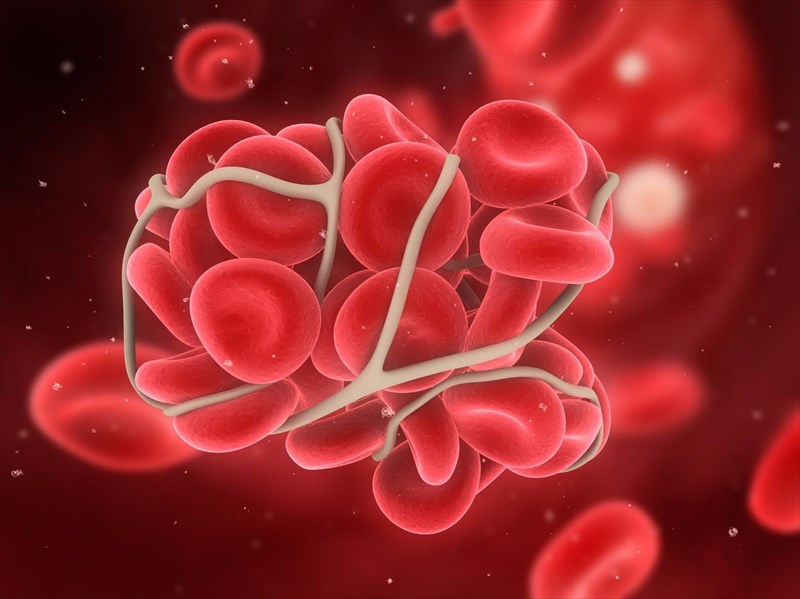
- Blood clot
- Types and causes of blood clots
- What risk factors contribute to blood clots?
- What are the signs and symptoms of blood clots?
- What kinds of blood clot complications can occur?
- How are blood clots diagnosed?
- What treatment procedures are involved in dealing with blood clots?
- Are there ways to prevent blood clots and what are the associated complications?
- Blood clot FAQs
Defining blood clots
What are blood clots?
One of the main functions of blood is to flow through the body’s various blood vessels continuously, ‘feeding’ tissues and delivering oxygen to them. Blood is capable of ‘shutting off’ and forming protective clumps during times of injury as a way to protect the body from further damage. Clotting in this instance can be somewhat lifesaving, slowing down bleeding.
How does blood clot?
When damage occurs in the lining of blood vessels (i.e. arteries, veins and capillaries), platelets (small, colourless cell fragments in the blood) ‘are recruited’ to assist by releasing chemicals (‘clotting factors’) which begin what is known as the ‘clotting cascade’ (or coagulation cascade). This then effectively forms a plug – tiny bits of these proteins attach and stick to the walls of the affected blood vessels, as well as to each other – in an effort to prevent more blood from leaking or travelling any further in the system. The released chemicals also attract more platelets and other cells, which enables the clot to grow.
These clotting factors effectively signal a rapid chain reaction. The protein fibrin is produced, and forms a crosslinked mesh (strands that become tangled up with platelets) which forms a ‘net’ and results in clumps (i.e. a blood clot or thrombus) which subsequently become more durable (i.e. tougher).
Other proteins react to the developed clot and offset other clotting factor proteins so as to prevent the newly formed thrombus from travelling much farther than is deemed necessary. Once the body assesses that damaged tissue has begun healing, the fibrin protein strands begin to dissolve and the normal consistency and function of blood (platelets and cells) resumes.
When clotting becomes dangerous
When abnormal clotting occurs (i.e. clots which form inside blood vessels and not at the site of an incision or cut), blood (naturally in liquid form) becomes gel-like (almost semisolid and ‘sticky’) and effectively restricts the normal flow of blood circulation in the body. Small clots typically dissolve on their own and do not become dangerous, especially if they remain immobile.
Clots that form unnecessarily (e.g. not for repair purposes to prevent loss of blood at times of injury), or are too large, and travel through the system can become problematic and lead to potentially significant health concerns. Blood clots which develop in the deep-seated veins in the body result in a condition known as deep vein thrombosis (DVT), which most commonly occurs in the lower extremities (pelvis, hips or legs).
Blood clots, however, can occur anywhere in the body, and become a major concern when a portion of the clot breaks loose and begins to travel through the bloodstream to various parts of the body. If a blood clot reaches the heart, lungs or brain (in particular), blood flow can quickly become restricted and result in a medical emergency. (1) Conditions which can occur as a result include stroke and heart attack.
It is possible to have a blood clot and be completely unaware of it until signs reach a critical stage or a complication develops. Any signs of a blood clot must be evaluated, diagnosed and treated by a medical professional immediately so as to avoid serious consequences.
Where do blood clots commonly form?
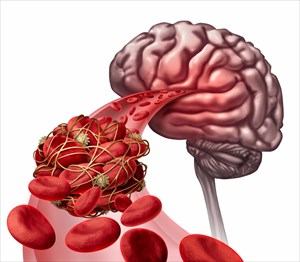
This intricate system flows throughout the body, and thus means that a clot can develop anywhere. A blood clot (or broken off piece of it) in the system forms a kind of bottle-neck, which restricts blood flow and results in clots and the pooling of blood, disallowing the supply to travel further (i.e. preventing it from getting where it needs to be). Clots can form in the superficial veins just beneath the skin’s surface, as well as deeper in the body.
Areas of the body where blood clots can occur include:
- The brain
- The heart
- The lungs
- The arms
- The abdomen
- The legs
Reference:
1. Centers for Disease Control and Prevention. December 2016. Blood Clots and Travel: What You Need to Know: https://www.cdc.gov/ncbddd/dvt/travel.html [Accessed 28.08.2018]
Other Articles of Interest

Stroke
We all know that a person having a stroke is in a serious and life-threatening situation, but do we really know what to do in the event of an emergency? We take an in depth look at the condition...

Deep Vein Thrombosis (DVT)
What is deep vein thrombosis? Here we break down how and why the condition occurs, as well as the basics of the deep venous system structure.

Heart Attack (Myocardial Infarction or MI)
A heart attack can be a scary occurrence. Take a look into the causes, treatment and symptoms for a heart attack so that you know what to do should it happen to you or a loved one.
