high-fibre, lean proteins and anti-inflammatory foods, there are others which a woman can be more mindful of limiting or cutting out altogether from her diet. These foods will aggravate insulin resistance and lead to inflammation in the body which will worsen symptoms of PCOS. These foodstuffs include:
- Refined carbohydrates such as white bread, muffins, sugary desserts, pastries, white potatoes, pasta noodles (which contain durum flour, durum wheat flour and semolina) and other foods made with white flour (i.e. cakes etc.)
- Sugary foodstuffs that include sucrose, dextrose and fructose corn syrup, as well as juices (with added sugar) and sodas (Coke, Pepsi, and other carbonated drinks).
- Inflammatory foods such as red meat, processed meats, French fries (chips) and margarine.
A change in diet will definitely be beneficial for a woman with PCOS. Once a woman’s settles into a new eating pattern, her overall health and mood will improve. It’s important to remember that just about every food that will exacerbate a woman’s physical condition and PCOS symptoms, generally has a healthier counterpart. There is no real need to feel that your diet is restricted. You’re just opting for healthier alternatives.
Can women with PCOS have children?
An imbalance in the body and a disrupted menstrual cycle doesn’t necessarily mean that you will not be able to conceive and carry a baby. Hormonal therapies have been effective in inducing a more regular menstrual cycle and thus regulating the system to accommodate the changes that pregnancy brings with it.
How effective therapies are does vary from one woman to the next, and are variable among women with PCOS undergoing assistance with fertility specialists. In some cases, it merely comes down to weight. Some women may be able to achieve improved ovulation patterns with moderate levels of exercise, effectively reducing their weight and maintaining it.
Others require a little help in the form of medication and assisted reproductive technologies (fertility options) to help with conception. Age and other health concerns are a huge factor in the success rate of these kinds of treatments, but if ovulation stimulation is successful a high percentage of woman can conceive.
What should a woman be mindful of when it comes to PCOS and pregnancy?
PCOS is typically diagnosed and treated during a woman’s childbearing years. A woman wanting to have her own children need not feel that her condition will mean the end of her dream of becoming a mother. Women with PCOS can still have healthy pregnancies and babies. A woman will, however, fall into a high-risk pregnancy category and be carefully monitored. This is to ensure the safety of both mother and child as there are risks for certain complications during the 9-month gestation term, labour and delivery of the baby.
It is important that a woman with PCOS understand that her pregnancy will not be without risk of complications. Pregnancy-safe exercise and diet will also play a huge role in having a healthier experience and baby, as well as managing PCOS symptoms. Discuss everything with your doctor to ensure the best possible outcomes.
It may also be a little difficult for a woman to fall pregnant in the first place due to hormonal imbalances. Other physical aspects that may compromise a woman’s ability to fall pregnant relate to her weight. Obese women may need a helping hand with the use of reproductive technology. This can still be challenging and a small percentage have successful pregnancies. If you have been trying to conceive naturally for more than a year and find that you are struggling, speak to your doctor for advice and assistance. Your doctor will be able to give you all the information you need regarding the options available to you and also discuss strategies that may help to increase your chances of conceiving.
Risks and complications for women with PCOS wanting to get pregnant include:
- Insulin resistance
- High cholesterol
- Hypertension (high blood pressure)
- Heart disease
- Type 2 diabetes
- Gestational diabetes
- Stroke
- Sleep apnoea
- Preeclampsia (also known as toxaemia, this is a pregnancy complication characterised by high blood pressure)
- Delivering a larger than normal sized baby (a caesarean / c-section may be necessary to deliver safely), a smaller than normal sized baby, and miscarriage.
- Uterine / endometrial cancer
A baby who is larger than normal in size also runs the risk of injury during delivery and may experience shoulder dystocia (when the shoulder gets stuck during birth). This is why a large baby will usually be delivered via caesarean and not natural birth.
Other risks for the baby include:
- Premature birth
- Meconium aspiration (or neonatal aspiration of meconium – a baby experiences respiratory distress when meconium, which comprises of substances such as amniotic fluid, bile, mucus and water accumulated in the womb, is breathed into the lungs during birth)
- Lower Apgar score (the measure of a new-born baby’s physical condition that details heart rate, muscle tone, respiratory function, response to stimulation and skin colouration).
Another risk relates to female babies who have a higher chance of having PCOS (born from a mother with the disorder) themselves once they reach puberty and start menstrual periods.
Hormonal fluctuations during pregnancy will affect pregnancy and continue once a baby is born and a new mother begins breast-feeding. It may take some time for a woman to feel 'normal' during pregnancy and breast-feeding, and settle into the changes both will bring physically and emotionally.
It is generally safe for a woman with PCOS to successfully breastfeed, but will depend on any medication prescribed to be taken as well. Insulin medication to help control blood sugar levels may not be problematic. Check with your doctor and discuss options that will best benefit you and your baby. Certain medications may be discontinued during pregnancy and breast-feeding, but overall if well monitored, your PCOS symptoms will not necessarily get in the way of a healthy pregnancy and baby.

 High-fibre foods
High-fibre foods