- Alopecia Areata (non-scarring hair loss)
- Hair and its stages of growth
- What commonly causes alopecia areata (non-scarring hair loss)?
- Alopecia areata patterns
- Understanding the different types of alopecia
- Signs and symptoms of alopecia areata related hair loss
- How is alopecia areata diagnosed?
- How is alopecia areata treated?
- Coping with alopecia areata (hair loss)
- What research is being done to potentially cure alopecia?
Which doctor to see regarding alopecia areata
- General practitioner (GP)
- Dermatologist
- Endocrinologist (for hormone-related hair loss)
What to expect at a doctor's consultation for hair loss
Symptoms of alopecia areata are fairly distinctive, making a diagnosis quite simple to make purely by sight (during a physical examination), along with a full medical review (including a family medical history) and symptom discussion.
Some questions which could come up during the discussion include:
- When did you start to notice changes in the condition of your hair?
- Have these changes included things like hair breakage, hair shedding or poor growth?
- How long ago did you experience noticeable loss of hair and the development of patches?
- Have you experienced any of the mentioned hair changes and loss of hair before?
- Do you know of anyone in your immediate family that has experienced similar hair related problems?
- Are you taking any medications, supplements or illicit drugs? If so, what and for how long?
- Have you tried anything that has seemingly improved hair loss related symptoms?
- Have you tried anything that has appeared to worsen your hair loss symptoms?
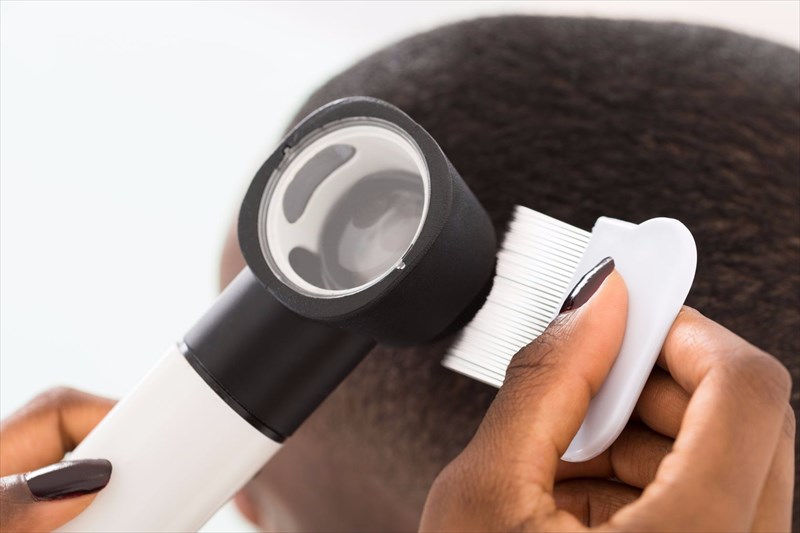
During an examination, a doctor will evaluate the degree and pattern of hair loss, as well as check the hairs around the affected areas under a microscope. Don’t get a fright if a doctor gently tugs on a few hairs during the examination. This is called a pull test, and is merely to determine the current stage of the shedding process. A few hairs may come loose, and these will be analysed microscopically (as a hair sample). This process is known as light microscopy. Hairs trimmed at the bases can also be analysed microscopically, providing clues to possible disorders of the hair shaft.
A doctor may recommend a skin biopsy (a small sample of skin in the affected areas, or from a few hairs that are plucked at the root will be removed for analysis) if a diagnosis is not entirely a straightforward one. A scalp sample will help a doctor to potentially rule out other possible causes of hair loss, such as a fungal infection (like tinea capitis).
Blood tests are another option if he or she wishes to either rule out or diagnose another possible autoimmune disease or health condition like an overactive or underactive thyroid gland (hyperthyroidism or hypothyroidism). The nature of symptoms being experienced will help guide a doctor as to which type of autoimmune or health condition to test for.
On the list to check for is likely to be the presence of one or more abnormal antibodies (or antinuclear antibodies). This generally indicates an autoimmune condition of some kind. C-reactive protein and erythrocyte sedimentation rates (both of which help to detect inflammation in the body), iron levels, testosterone, thyroid hormones, as well as follicle stimulating and luteinising hormones will also likely be checked from the blood sample (taken via a vein in the arm). More appropriate testing can help to determine the specific condition concerned.
