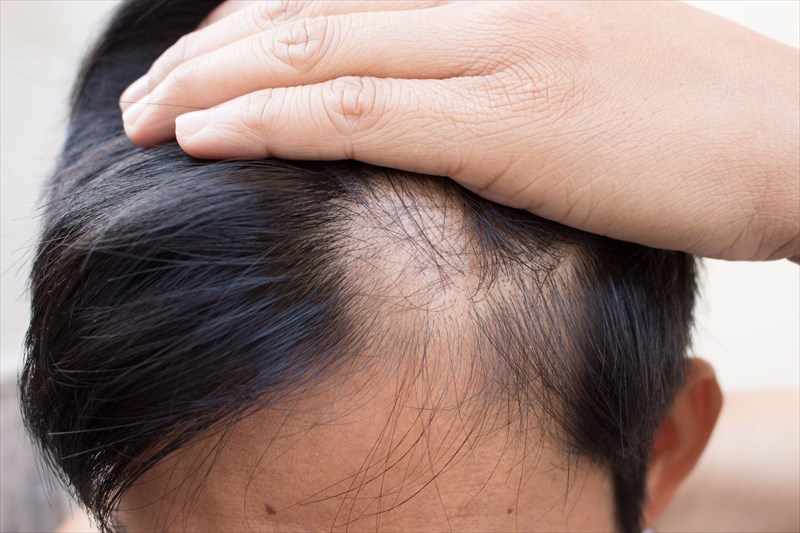
- Alopecia Areata (non-scarring hair loss)
- Hair and its stages of growth
- What commonly causes alopecia areata (non-scarring hair loss)?
- Alopecia areata patterns
- Understanding the different types of alopecia
- Signs and symptoms of alopecia areata related hair loss
- How is alopecia areata diagnosed?
- How is alopecia areata treated?
- Coping with alopecia areata (hair loss)
- What research is being done to potentially cure alopecia?
A misguided immune system response (wherein white blood cells attack the cells within the hair follicles) is generally regarded by experts as the main reason for hair loss. Affected hair follicles begin to shrink once ‘under attack’ from white blood cells. The effect is a dramatic slowing of normal hair production (i.e. shedding and regrowth cycles).
The underlying reasons why the immune system attacks tissues (hair-bearing skin / follicles) and hinders normal hair formation is not entirely known. Research has, however, been able to identify some common factors which may play a role in the development of the disease.
Potential reasons alopecia areata may develop are linked to the following:
- Family history (genetics): It appears that many who experience the effects of this condition, have a close family member with the disease or male-pattern baldness / female-pattern baldness. In fact, at least one fifth (20%) of those with alopecia areata, have a close relative with the condition (4). Those with a history of other autoimmune disorders, also tend to have a family history of the same types of conditions. Genetics in relation to hair loss (i.e. patterns in family history) are also associated with the age and rate at which hair is lost and how much baldness or thinning, also known as miniaturisation (wherein the hair becomes soft, fine and short) has occurred.
- Hormonal changes: Imbalanced hormones can sometimes lead to temporary hair loss and other hair-related changes. Women, in particular, go through changes such as pregnancy, childbirth, and later on, the onset of menopause. During these changes, hormone fluctuations (in the levels of oestrogen and progesterone) can lead to problems with hair loss. Hormonal changes affecting thyroid gland function can also lead to the development of alopecia areata.
- Medical conditions and treatments: Among those with the condition, it is also fairly common for the disease to occur alongside other autoimmune disorders, such as thyroid abnormalities, lupus, rheumatoid arthritis, vitiligo, atopy (a genetic tendency toward developing allergic conditions, such as asthma or eczema), diabetes (type 1) and ulcerative colitis. Surprisingly, medical treatment of such conditions does not appear to correct abnormalities in the immune system when it comes to alopecia areata, and hair loss can still take place. Some medical conditions such as lupus or sarcoidosis (the formation of abnormal nodules / masses consisting of inflamed tissue in the body’s organs) can sometimes cause scarring alopecia (permanent hair loss whereby scarred areas cannot regrow any new hair due to permanent hair follicle damage). Many who have received radiation therapy to the head experience hair loss wherein hair does not grow back the same as it was before.
- Medications and supplements: The treatment of certain medical conditions can result in the development of hair loss as a side-effect. Medications used in the treatment of arthritis, cancer, depression, heart conditions, hypertension (high blood pressure) and birth control can lead to hair loss. So too can vitamin A supplementation when taken in excess.
Stress and environmental factors have been associated with the development of alopecia areata, but have yet to be backed by any substantial scientific research with regards to directly causing the condition. These factors may, however, have a triggering influence in those who are more genetically predisposed to developing alopecia, but to date this has not been conclusively proven.
Reference:
4. US National Library of Medicine National Institutes of Health. 23 January 2010. Management of alopecia areata: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3230136/ [Accessed 20.11.2017]
