Defining sickle cell disease, its causes and types
What is sickle cell disease?
An autosomal recessive condition, sickle cell disease (SCD), also known as sickle cell anaemia, is characterised by a group of inherited red blood cell (RBCs) disorders. A person with the condition typically has two copies of the autosome gene (non-sex chromosome). Essentially, the normal function of red blood cells in the body is compromised and they aren’t able to carry a sufficient amount of oxygen throughout the body.
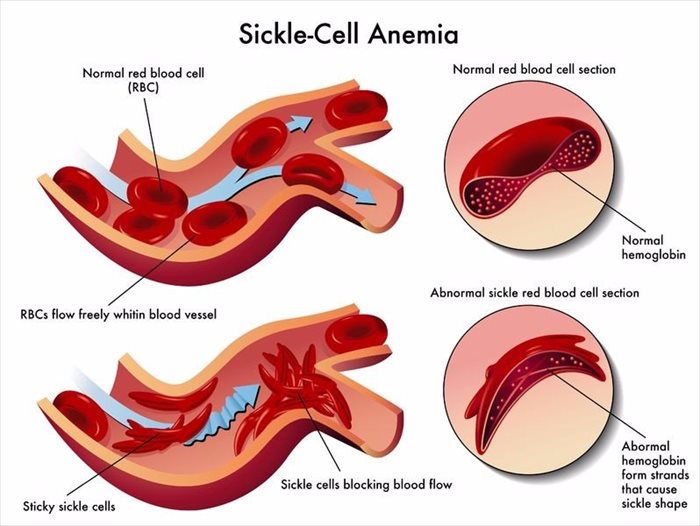
Normally, the body’s red blood cells are round in shape (like little discs) which enables them to travel easily throughout the body. The shape gives them enough movement flexibility to be carried through even the smallest blood vessels in the body.
A person with SCD does not have many round shaped red blood cells. Their RBCs are crescent-shaped, like that of the crescent-shaped blade known as a sickle (almost crescent moon or banana-shaped). This shape is not as flexible for the cells to perform their normal functions and thus makes them ‘sticky’ and more susceptible to becoming ‘trapped’ or ‘stuck’ as they move, particularly in smaller blood vessels. This in turn means that blood and the oxygen they carry is restricted from reaching various parts of the body that require it for normal function. The lack of sufficient blood flow and oxygen then results in tissue damage (organs, bones and muscles) and pain.
A person with SCD is also more susceptible to anaemia, infections and even stroke. As an inherited disease, the condition is managed with a daily treatment plan to alleviate symptoms and prevent as many complications as possible. As yet, there is no cure for sickle cell disease.
Causes of sickle cell disease
As an inherited blood disorder, sickle cell disease is passed from one generation to another (known as ‘autosomal recessive inheritance’). A mother and father must each pass on to their offspring a defective form of the gene (haemoglobin S gene) that normally produces healthy and red, iron-rich compounds (haemoglobin – the protein which carries oxygen in the blood) for SCD to occur.
It can happen that only one biological parent passes on this defective gene to their child. In this instance, a child may be diagnosed as having the sickle cell trait. This means that a child will have one defective form of the gene and one normal haemoglobin gene. This enables the body to produce a healthy supply of haemoglobin (with normal red blood cell function) as well as sickle cell haemoglobin (defective function causing damage to the body).
A person with the sickle cell trait may not have symptoms of pain as result of damage to the body, even though there is a presence of abnormally shaped RBCs. They will, however, be carriers of the disease, which means it is entirely possible to pass on the gene to their offspring.
Types of sickle cell disease
A haemoglobin molecule comprises of 4 polypeptide chains. Two of these are characterised as ‘alpha chains’ (containing 141 amino acid residues each) and the remaining two as ‘beta chains” (containing 146 amino acid residues each). These chains have differing amino acid sequences, but combine to form a three-dimensional structure (gene).
Different mutations in these genes (4 polypeptide chains) result in the four main types of sickle cell disease. These are:
- Haemoglobin SS disease: This is the most common variation of the disease and occurs when a child inherits two copies of the haemoglobin S gene (Hb SS) from both of their biological parents. This type is the most severe variation of the condition where the worst symptoms are experienced more frequently.
- Haemoglobin SC disease: The second most common variation of the disease occurs when a child inherits an Hb C gene from one biological parent, and the Hb S gene from the other. Symptoms of anaemia are less severe than those of the Hb SS variation, but a sufferer will display similar overall symptoms.
- Haemoglobin SB+ (beta) thalassemia: This variation of SCD affects the beta chain gene production by reducing the size of the RBC, and thus restricting the production of beta protein in the blood. A child will inherit the Hb S gene for this variation of the condition to occur but will not typically experience severe symptoms.
- Haemoglobin SB 0 (Beta-zero) thalassemia: This variation also affects the beta chain (globin) gene and displays similar symptoms to Hb SS anaemia, but often in a more severe capacity, and with a poorer outlook for treatment management.
Rarer types of sickle cell disease with less severe symptoms are:
- Haemoglobin SD
- Haemoglobin SE
- Haemoglobin SO
- Sickle cell trait
Other Articles of Interest

Stroke
We all know that a person having a stroke is in a serious and life-threatening situation, but do we really know what to do in the event of an emergency? Here's all you need to know...

Heart Attack (Myocardial Infarction or MI)
A heart attack can be a scary occurrence for you or someone you love. Take a look into the causes, treatment and symptoms for a heart attack so that you know what to do if it occurs...

Stress
Stress can affect everyone differently. It is your body's biological response to a certain situation. It is important to know how to deal with stress in order to develop effective coping mechanisms...