- Thyroid Disorders
- Common types and underlying causes of thyroid disorders
- Signs and symptoms of thyroid dysfunction
- What risk factors are associated with thyroid disorder?
- Diagnosing thyroid disorders
- Treatment for thyroid disorders
- Common complications of thyroid disorders
- Outlook for thyroid disorders
How are thyroid disorders diagnosed?
Consultations to detect irregularities with the thyroid involve a thorough medical history and symptom discussion with a medical doctor. A general practitioner (GP) is usually the first medical professional of choice. He or she will assess all symptoms, medical history as well as enquire about specific family history details which may be relevant. A complete physical examination and tests generally follow in order to make a specific diagnosis. Specialised tests may be referred to a hormone specialist (endocrinologist).
1. Hyperthyroidism diagnosis
An overactive thyroid may be diagnosed in the following ways:
- Physical exam: A doctor will look for a slight tremor in the hand, specifically the fingers when open and extended. He or she will also look for signs of overactive reflexes, increased metabolism and eye changes, as well as assess if skin is warm and moist to the touch. A doctor will request a person to swallow to assess the thyroid gland (externally) and check for signs of enlargement, tenderness or bumps in the neck during the process. A pulse rate will also be measured to determine the presence of a rapid heart rate.
- Blood tests: A blood sample will be taken to measure levels of T3 (Triiodothyronine hormone), T4 (thyroxine) and TSH (thyroid stimulating hormone). High levels of T3 and T4 and low or virtually non-existent levels of TSH are indicative markers of an overactive thyroid.
- Radio iodine uptake test: Signs of an overactive thyroid following blood test results may prompt a doctor to recommend this test to look for signs of underlying causes. A small, oral dose of radioiodine (i.e. radioactive iodine) will be given. A doctor will then request follow-ups after 2 hours, then at 6 and finally 24 hours later to assess how much of the substance the thyroid gland has absorbed. This is because iodine collects in the gland normally in order to be used for the production of thyroid hormone. High levels collected may indicate that the thyroid gland is producing T4 in excess. A doctor may then look for signs of hyperfunctioning nodules in the thyroid or Grave’s disease. If levels are low, T4 may be leaking into the bloodstream from the thyroid gland. In this instance, a doctor will investigate thyroiditis underlying causes. The amount of radioactive iodine administered during this test is very small and passes through the body’s system easily without causing any physical harm. This test is not normally recommended for pregnant women.
- Thyroid scan (nuclear medicine imaging): A radioactive isotope (chemical elements also called radiotracers) will be injected in a vein on the inside of the elbow or sometimes in the hand. A person will need to lie down with their head stretch backwards. From there a doctor will use a specialised camera and computer screen to produce and view an image of the thyroid gland (the isotope content will clearly show up ‘hot nodules’ – hyperfunctioning masses). Depending on how long it takes for the isotope chemical to reach the thyroid gland, the process for the scan could take a little bit of time. Some discomfort in the neck may be felt during the scan process once the isotope has been injected. This scan may be done individually or in conjunction with a radio iodine uptake test (in this instance only the orally administered radioactive iodine will be used to produce the image). During the scan, the doctor will check the size, shape, position and function of the thyroid gland, and look for irregularities. It is not possible to distinguish between malignant or benign ‘cold nodules’ (these appear hole-like on the produced image) on a scan. ‘Cold nodules’, however can sometimes represent cancer.
2. Hypothyroidism diagnosis
An underactive thyroid may be diagnosed in the following ways:
- Physical exam: A doctor will assess for physical signs of an underactive thyroid which can be seen, such as dry skin, a slower than normal heart rate and facial swelling.
- Blood tests: T4 and TSH will be measured using a blood sample. Low levels of T3 (triiodothyronine hormone) and T4, and high quantities of TSH are indicative markers of an underactive thyroid and signs that the pituitary gland is producing more TSH than normal in order to stimulate the thyroid gland. An injection of the TSH hormone can help to determine possible abnormalities of the hypothalamus and pituitary gland if it is noted that TSH levels are abnormally low. Levels must be measured accurately so as to determine the correct dosage of medication treatment.
3. Goitres / thyroid nodules diagnosis
If goitres or thyroid nodules are suspected during the physical examination, a doctor may test in the following ways:
- Physical exam: A doctor will request a person to swallow hard during a physical examination to determine the possibility of a goitre or nodule. Nodules typically move in the gland / neck when swallowing and if big enough, can be physically seen this way.
