- Wisdom Teeth Removal / Impacted Tooth Extraction
- Why do I need to have my wisdom teeth removed?
- How do I prepare for my wisdom teeth extraction?
- During the procedure of wisdom teeth removal
- After the procedure of wisdom teeth removal
- The different types of wisdom tooth impactions and what they mean
- FAQ about wisdom teeth removal
Introduction to wisdom teeth removal
The removal of wisdom teeth is a procedure that involves one or more (there are generally four wisdom teeth, although this is not always the case) being surgically removed. Your wisdom teeth are permanent adult teeth, often referred to as third molars, found at the back of your mouth and are located at the top and bottom corners.
If your wisdom teeth do not have room for growth they may either come in skew or not erupt through the gums like your other adult teeth did, this is known as impaction. Impacted teeth can often be painful or cause dental issues such as infection and the teeth will have to be removed (pulled). A dentist or oral surgeon is likely to perform the surgery.
Oral surgeons and dentists will often recommend that your wisdom teeth are removed even when they are not causing any issues as dental problems arising in the future are often inevitable because of these teeth.
What are my wisdom teeth?
Your wisdom teeth are your third and the last molars located on either side of your lower and upper jaws. These are the final adult teeth to erupt and typically appear when you are in your late teenage years or during your early twenties.
Why do I need wisdom teeth if they have to be removed?
Some anthropologists believe that our wisdom teeth are an evolutionary result of the diet of our early ancestors which consisted of more rough foods like nuts, meats and roots. These foods often required more chewing and therefore resulted in more wear than we experience today. With our more modern diets consisting of softer foods and the aid of eating utensils to help cut our food into bite size portions, the need for these extra teeth has become almost non-existent.
Experts believe that the reason why wisdom teeth result in a number of issues is due to the evolutionary changes humans have undergone. The most significant of which is the expansion of the human brain, as a result, our jaws have had to constrict and become narrower in order to still be able to connect with the lower portion of our skulls. Therefore, we no longer need these teeth.
Some people are, therefore ‘evolving’ to have one or more of their wisdom teeth ‘missing’.
Why are they called wisdom teeth?
These third molars were originally referred to as the ‘teeth of wisdom’ in the 17th century and were referred to as ‘wisdom teeth’ from the beginning of the 19th century onwards.
These teeth usually erupt or appear considerably later than the other teeth (normally when you are somewhere between 17 to 25 years old as opposed to your permanent adult teeth which are usually fully developed by the age of 12 or 13), as such, you are seen as a young adult and ‘wiser’ than you were when your other adult teeth emerged in childhood. It is for this reason that linguists believe that the third molars were termed the ‘teeth of wisdom’ and later ‘wisdom teeth’.
In more recent times, scientists have added some truth to the idea of the third molars appearing when you are indeed ‘wiser’. Recent research shows that our brains continue to develop through adolescence with some experts suggesting that the brain only stops developing after we have turned 25.
With this in mind, it only makes sense that our ancestors thought these teeth were, in fact, our ‘teeth of wisdom’ as they are a sign of the innocence and carefree days of childhood being behind us and therefore welcome maturity and adulthood with their eruption.
How do I know if I have wisdom teeth?
You will know if you have wisdom teeth when you feel them growing or rather, ‘coming’ in. You can often feel these teeth breaking through the surface of your gums which can feel a little painful. You may be able to feel the pressure of them growing which is accompanied by a dull throbbing in your gum. Most people have four wisdom teeth, each one located at a back corner of your mouth, although some people may be ‘missing’ one or more wisdom teeth which are simply non-existent. Genetics often influence whether or not you get these teeth.
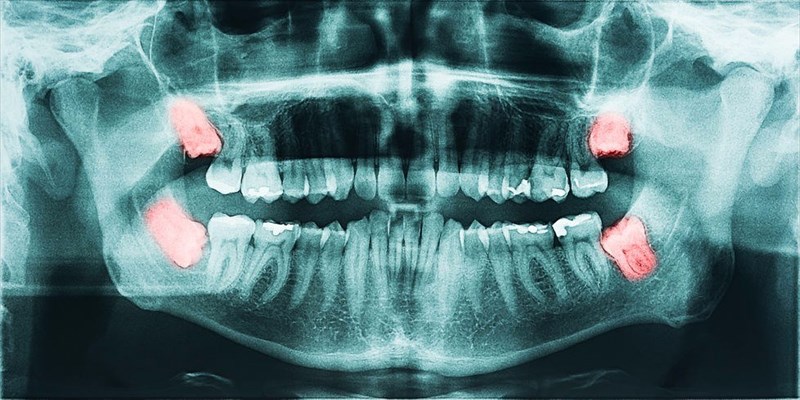
If one of your wisdom teeth is impacted under the gingival tissue, you will not be able to feel or see it and may therefore not even know it exists. As impacted teeth are not visible, your dentist will need to verify their presence through a panoramic radiograph which is a form of X-ray that aids in assessing the angle of the tooth’s growth and its current state of development.
**My Med Memo – An impacted tooth is one that is somehow blocked when it tries to push through the gingival tissue (gum tissue) of the mouth. Wisdom teeth are the most commonly impacted teeth. Therefore, the tooth fails to break through the gum and erupt within its expected window of development.
When to see a dentist
It is advised that you see your dentist for a check-up (part of your annual or bi-annual check-up) if you are suffering from any discomfort or severe pain as a result of impacted wisdom teeth. The dentist will examine your teeth and then advise you as to whether or not they should be removed.
Should your dentist think that you need to have your teeth removed, he or she will conduct an X-ray of your mouth to get a clear indication of the position of your wisdom teeth.
What kind of specialist will remove my wisdom teeth?
An oral or maxillofacial surgeon will typically perform the tooth extraction. These types of specialists are orthopaedic facial surgeons and are able to treat a wide range of dental issues, specifically, the removal of impacted teeth.
Other Articles of Interest

Blood clot
What are blood clots and how do they occur? Learn more about when the formation of a blood clot becomes a little more serious and what to do about it here...

Paracetamol (acetaminophen)
Commonly used for the treatment of mild to moderate pain and fever, paracetamol is widely used around the world. We explore its most common uses, dosages and forms, as well as precautionary factors...

Fever (Temperatures)
Often a sign that something is wrong in the body, a fever is a typical symptom of a variety of different illnesses. What happens when body temperature increases?

