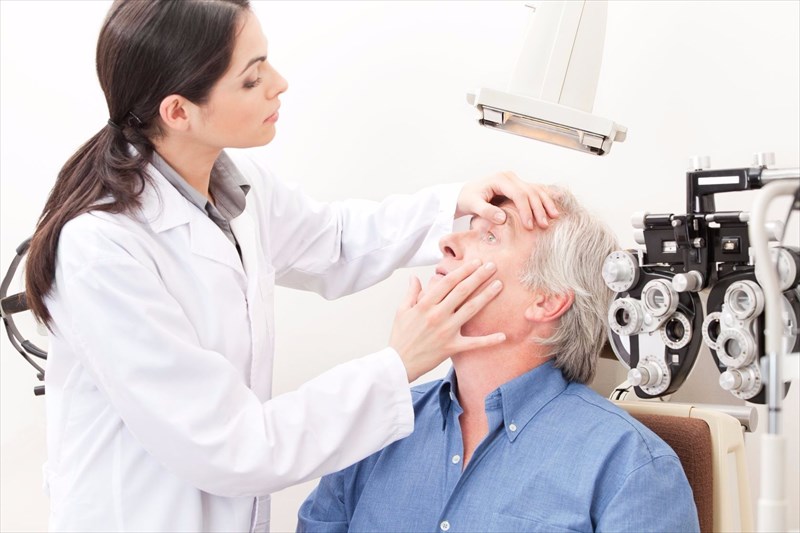
How are cataracts diagnosed?
When to call the doctor
- Severe pain develops
- Double vision or severe loss of vision develops
- Flashes of light occur
- A sudden headache develops
A wait and see approach is not normally harmful if cataracts are small enough not to cause serious symptoms (advanced vision changes). If any noticeable symptoms develop, a medical specialist can also monitor the cataract/s until they are deemed appropriate to treat. However, any cataracts which are noted in children should be treated as soon as possible.
Who to see?
Medical professionals who can evaluate problems associated with vision, such as cataracts include:
- Ophthalmologists (a specialist in medical and surgical eye problems – anatomy, physiology and disease of the eye)
- Optometrists (service-related eye care professional)
- Family physicians or general practitioners (GPs) and physician assistants
- Nurse practitioners
- Internists
- Paediatricians
For detection, diagnosis and treatment, it is best to seek out the professional assistance of an ophthalmologist who can appropriately administer medical care for cataracts.
What to expect during a consultation
A doctor will conduct an evaluation of symptoms through a discussion and an eye examination. A doctor may ask a series of questions to help determine the nature of symptoms and also establish any associated underlying causes. A full medical history (including family health history) will also form part of the discussion.
Questions which can be asked may include:
- How long ago were symptoms first noticed?
- Are symptoms consistently experienced or do they tend to subside?
- Have symptoms worsened between the time they began and this consultation?
- Has a surgical procedure ever been performed on the eyes? If so, what? Were there any complications?
- Have radiation treatments ever been used to the head or neck?
- Have problems with bright light been experienced?
- Have symptoms impacted driving or reading capabilities?
- Have symptoms impacted your ability to do your job effectively, attend school or perform certain activities?
- Have any eye problems ever been diagnosed? If so, what and how long ago?
- Are any medications currently being taken? If so, what and for how long have they been used?
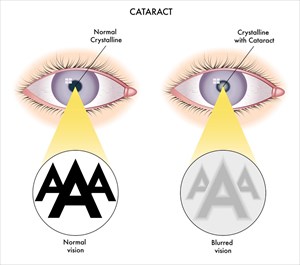
- Visual acuity test: A doctor will use an eye chart (or other viewing device) to assess how well a series of letters, which become progressively smaller, can be read. Each eye is tested one at a time, covering the other. This test usually helps to determine signs of visual impairment.
- Slit-lamp examination: This test allows the doctor to assess structures at the front of the eye using magnification (a slit lamp microscope). The microscope produces an intense line of light which illuminates the iris, cornea and lens, allowing for small sections to be seen with ease. This makes it easier to determine any abnormalities within these eye structures.
- Retinal exam: Dilating eye drops will be placed in the eye/s in order to dilate (open up) the pupils. By dilating the pupils, the doctor will be able to examine the retina with a little more ease. A slit lamp or ophthalmoscope will be used to examine the lens of the eye and determine the presence of cataracts or other abnormalities.
During any examination, the doctor is likely to examine the entire eye to determine any possible signs of abnormalities, and not just cataracts. This is to ensure that there are no other underlying conditions or eye diseases causing symptoms which are compromising visual capability.
The doctor will note pupillary responses and eye movements during examinations, and also conduct a fluid pressure measurement inside the eyes (tonometry – intraocular pressure or IOP) using a tonometer. This test is usually a painless puff of air which is applied to flatten the cornea of the eye and take a measurement of the inside eye pressure.
A doctor will also make note of glare sensitivity and evaluate colour perceptions. All evaluations will be able to confirm the presence of a cataract and also rule out (or confirm) any other suspected medical conditions that can result in a similar set of symptoms affecting vision.
A doctor will also wish to look at any prescription glasses or contact lenses being used, so it is a good idea to bring these along to the consultation.
