- Candida
- Causes of candidiasis
- Signs and symptoms of candidiasis
- Oropharyngeal / oesophageal candidiasis (oral thrush)
- Genital Candidiasis / vulvovaginal candidiasis (VVC) / Candidal vulvovaginitis
- Cutaneous Candidiasis / Candida Skin Infection
- Invasive candidiasis
- What is Candida die-off?
- Candida Diet and Outlook for the infection
Cutaneous candidiasis is the medical term for a fungal yeast infection of the skin, commonly referred to as a candida skin infection. It is estimated that 20 to 25% of the global population are affected by fungal skin infections, making these a rather current occurrence1.
The body is usually able to keep skin infections at bay when a person is healthy. If, however, the immune system is compromised for some reason, an upset in the natural balance of fungi that normally reside on the skin without causing any issues may occur. When this happens, opportunistic species (including candida) multiply and penetrate the skin’s barrier, causing infection. Of the over 200 known candida species, just a few that are commonly found on the skin cause infection. These include:
- Candida tropicalis
- Candida parapsilosis
- Candida orthopsilosis
- Candida albicans – which most commonly causes symptomatic skin infections2
Yeast infections of the skin can occur anywhere on the body but are most common in warm, moist skinfold and creases such as those found:
- In the armpits
- In the groin
- Under the breasts
- In the folds of the buttocks (in infants, cutaneous candida infection can cause diaper / nappy rash).
- In the webbing between the fingers and toes
- Around the edges or corners of the mouth
- In the creases of joints
Infections may also occur in the area around the anus (this is referred to as perianal candidiasis) and on or around the nails (referred to as paronychial and onychial infections).
In overweight individuals, candida infections may spread to various areas where fat rolls have accumulated.
Candida-related skin infections are also common in those with ill-managed diabetes3. This is due to the fact that diabetes interferes with the body’s immune system and suppresses it. This, coupled with blood sugar level spikes in those whose diabetes is not under control, facilitates the overgrowth of yeast which feeds on the excess sugar.
Lactating women who experience nipple injuries due to breastfeeding may also be at increased risk of developing skin or breast-related candida infections. In some but not all lactating women, candida infections may cause sore nipples and a deep, sharp, shooting and/or burning pain in the breasts. When candida infects the breasts, this is referred to as mammary candidiasis.
Candidal infections may also commonly affect those being treated for psoriasis as the treatments for this condition may increase the risk of developing fungal infections4.
Symptoms of candida skin infections (cutaneous candidiasis)
A candidal infection of the skin can cause the following symptoms:
- Intense itching and/or burning sensation in the affected area
- A spreading, red, crusted skin rash (generally starting in the folds of the skin) which may include satellite pustules (little bumps that look like pimples) and overlaying white plaques (hardened areas of skin).
- Sore, cracked skin
- When affecting the breasts, the nipples may appear shiny or flaky
A candidal infection affecting the toenails or fingernails may cause:
- Nail discolouration (greenish-yellow, ochre, or whitish discoloration)
- Nail thickening
- Detachment of the nail from the nailbed
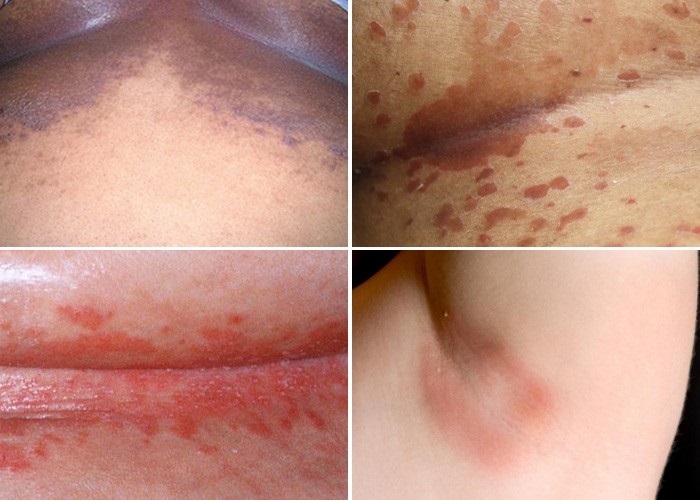
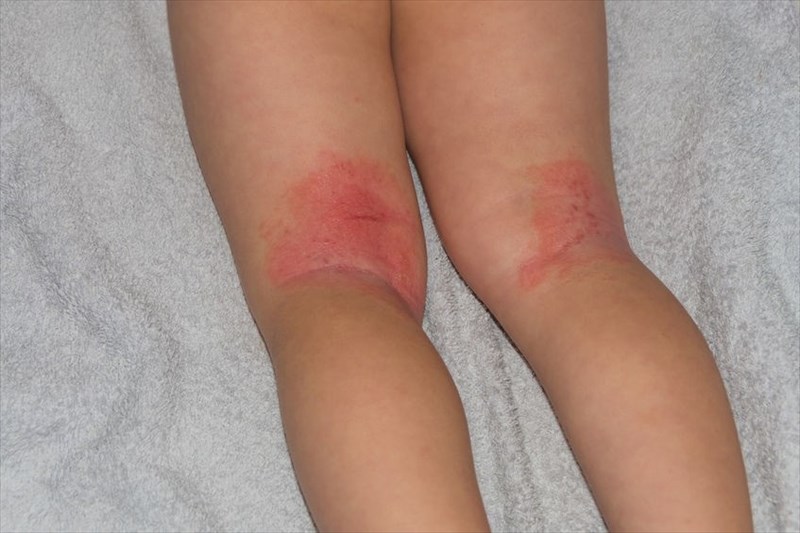
What do candida skin infections look like?
