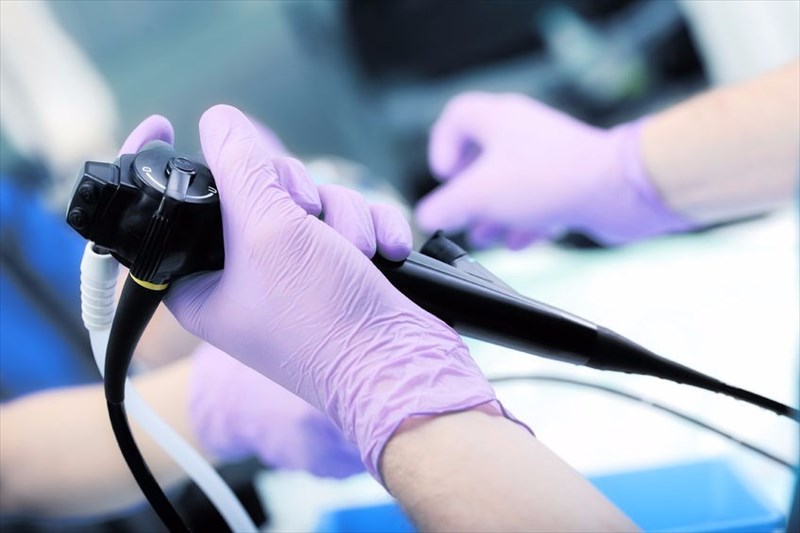
Endoscopy (overview)
An endoscopy, commonly referred to as “a scope” is a non-surgical procedure that is used to examine an internal organ or tissue (for instance in the digestive tract) in detail to determine if there are any problems and may be used to carry out procedures or minor surgery without having to make large incisions. Specialised instruments are used during the procedure to view and operate on the internal organs and vessels of the body.
An endoscope is a thin flexible tube with a camera and a light attached to it. It is inserted through a small opening in the body such as the mouth, and in some instances a small cut (incision).
There are many types of endoscopy procedures which are generally categorised by the area of the body needed for examination. A specialist will generally use an endoscope procedure to view high definition images (or video) of the body on a colour TV monitor (or screen) as a way to help determine a cause of problematic symptoms, as well as make a diagnosis for treatment. Some endoscopes are passed into the mouth and throat (upper endoscopy), while others can be passed into the colon (large intestine) and through the rectum (sigmoidoscopy or colonoscopy) to examine other areas too.
Endoscopic retrograde cholangiopancreaticography (ERCP) is another form of endoscope procedure which allows for images to be taken of the gallbladder, pancreas and other related structures. An endoscope ultrasound (EUS) combines an upper endoscopy procedure and ultrasound examination to retrieve information and images of specific areas of the digestive tract.
A specialist can also use tongs (forceps) and scissors on the endoscope if they need to remove tissue for biopsy (examination and evaluation). From there he or she will use their findings to diagnose and treat conditions that affect the oesophagus, stomach and small intestine (duodenum).
Many endoscopes use technology called narrow band imaging, which makes use of a special light to also help better detect various ‘difficult-to-see’ conditions. This has been very helpful in detecting precancerous conditions, such as Barrett’s oesophagus.
An upper endoscopy may be performed at an outpatient surgery centre (clinic) or a hospital.
Other Articles of Interest

Gastritis
When inflammation, irritation, or erosion of the protective lining of the stomach occurs, gastritis develops. Find out how to recognise the signs here...

Peptic Ulcers (Stomach and Duodenal)
Peptic ulcers are a commonly seen ailment in a number of people and can result from a number of factors. Find out about the symptoms, treatment and diet here.

Hernia
What is a hernia? What causes a hernia? How serious is it? And how is it treated? We take an in depth look at hernias, the different types and how they are treated...
