- Alopecia Areata (non-scarring hair loss)
- Hair and its stages of growth
- What commonly causes alopecia areata (non-scarring hair loss)?
- Alopecia areata patterns
- Understanding the different types of alopecia
- Signs and symptoms of alopecia areata related hair loss
- How is alopecia areata diagnosed?
- How is alopecia areata treated?
- Coping with alopecia areata (hair loss)
- What research is being done to potentially cure alopecia?
Treatment for alopecia areata is not always prescribed as the condition is considered benign (i.e. having no harmful effects) and remissions and recurrences are common. When treatment is administered, it is aimed at controlling hair loss as much as possible, as well as stimulating regrowth. Sometimes, treatment involves measures to hide hair loss, especially for those particularly distressed by their condition.
There is no cure for this condition as yet, but it is considered treatable. That said, how effective treatment is, varies from person to person. Some individuals experience regrowth without any medical intervention within a year. Others may try various treatment options before seeing results.
Some may not experience results at all. Regrowth is also often temporary (while in spontaneous remission), but recurrence is a real possibility, so hair loss can be experienced again.
The unpredictable nature of alopecia areata means that it is difficult to gauge how treatment will work and if it will be successful in the long term. No treatment has yet been developed that can comfortably predict an outcome or confidently impact the course of this condition. The best anyone can do is try the options that are available. Results can be achieved, even if only temporary.
Treatment options may involve the following:
Medical intervention for hair loss
1. Topical treatments
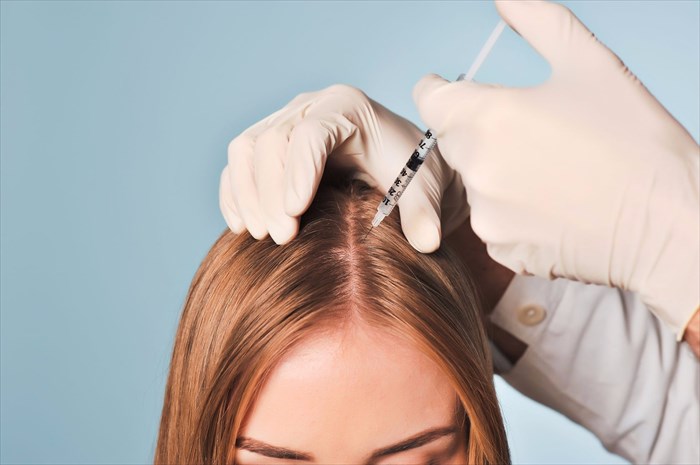
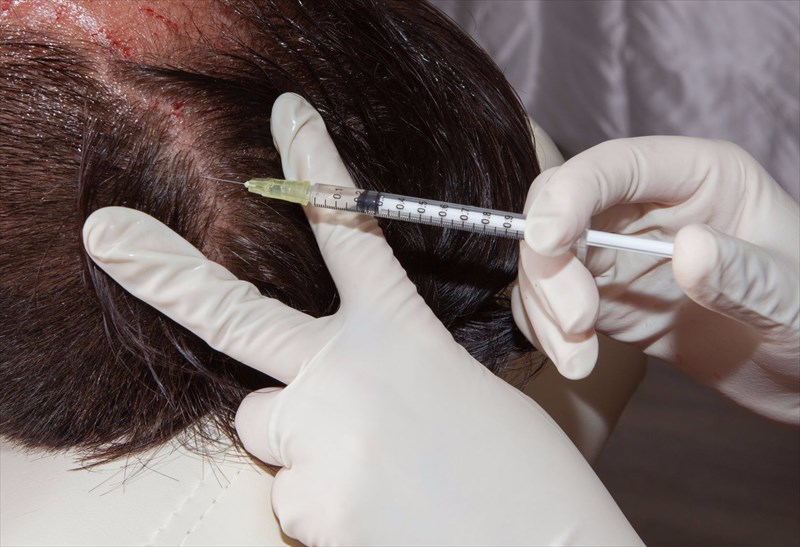
The administration of intralesional steroid injections (anti-inflammatory medications which can help to stimulate the hair growth cycle and suppress the immune system – often given every 4 to 6 weeks).