When candida affects the skin, well-defined, red and sometimes itchy patches of lesions in various shapes and sizes appear, generally in the folds of the skin, this is referred to as candidal intertrigo. While the infection generally starts in the folds of the skin, it can spread to the face, trunk or fingertips. On the scalp, crusts may form and can cause hair loss in these areas, infection of the hair follicles may look like pimples.
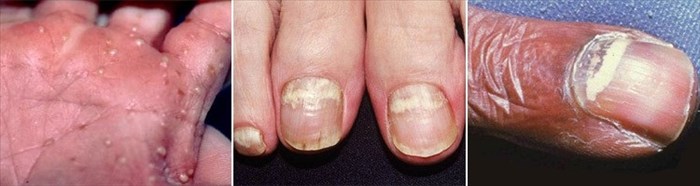
What do candida foot and nail infections look like?
When candida infects the nails the most noticeable symptom is discoloration and thickening. The images below illustrate what candida skin infections of the feet and nails may look like.
Diagnosing a candida skin infection
If you have any of the above-mentioned symptoms, make an appointment with your doctor. He or she will generally be able to diagnose the condition by looking at the skin or nails in the affected area during a physical examination. A sample may be taken for testing.
Adolescents and adults with candida skin infections will generally also be tested for diabetes as these are commonly seen in those with high blood sugar levels. A diabetes test may involve giving a blood and/or urine sample.
Candida skin infection treatment
If it is determined that a skin infection is caused by candida, a doctor may prescribe5:
- An antifungal skin cream, ointment or powder to be used for between two and four weeks. Common first-line therapy includes imidazole (either clotrimazole 1% or miconazole 2% applied twice daily). In those who are allergic to imidazole, nystatin cream may be prescribed.
- For severe symptoms, a single dose of oral antifungal medication (fluconazole – 150mg) or a combination antifungal and cortisone cream may be prescribed.
- For acute lesions: Domeboro®solution, Castellani paint or vinegar–water solutions may be applied twice daily for 5–10 minutes. After these dry a mixture of zinc oxide, talc, and glycerine may be applied twice daily.
- For less serious lesions cleansing with benzoyl peroxide, Castellani stain, or vinegar may be recommended followed by the application of the above-mentioned topical antifungal creams, ointments or powders.
- Chronic lesions may be treated with a rinsing lotion comprised of zinc-talc applied twice a day. Applying an antifungal and corticosteroid combination ointment at night may also be recommended.
Home remedies for candida skin infection
Practicing good hygiene is key when treating a candida infection of the skin. It is vital to keep the skin dry and exposed to air as much as possible. Absorbent powders may assist in keeping moist areas that are prone to perspiration dry.
If a person is overweight, weight loss may aid in the elimination of the issues associated with candida infection. In those with diabetes, getting blood sugar under control and continuing to manage it may also help to clear candida infection and prevent recurrences.
Consuming lactobacillus-containing yogurt has proven to be effective in reducing the candida colonisation of the rectum and vagina in women, as such, there is theoretical evidence that it may be useful in treating various types of candidal infections, including those of the skin.
Plant-based alternative therapies that include the use of garlic, calendula, and the goldenseal herb to treat candida are not usually recommended by medical doctors as there is no reliable data the proves their effectiveness in treating candida at present.
Prognosis (outlook) for those suffering from candida skin infection
While cutaneous candidiasis often resolves with treatment, especially when the underlying cause is addressed, repeat infections are common. In those with weakened immune systems, widespread candidiasis may occur. For this reason, the symptoms of any type of skin infection should never be ignored and rather examined and treated by a medical doctor as soon as possible.