- Blood tests: Measure T3, T4 and TSH hormone levels and determine overactive or underactive function. A doctor will then assess blood sample for antibodies, such as titres of anti-thyroglobulin, TSH receptor stimulating or anti-thyroperoxidase antibodies. The presence of these antibodies can indicate a potential goitre. The TSI (TSH receptor antibody) is normally present in Grave’s disease. Thyroperoxidase antibodies are typically present in conditions of Hashimoto’s and Grave’s disease.
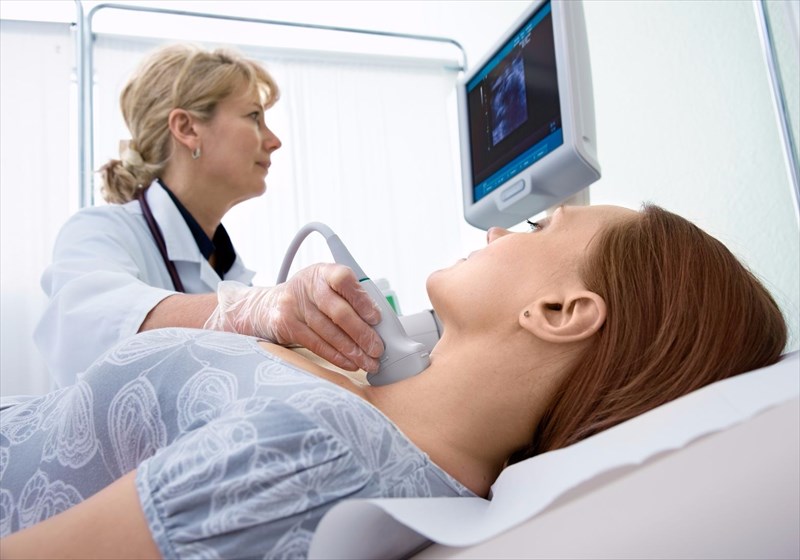
- Ultrasonography: A transducer (wand-like device) will be held over the neck, and using high-frequency sound waves (instead of radiation) to bounce through, will form clear images on a computer monitor showing the shape and structure of nodules. The doctor will assess the thyroid gland size and also detect abnormal masses (goitres and nodules) of any size. A doctor can determine single masses and multiples as well, and also distinguish between cysts (fluid-filled) and solid nodules.
- Thyroid scan or ultrasound scan: Scans may be recommended to evaluate the size and shape of nodules.
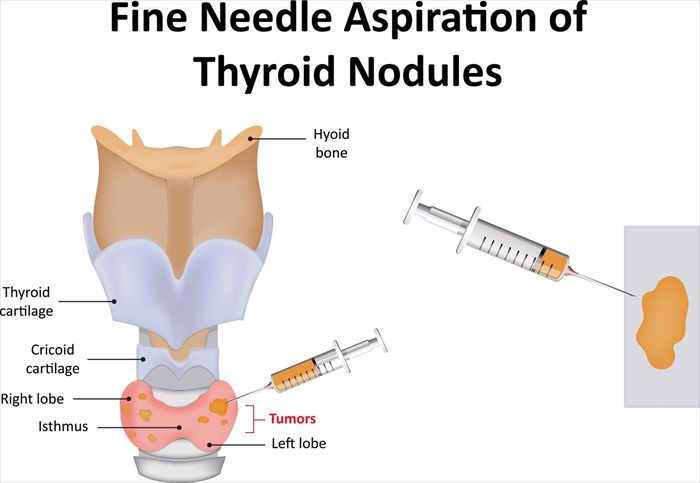
- Fine needle aspiration biopsy (FNA): A thin needle is guided into nodules in the thyroid gland using the aid of an ultrasound scan in order to obtain a sample of tissue or fluid (nodule cells) for testing in a laboratory under a microscope. This test may be recommended in order to rule out the possibility of thyroid cancer. The sample retrieval process can take up to 20 minutes.
4. Thyroid cancer diagnosis
If thyroid cancer is suspected, the following tests may be done:
- Physical exam: Assessed against possible risk factors, a doctor will look for any visible abnormalities or changes in the thyroid during a physical exam. Questions such as whether there has been any exposure to radiation or a family history of thyroid problems (specifically tumours) may come up as well.
- Blood tests: Thyroid function and hormone production levels will be tested, along with the presence of antibodies.
- Imaging tests: A doctor may recommend an ultrasound scan (which helps to visualise tissue consistency), computerised tomography (CT) scan or a positron emission tomography (PET scan) to carefully assess nodules, as well as to determine any signs of cancer which has spread beyond the thyroid gland.
- Fine needle aspiration biopsy (FNA): Cell samples retrieved will be assessed for malignancy.
Who may be involved in the diagnosis process?
- General practitioner (GP)
- Pathologist (specialist in tissue samples)
- Endocrinologist (specialist of the endocrine system)