Widely used as a first-line treatment for alopecia areata, injections are seemingly preferred over topical corticosteroids for use in localised alopecia (with less than 50% hair loss). Those with extensive, long-standing or conditions which have progressed rapidly generally appear not to respond as well in terms of regrowth success. If no improvement is seen after 6 months, a doctor may recommend discontinuing this treatment option. Studies have shown the best regrowth success for patients with patchy conditions (with up to 92% of subjects showing favourable results), and alopecia totalis (up to 61% of subjects showing positive results) within 3 months of treatment. Regrowth can still be observed with some success thereafter, persisting for between 6 and 9 months following just one injection.
Injections are given intradermally (i.e. injected into the dermis, just beneath the epidermal skin layer) so as to achieve a longer absorption time (compared to injections given subcutaneously or in the muscle). The most commonly used synthetic corticosteroid is a Triamcinolone acetonide suspension (Kenalog), which is generally well tolerated by patients.
Lower injection concentrations are favoured for the facial area so as to reduce the risk of possible steroid skin atrophy (a thinning of the skin as a result of a reduction in dermal and epidermal thickness, a regression of sebaceous glands, subcutaneous fat loss, as well as atrophy of the muscle layer). Injection sites may be spread out, covering affected areas (at least 1 cm apart).
Injection side-effects are generally mild, the most common being a little pain at the injection site. Some skin atrophy may also be experienced. If this occurs, a doctor will likely reduce the concentration of the corticosteroid for future injections.
Minoxidil (Rogaine)
A doctor may prescribe a medicated topical treatment (available in liquid or foam form), known as minoxidil (Rogaine) which is to be applied and rubbed into the scalp. It is generally recommended that this be done twice a day. Originally this medication was only really used for the treatment of hypertension (high blood pressure), and was discovered to be beneficial for hair loss completely by accident. A side-effect of the medication seen in many was the stimulation of hair growth, even in unexpected or unwanted areas of the body.
The medication helps to stimulate hair growth (by increasing blood flow), speeding up the natural growth cycle process, and can be used by both males and females. The treatment also helps to slow the rate of potential hair loss. Results are most often noted at about 16 weeks, but it will be advised that applications be continued in order to retain any benefits.
Many consider this medication to be helpful, but only marginally effective when it comes to successfully treating hair loss. This may be because the treatment process does not have any real impact on the hormonal processes associated with hair loss. Thus, any results achieved can only be temporary and last as long as the treatment is active.
Minoxidil does come with side-effects which include unwanted hair growth (sometimes on the face or hands), some irritation to the scalp, and in some instances, a rapid heart rate (tachycardia).
Contact immunotherapy / topical immunotherapy (topical diphencyprone)
This is another technique that can be used in treating alopecia areata. This treatment option effectively triggers an allergic reaction on the scalp (allergic contact dermatitis), and in so doing stimulates hair growth by redirecting the immune response away from hair follicles.
A solution is ‘painted’ onto the scalp (often once a week), causing it to become red and scaly. Repeated sessions can help to stimulate regrowth within about 3 months. A stimulated ‘allergic reaction’ does carry side-effects of possible contact dermatitis (a severe rash) and swollen lymph nodes in the neck.
As such, it is usually reserved for patients with diffuse hair loss that have not responded to other forms of treatment and the doctor performing it will monitor all reactions closely to ensure patient safety.
Low-level laser therapy (LLLT)
This technique uses light and heat to stimulate hair growth, and has seen some success in both men and women experiencing hair loss. The treatment targets epidermal stem cells in hair follicles, and works to stimulate viable follicles back into the anagen phase (growth phase).
Photochemotherapy
Hair growth may also be stimulated with a type of radiation treatment known as photochemotherapy, which makes use of ultraviolet light to stimulate blood circulation in combination with the taking of oral medications, helping to stimulate regrowth.
Other medical treatment options include ointments and creams (also shampoos or alternatively prescribed as oral medications) containing corticosteroids.
2. Orally administered treatments
An alternative prescription medication may be recommended for males, known as Finasteride (Propecia). Once again, the medication was stumbled upon due to hair growth side-effects during the developmental stages of the drug, which was being researched for the treatment of enlarged prostate glands.
This is prescribed as an oral medication (in pill form) which helps to slow hair loss and stimulate regrowth in bald patches. The medication inhibits the enzyme (type II 5-alpha-reductase) responsible for converting testosterone into androgen DHT. The drug has been seen to achieve a reduction level of DHT by up to 60% while a person is under treatment. This is what helps to prevent follicles that are more prone to hormonal shrinkage, from being affected, and keeps the hair at its normal shaft size.