Chronic mucocutaneous candidiasis
Chronic mucocutaneous candidiasis (CMCC) refers to a group of rare syndromes that usually develop in childhood but may only be diagnosed in adulthood. In some sufferers, these syndromes are caused by hereditary genetic defects as a result of the mutation of specific genes that affect the immune system.
These defects affect the ability of the immune system’s lymphocytes / T-cells (i.e. the white blood cells that fight off infection) to defend against candida infections. If the immune system’s antibodies (other immune system cells involved in fighting off foreign bodies) are functioning the body may still be able to fight off infections. However, in some individuals both T-cells and antibodies are compromised, making it difficult for them to resist infection.
Symptoms of chronic mucocutaneous candidiasis
Chronic mucocutaneous candidiasis symptoms include those experienced with non-invasive Candida infections of the skin, nails, and mucous membranes6. These include:
- Severe, recurrent oral thrush
- Onychomycosis (nail infections that may cause one or more nails to thicken, crack, and become discoloured)
- Vaginitis (vaginal yeast infection also referred to as vaginal thrush that is often associated with an abnormal, itchy vaginal discharge)
- Chronic skin lesions (including a thick, crusted rash that may develop over the face and scalp, often causing hair loss)
The above can be experienced along with autoimmune manifestations, often associated with diseases of the endocrine glands (i.e. the glands that secrete hormones). The most common of which include:
Other non-endocrine related autoimmune manifestations include:
- Autoimmune haemolytic anaemia (a condition that occurs when the sufferer’s antibodies attack their own red blood cells (RBCs) cause them to burst, resulting in a deficiency of oxygen-carrying red blood cells in the body).
- Immune thrombocytopenia purpura
- Autoimmune neutropenia
- Rheumatoid arthritis
Chronic mucocutaneous candidiasis diagnosis
A doctor will usually diagnose a candida infection by looking at the infected area during a physical examination. He/she may take a sample of the infected area for examination under a microscope in order to confirm that Candida is, in fact, causing the infection.
Due to the fact that people without underlying immune system disorders can also develop candida infections, risk factors for these will be explored such as recent antibiotic use or whether a person is diabetic.
If a person with chronic, recurrent candida infections that have not become invasive (i.e. they have not spread to the internal organs) has no evident risk factors, a doctor may suspect that he/she has chronic mucocutaneous candidiasis7 and will order blood tests to check for various genetic mutations in order to confirm the diagnosis.
Chronic mucocutaneous candidiasis treatment
Mucocutaneous candidiasis is treated with antifungal therapy. Fluconazole is often the preferred form of treatment as it is effective, has few side effects and is affordable.
The underlying autoimmune or endocrine disorders associated with the condition will also be treated with replacement therapies (i.e. treatments aimed at making up the deficit of a hormone or substance naturally present in the body).
Prognosis (outlook) for those with chronic mucocutaneous candidiasis
While mucocutaneous candidiasis is a chronic disorder, it can be effectively managed and does not affect a person’s lifespan.
References
1. Kühbacher A, Burger-Kentischer A, Rupp S. Interaction of Candida Species with the Skin. Microorganisms. 2017;5(2):32. doi:10.3390/microorganisms5020032
2. Palese E, Nudo M, Zino G et al. Cutaneous candidiasis caused by Candida albicans in a young non-immunosuppressed patient: an unusual presentation. Int J Immunopathol Pharmacol. 2018;32:205873841878136. doi:10.1177/2058738418781368
3. Rodrigues C, Rodrigues M, Henriques M. Candida sp. Infections in Patients with Diabetes Mellitus. J Clin Med. 2019;8(1):76. doi:10.3390/jcm8010076
4. Pietrzak A, Grywalska E, Socha M et al. Prevalence and Possible Role of Candida Species in Patients with Psoriasis: A Systematic Review and Meta-Analysis. Mediators Inflamm. 2018;2018:1-7. doi:10.1155/2018/9602362
5. Metin A, Genç Dilek N, Gunes Bilgili S. Recurrent candidal intertrigo: challenges and solutions. Clin Cosmet Investig Dermatol. 2018;Volume 11:175-185. doi:10.2147/ccid.s127841
6. Firinu, D., Massidda, O., Lorrai, M., Serusi, L., Peralta, M., Barca, M., Serra, P. and Manconi, P. (2011). Successful Treatment of Chronic Mucocutaneous Candidiasis Caused by Azole-ResistantCandida albicanswith Posaconazole. Clinical and Developmental Immunology, 2011, pp.1-4.
7. Khalsa, K., Yang, Q., Shen, X., Pasha, M. and Celestin, J. (2018). Immunologic characterization of patients with chronic mucocutaneous candidiasis disease. Clinical Case Reports, 7(1), pp.180-185.