The medication (like minoxidil) typically works, showing results, for as long as it is taken. It has not been able to achieve any effect whatsoever in women experiencing hair loss.
Side-effects to note, but that are rarely experienced, include reduced sexual drive and function, and a possible increased risk for prostate cancer.
Other oral medications may also be prescribed for those who are diagnosed with an underlying condition, other than alopecia areata. These will be necessary to treat the associated symptoms and can include drugs that reduce inflammation in the body and or/ suppress the immune system. It may also be determined during the diagnostic process that certain medications may be the underlying cause of hair loss. In this instance, a doctor will look at alternatives where necessary or recommend a discontinuation of use for a short period of time (at least 3 months).
Medicated treatments can help to reduce the likelihood of further hair loss (by stimulating regrowth from viable follicles), but are not a guaranteed preventative means. No medication has thus far been able to achieve results from follicles that have become inactive.
3. Surgery
Where hair loss is more permanent, particularly at the top of the head, hair transplantation or restoration surgery may be considered. A surgeon will make the most of healthy hair that remains and remove tiny (minuscule) plugs of skin from the back or sides of the scalp (this contains follicles that are viable as they are DHT resistant). Each plug contains a few hairs and will be implanted into the bald patches (on the scalp). An average of about 15% of implanted hair follicles grow in groups of between 4 and 5 hairs.
The procedure does not give a person additional hair as such. The affected individual still effectively has the same amount of hair that they did before the procedure, but the surgery does help with distribution of hair and in that respect, helps to correct the appearance of hair loss.
Medications may be prescribed before and after the transplantation procedure as a way to help improve the end result. Such procedures are expensive and can be painful for the patient concerned. Scarring and infection are some of the main risk factors associated with this type of surgery.
4. Hairpieces and wigs (cosmetic camouflage)
A doctor may suggest the use of hair pieces or wigs as either an alternative to medical treatment options or during the initial stages of treatment, in the time period before regrowth is achieved.
Quality hair pieces and wigs, made from both human and synthetic hair, are widely available and can be used in ways that help to achieve a natural-looking result, both for temporary or permanent hair loss. Hair pieces can be attached to the scalp in various ways with choices of glue, tape or metal clips.
It is advisable not to consider hair pieces which involve weaving, sewing or braiding to existing hair, as this can lead to more permanent hair loss.
Some medical insurance organisations may cover the cost of hair pieces and wigs should they be required as a result of various hair loss related medical conditions, including alopecia areata. A medical note will be required from a treating doctor. It is best to contact a medical insurance organisation beforehand to ascertain cost coverage.
Homecare considerations for those with alopecia
Discomfort can be further minimised by taking certain simple care measures into consideration.
These include:
- Wearing protective sunscreen on exposed areas so as to avoid unnecessary sunburn which could further damage the scalp in particular (a sensitive portion of the body).
- Wearing sunglasses (wraparound glasses work well) if hair loss has affected the eyelashes and eyebrows, as this can help to considerably shield the eyes from the sun, as well as protect them from contact with dust and other debris (which can cause irritation).
- If not wearing a wig or hair piece, a scarf or hat can also be worn outdoors so as to protect the scalp from the elements.
- Considering the use of hair care products and styling techniques carefully, and using these with caution. A doctor can recommend the best care products to use. Some styling techniques can help to make hair appear thicker or have more volume. Colour and dyes as cosmetic camouflage should be used with caution as continuous use can lead to more permanent hair loss down the line.
What complications can occur with alopecia areata?
Alopecia areata can sometimes progress to alopecia totalis or even alopecia universalis, wherein hair is lost in other parts of the body, or entirely. Early medical intervention can considerably reduce this risk should a person’s condition show signs of worsening.
In any case, alopecia-associated hair loss is not a life-threatening condition and does not generally increase a person’s risk of developing many other concerning health issues. A person is, however, at higher risk of damage to the skin caused by sun exposure, and thereby an increased risk of developing conditions such as skin cancer (the more skin is exposed and experiences sunburn).
If alopecia universalis develops, a person will lose their eyebrows and eyelashes which normally offer some protection against debris getting into the eyes. Protective eyewear can help to prevent problems from developing and damaged caused as a result. If nostril hair is lost (also due to alopecia universalis), a person is at higher risk of developing frequent respiratory illnesses as bacteria and germs have easier access into the system through the nose. The annual flu shot or pneumonia vaccine are some effective preventative measures one could take in this regard.